Full Text
Brodie’s abscess radiologically is a distinct form of subacute osteomyelitis. Infection of bone i.e., osteomyelitis can be radiologically divided into three stages i.e., 1) acute, 2) subacute and 3) chronic. However, in transitional periods, different stages cannot be seperated as there is overlap of radiological findings. In the subacute form, two radiological stages have been described. One of the major forms is bone abscess which is a collection of purulent material surrounded by granulation tissue and reparative sclerotic bone which is a classical finding of Brodie’s abscess.
The most common organism is staphylococcal aureus or streptococcus but any pyogenic organism may be the cause. Occasionally, the pus may be sterile. Histopathologically the abscess material reveals necrotic tissue with an acute or chronic inflammatory infiltrate. Even cystic type of tuberculosis may simulate Brodie’s abscess. Cultures and histopathological findings are needed for scientific evidence and in the management of the patients. Clinically, it is encountered in children of 10-20 years, but it can occur at any age, although uncommon at old age.
The radiological manifestations of the three stages of osteomyelitis on conventional radiology are described in Table 1.
Osteomyelitis results from infection of bone where both trabecular and cortical bone are involved. It may be exogenous and contiguous or endogenous due to hematogenous spread.
Acute osteomyelitis
Table 1: Acute osteomyelitis.
|
Day 1.3: Localized, deep focal swelling.
Day 3.4: Ill defined, extensive swelling, edema, wide subcutaneous planes- deep cellulitis.
Day 8-12: Soft tissue changes are not characteristic. Delicate, linear, unilaminar periostral
Reaction with localized permeative osteoporosis is noted. In some patients, extensive osteolysis may be noted. Untreated this will progress to subacute osteomyelitis.
Conventional radiology shows the findings radiological only after 10 days.
|
Subacute osteomyelitis
Type – I
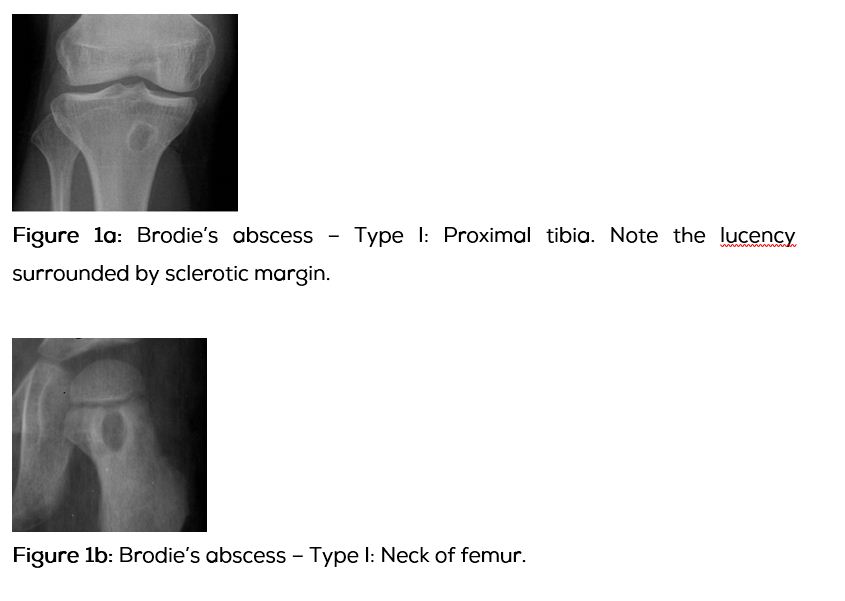
Periosteal reaction may be absent. A well defined lucent area surrounded by new bone formation is noted and is named as Brodie’s abscess.
Type – II
Periosteal reaction is thicker than in acute osteomyelitis. More diffuse and mottled permeative osteolysis is often noted with surrounding new bone and cortical thickening. Untreated this may lead to chronic osteomyelitis.
Chronic osteomyelitis
Radiological findings are described in Table 2.
Table 2: Chronic osteomyelitis – Radiological findings.
|
· Dense cloaking of periosteal new bone.
· Bizarre cortical thickening.
· Sequestrum and involucrum formation.
· Sinus tracts.
· Old fracture or deformity may be noted in some cases.
|
This write up is confined to Brodie’s abscess. In the spectrum of developing Brodie’s abscess, some overlap of radiological findings may be noted between subacute and chronic osteomyelitis.
Radiological appearances of Brodie’s abscess are listed in Table 3.
Table 3: Brodie’s abscess.
|
· A lytic lesion with an oval configuration which is oriented along the long axis of a tubular bone.
· It is surrounded by thick dense rim of reactive sclerosis that fades imperceptibly into surrounding bone.
· A lucent tortuous channel extending toward growth plate prior to physeal closure is pathognomonic.
· Periosteal new bone may be noted.
· Adjacent soft-tissue swelling may be present.
· Occasionally, a small sequestrum may also be noted.
· It may persist for many months and untreated leads to chronic osteomyelitis .
|
Sir Benjamin Brodie was first to described subacute osteomyelitis and reported the abscess in the Tibia. Conventional radiology is adequate but in certain instances, computerized tomography (CT) or magnetic resonance imaging (MRI) may be needed. Radionuclide scan is not always necessary. Positron emission tomography (PET) CT scan is ideal but costly for establishing the diagnosis. Roberts et al. modified Gledhill classification and described in six types (Table 4).
Table 4: Roberts et al. modified Gledhill classification.
|
Type I: Metaphyseal (Figure 1abcd).
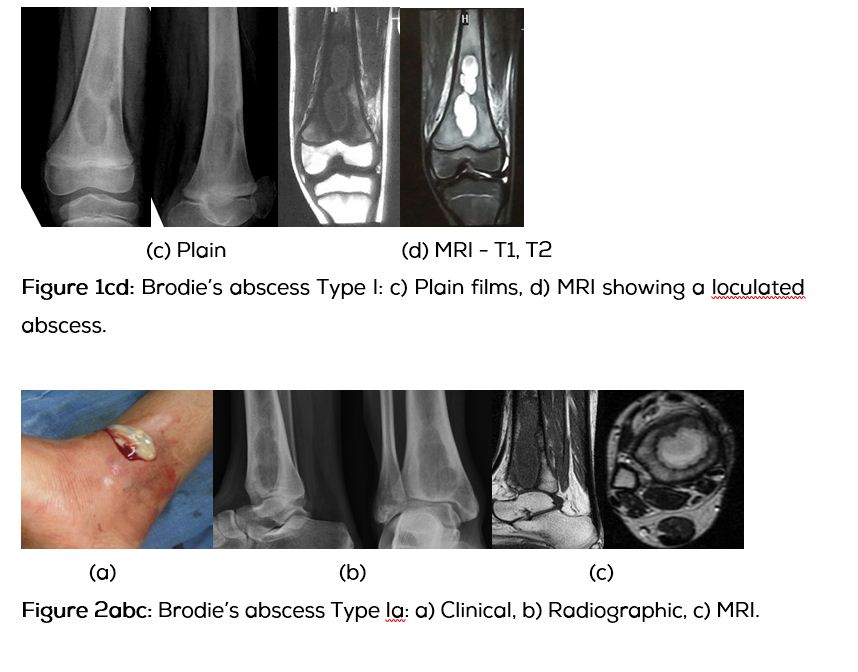
Type Ia: Punched out central metaphyeal (Figure 2abc).
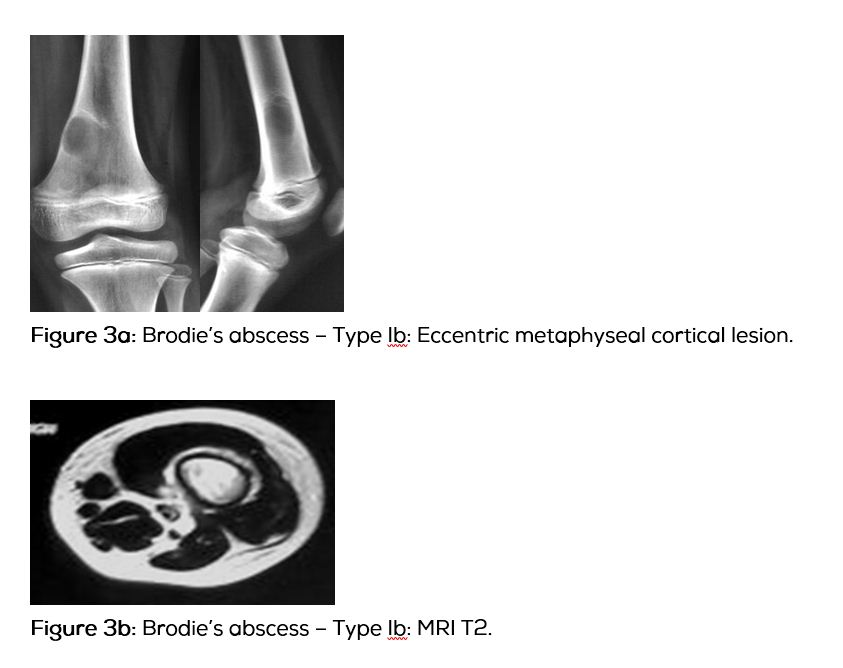
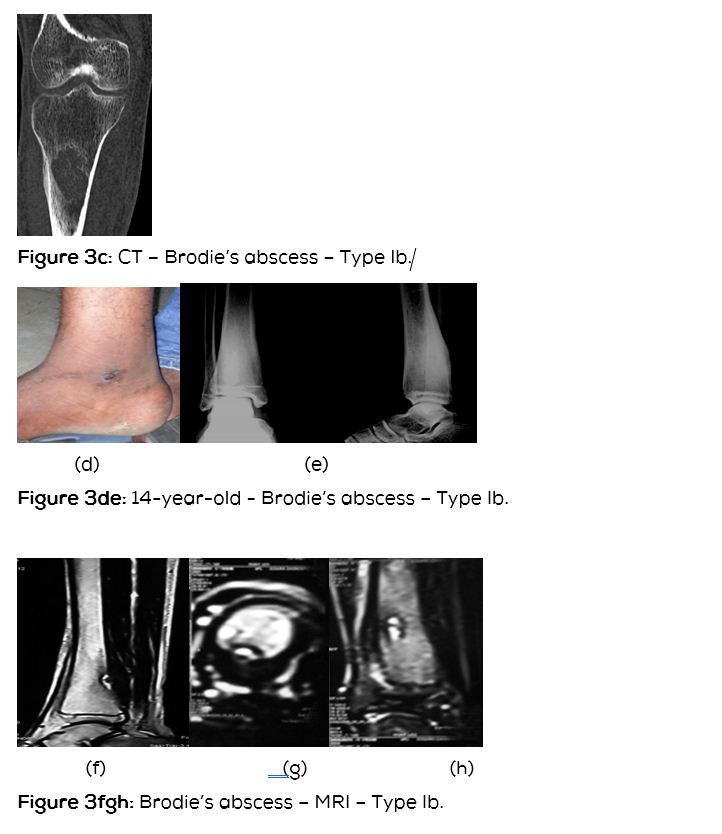
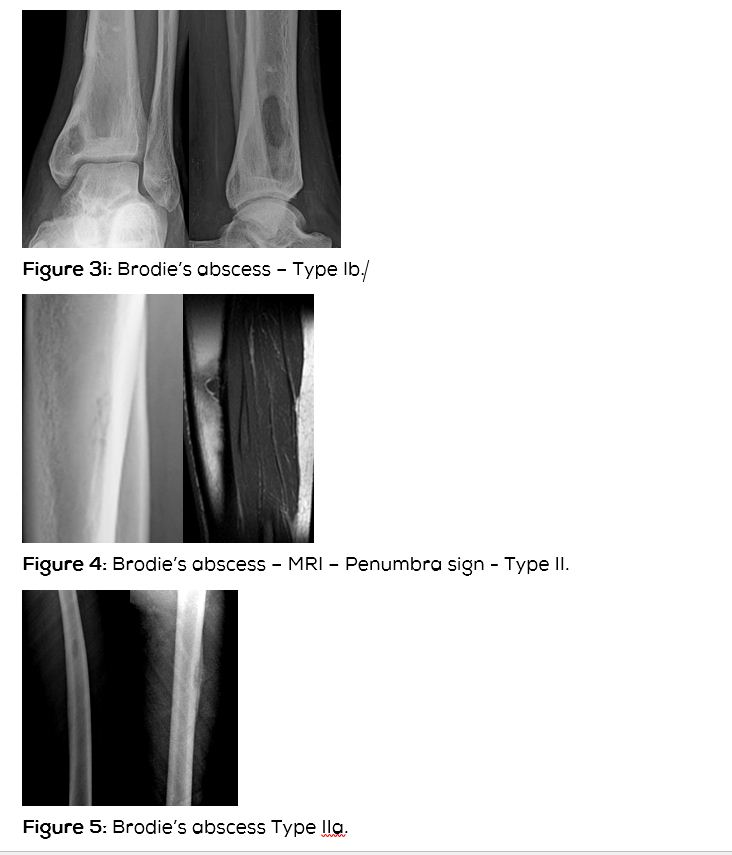
Type Ib: Eccentric metaphyseal cortical (Figure 3abcdefghi).
Type II : Diaphyseal (Figure 4).
Type IIa: Localized cortical with periosteal reaction (Figure 5).
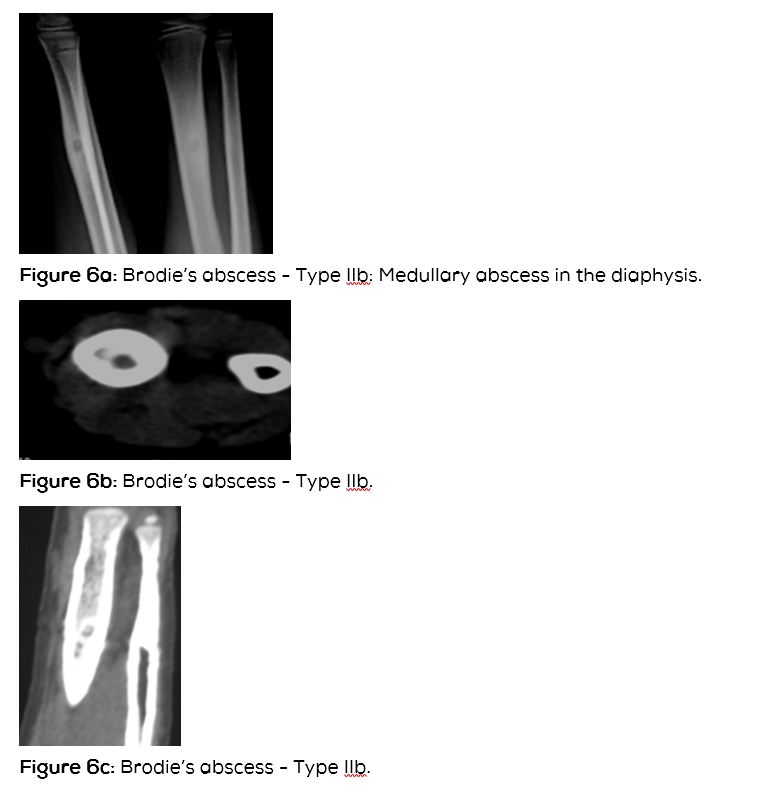
Type IIb: Medullary abscess in the diaphysis without cortical destruction but with onion skin periosteal reaction (Figure 6abcd).
Type III: Epiphyseal.
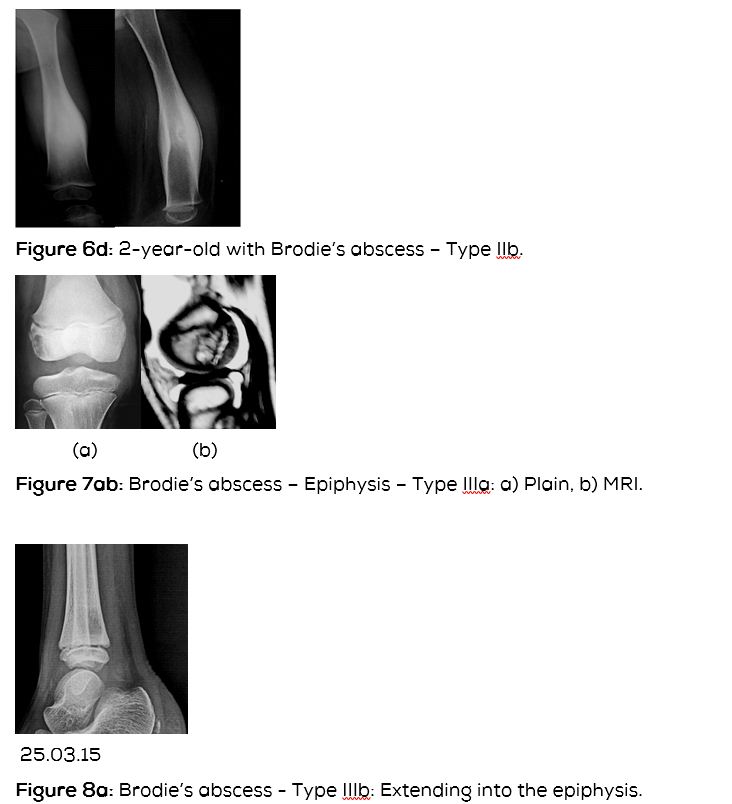
Type IIIa: Primary epiphyseal osteomyelitis (Figure 7).
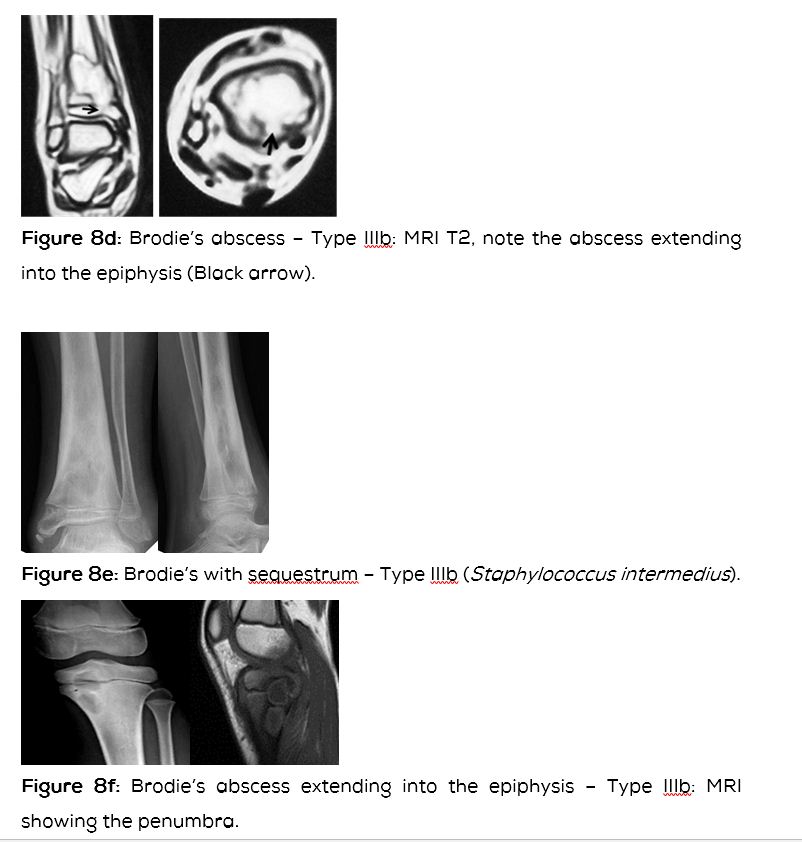
Type IIIb: Lesion involving epiphysis and metaphysis (Figure 8abcdef).
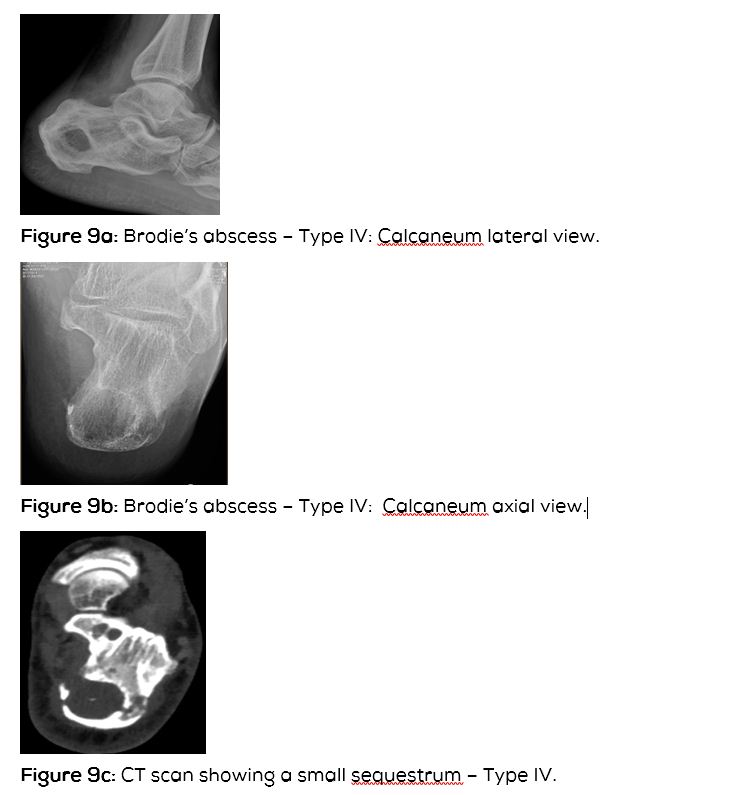
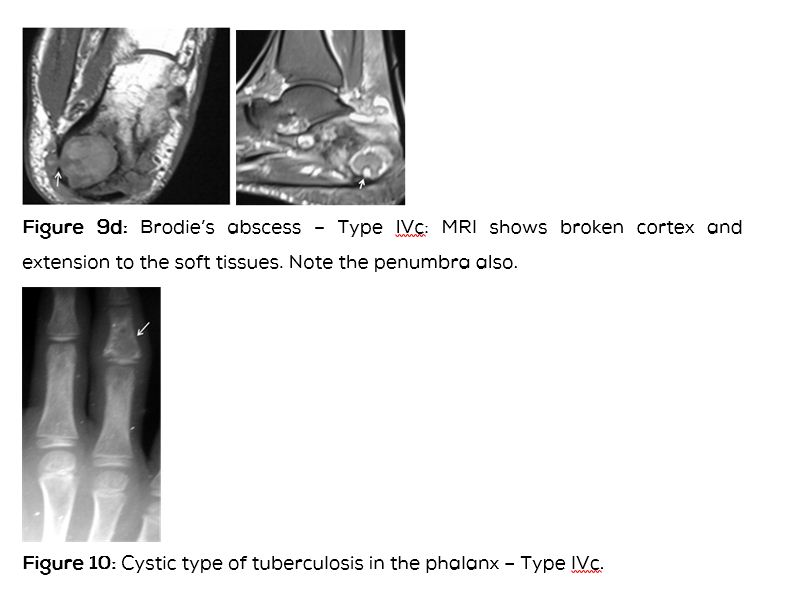
Type IV: Metaphyeal equivalent (Figure 9abcd).
Type IVa: Involves the vertebral body with a lytic process.
Type IVb: Involves the flat bones of the pelvis.
Type IVc: Involves the small bones (Figure 10).
|
This classification may confuse the general radiologist as there is overlap of several features. This appears to be purely academic and of little practical use.
MRI
Whenever there is ambiguity in differentiating Brodie’s abscess from other bone lesions, MR scanning is useful in confirming the diagnosis of Brodie’s abscess. MRI reveals low signal intensity centre on T2 weighted images. A “penumbra sign” is characteristic but is not pathgnomonic as this sign has been observed in eosinophilic granuloma, cystic lesions of bone, etc. This sign shows a rim lining of the abscess cavity with higher signal intensity than that of the main abscess on T1 weighted images. The Stir and T2 weighted MR sequences depict the extent of the infection and can differentiate from other radiolucent bone lesions (Table 5).
Table 5: Abscess characteristics – MRI.
|
• Hyperintense enhancing rim (= hyperemic zone) around a central focus of low intensity (= necrotic/ devitalized tissue) on contrast-enhanced T1WI.
• Hyperintense fluid collection surrounded by hypointense pseudocapsule on T2WI + contrast enhancement of granulation tissue.
• Hyperintense adjacent soft tissues on T2WI.
• Fat-suppressed contrast-enhanced imaging (88% sensitive + 93% specific compared with 79% + 53% for nonenhanced MR imaging).
|
Computed tomography (CT)
CT scan denotes the abscess as well as the surrounding reactive bone and periosteal reaction (Figure 3c). Occasionally, a small sequestrum which is not identified on conventional films may be seen on CT (Figure 9c). It is also helpful in differentiating from osteoid osteoma and other lytic lesions.

Differential diagnosis (DD)
In the imageological DD of Brodie’s abscess, chondroblastoma, fibrous dysplasia, osteoid osteoma, eosinophilic granuloma, stress fracture, ganglion etc., may be considered.
Chondroblastoma
This is a benign cartilaginous tumor involving the epiphysis/ apophysis or epimetaphysis. In majority of the cases calcification is present which clinches the diagnosis (Figure 11).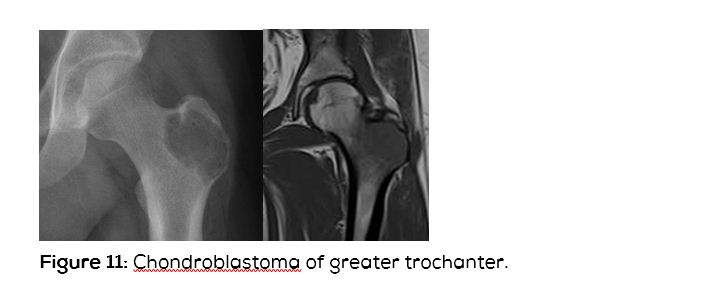
Fibrous dysplasia (FD)
This is fibrous aberration in the development of bone. In the monostotic type of FD, the cystic lesions may simulate Brodie’s abscess (Figure 12).
Osteoid osteoma
This is a benign bone tumor occurring in the cortex, subperiosteal area, subarticular region and in the spongiosa. The spongiosal form does not produce much reactive bone. The nidus is lucent and is less than 1.5cm in diameter. This may simulate small Brodie’s abscess (Figure 13a). A diaphyseal osteoid osteoma may also simulate Brodie’s abscess (Figure 13bc).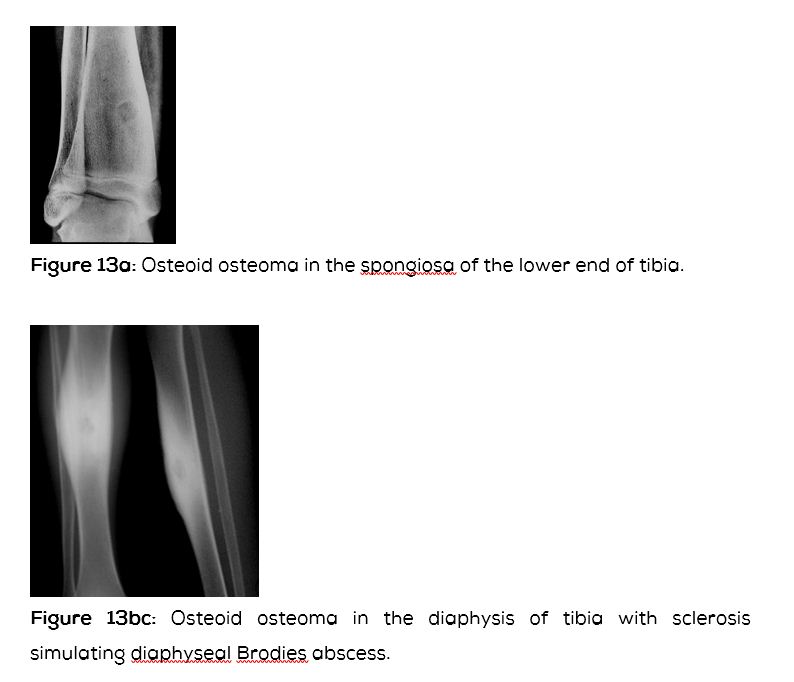
Eosinophilic granuloma (EG)
This is a benign granulomatous bone lesion belonging to Langerhan’s Histiocytosis X. This may be single or multiple. A solitary EG radiologically is a lytic lesion with surrounding sclerosis with bevelled edges. Periosteal reaction may be noted. When it occurs in the tubular bones may simulate Brodie’s abscess (Figure 14abc).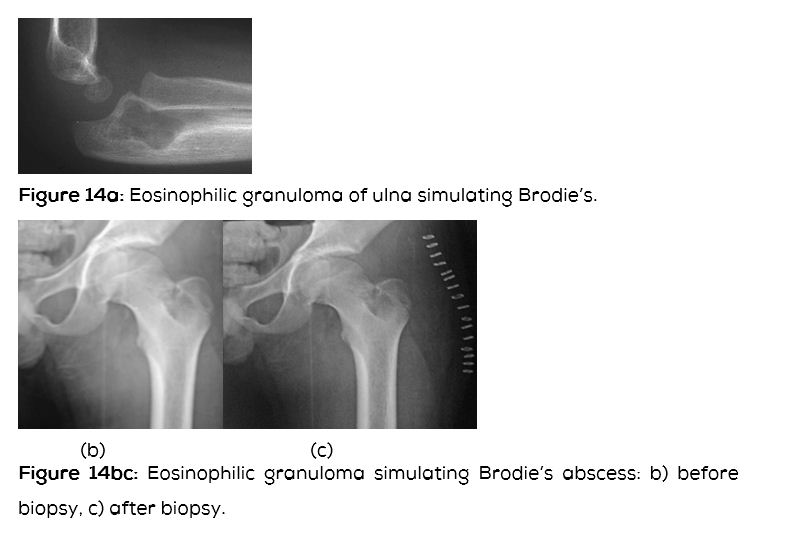
Stress fracture
It occurs in active athletic people, usually in the bones of the lower limb. A cortical lucency is noted with surrounding sclerosis and may simulate Brodie’s abscess (Figure 15).
Ganglion
A ganglion consists of synovial fluid and radiologically is subarticular with a lucency surrounded by sclerosis (Figure 16).
Conclusion
Inspite of extensive antibiotic use Brodie’s abscess is still encountered. The imageological features are classical and to be differentiated from many other lytic bone lesions. These features are well illustrated and should be of use in practice. The classification is mostly academic and is not in practical use in management as there is considerable overlap of the stages.
Acknowledgements
Osmania General Hospital and Nizam’s Institute of Medical Sciences, Hyderabad.
Conflict of interest
The author declares no conflict of interest.
References
1. Afshar A, Mohammadi A. The “Penumbra Sign” on Magnetic Resonance Images of Brodie’s Abscess: A case report. Iran J Radiol. 2011; 8(4):245-248.
2. Brant WE, Helms CA. Fundamentals of diagnostic radiology. Lippincott Williams & Wilkins. 2007; ISBN: 0781761352.
3. Dahnert WF. Radiology review manual. Lippincott Williams & Wilkins. 2002; ISBN: 0781738954.
4. Gaillard F, Weerakkody Y. Brodie’s abscess. Accessed on 14 July 2015 at: htpp://radiopaedia.org/articles/brodie-abscess-1
5. Khoshhal K, Letts RM, Mehlman CT. Subacute Osteomyelitis (Brodie Abscess). Accessed on 14 July 2015 at: http://emedicine.medscape.com/article/1248682-overview#a0101
6. McGuinnes B, Wilson N, Doyle AJ. The “Penumbra Sign” on T1-Weighted MRI for differentiating musculoskeletal infection from tumor. Skeletal Radiol. 2007; 36(5): 417-421.
7. Md.Amanullah F, Ansari S,, Ahmad K. Brodie’s abscess mimicking as of malignancy: case report with radiological features: Journal of Msk. Research. 2013; 16(1):1372001.
8. Miller WB, Murphy WA, Gilula LA. Brodies abscess – Reappraisal. Radiology. 1979; 132(1).