Full Text
Introduction
Bladder carcinoma (BC) is one of the most common urological malignancies. It is the fourth most common cancer in men and eighth most common malignant tumor in women in the Western world [1]. From the data obtained from Indian cancer registry, bladder cancer accounts for 3.9% of all cancer cases in men [2]. The most common histological type of bladder carcinoma is the urothelial carcinoma (UC) and it accounts for 95% of carcinomas [3]. Among the urothelial carcinomas, the squamous differentiation is seen in 20% [4]. In the recent series, pure squamous cell carcinoma of the bladder is an uncommon cause of bladder cancer in the developed world and accounts for 2.7% of bladder cancers [5]. Adenocarcinoma is a rare form of bladder carcinoma and accounts for 0.5-2% of all bladder malignancies [6] and carcinoma rectum is an unusual site of origin for distant metastasis into the bladder and its incidence was only 0.06% [7]. These histologic variant were independent factor for recurrence, aggressiveness, and poor survival with varied treatment modalities. We present here a series of such rare bladder carcinomas.
Case presentation
Case 1
A 55-years-old male came to the Department of Urology with a complaint of dysuria, hematuria with passage of clots and loss of appetite. He had a history of vesicular calculi and open cystolithotomy was done 2 years back. Cystoscopy revealed an anterior wall growth extending into dome with multiple calcifications and necrosis. Radical cystectomy was done. Grossly, an ulceroproliferative growth was present in the dome and anterior wall of bladder, measuring 10×6.5×4cm and infiltrating the muscular layer, perivesical fat and adjacent abdominal wall skeletal muscle. Cut surface of the tumor appears solid and grey white. Histopathologically it was diagnosed as moderately differentiated squamous cell carcinoma with invasion (Figure 1).
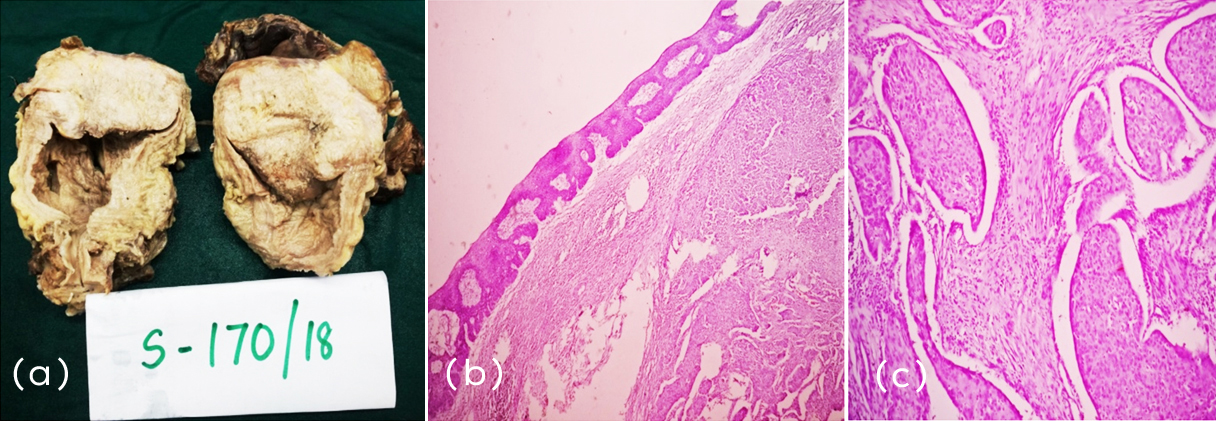
Figure 1: (a) Gross- ulceroproliferative growth in the dome and anterior wall, C/S appears solid and grey white, (b) Squamous cell carcinoma of bladder H&E (4x), (c) Solid nests of squamoid cells infiltrating the muscular layer (40x).
Case 2
A 47-years-old male presented with a complaint of painful micturition, hematuria, foul smelling urine. Cystoscopy showed hypoechoic lesion with superficial papillary projections in the anterosuperior wall of bladder and radical cystectomy with regional lymph node dissection was performed.
Gross examination showed ulceroproliferative growth seen in the dome, posterior and lateral wall of the bladder measuring 7×6×5 cm and infiltrating into underlying muscle and perivesical fat. Cut section of the tumor was friable, grey white and firm. Microscopic examination showed malignant tumor arranged in glands, cords, small nests and sheets with microcystic areas showing tumor cells exhibiting moderate pleomorphism with vesicular nucleus and prominent nucleoli with focal area showing cytoplasmic vacuolation. Large areas of squamous differentiation (40%) seen with areas of necrosis and keratin formation and the tumor was invading into the deep muscularis propria and perivesical pad of fat with nodal metastasis and was diagnosed as high grade infiltrating urothelial carcinoma with squamous differentiation (40%) with regional lymph node metastasis (Figure 2).
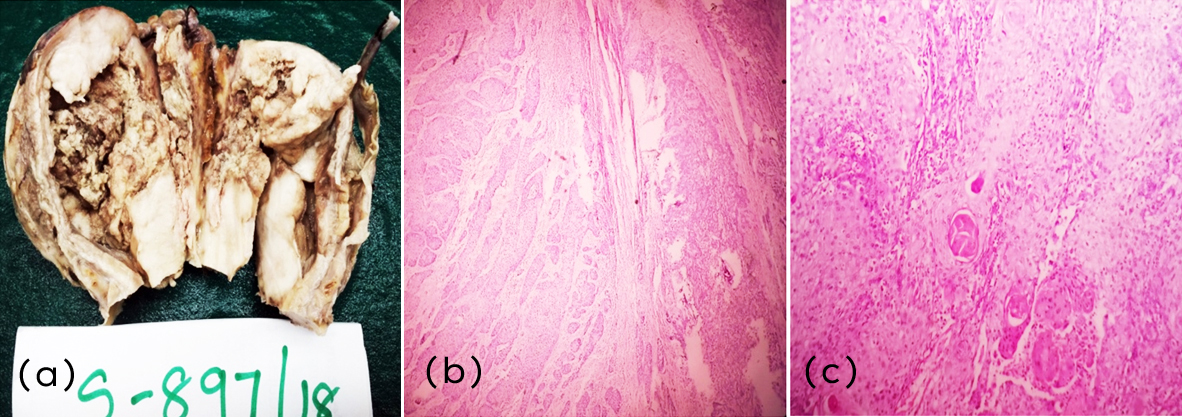
Figure 2: Urothelial carcinoma with squamous differentiation- (a) Gross- ulceroproliferative growth seen in the dome, posterior and lateral wall. C/S appear friable, grey white and firm, (b) Tumor cells are arranged in nests, sheets and cords (4X), (c) Areas with squamous differentiation (40X) H&E.
Case 3
61-years-old male, known case of carcinoma rectum and abdominoperineal resection was done 9 month back, presented with perianal nodule and pelvic mass, oliguria and painful micturition. Fine needle aspiration cytology (FNAC) from the perianal nodule showed signet ring cells, suggestive of metastatic adenocarcinoma. Patient was treated for bladder outlet obstruction, hence Transurethral resection of the prostate (TURP) was performed and it showed features of adenocarcinoma. Immunohistochemistry was performed and showed positivity for CK20, CDX2 and negative for PSA suggestive of metastasis from colorectal primary. PET CT showed positive for metastatic disease. Hence proceeded with total pelvic exenteration with ileal conduit.
Gross examination showed bladder with prostate and soft tissue measuring 19×11×8 cm. Wall of the bladder was diffusely thickened and right and left ureteral resected margin and uretheral resected margin were free of tumor. Microscopic examination from the bladder showed tumor composed of highly pleomorphic cell arranged in glandular pattern and diffuse sheets with mucin pools infiltrating the deep muscle upto perivesicular fat and into the adjacent soft tissue and prostate (Figure 3). Hence, histopathological diagnosis of metastatic mucin secreting adenocarcinoma infiltrating to bladder and prostate was considered. Unfortunately the patient died in the postoperative period due to sepsis.

Figure 3: (a) Gross- bladder wall was diffusely thickened, (b) and (c) Metastatic mucin secreting adenocarcinoma of urinary bladder (H&E, 10X and 40X), (d) Mucicarmine stain – Mucin pools with tumor cells, (e) TURP – adenocarcinoma (H&E, 10X), (f) FNAC from perianal nodule showing mucin and atypical cells (MGG, 40X).
Discussion
Bladder carcinoma constitutes a spectrum of epithelial tumors and urothelial carcinoma is the most common type, but also includes squamous cell carcinoma, adenocarcinoma, small cell tumors and other histological variants. Urothelial carcinoma has a divergent spectrum of microscopic forms including squamous cell differentiation. Generally urothelial carcinoma has better response to chemotherapy and have good prognosis. When compared to conventional urothelial carcinoma, squamous cell carcinoma has been associated with adverse oncologic outcomes and worse disease specific survival [8]. Most of the squamous cell carcinoma are high grade with muscle invasion at the time of diagnosis. Our case showed moderately differentiated squamous cell carcinoma with invasion. Since this tumor may be resistant to chemotherapy and radiotherapy, surgical resection will be treatment of choice [9].
Squamous differentiation is the most common variant of urothelial carcinoma. Liu et al stated urothelial carcinoma with squamous differentiation is associated with a high tumor stage and a high rate of pelvic nodal metastasis [4]. These factors accounts for the aggressive clinical behavior of this variant which was even observed in our case where the tumor was of high stage with nodal metastasis at time of presentation.
Though the bladder is not a common site for metastasis, secondary adenocarcinoma is more common than primary adenocarcinoma. When a diagnosis of adenocarcinoma bladder was made, usually the queries raises whether it is primary, urachal or metastatic arising from adjacent organ or distant site. The incidence of bladder involvement in colonic and rectal carcinomas was only 0.06% [7]. Our case was rectal carcinoma metastasis to urinary bladder and prostate which is extremely rare and the exact mechanism for distant metastasis is still unclear. For any tumor to produce metastasis, malignant cells should exhibit intravasation, embolization, survival in circulation, arrest of cells in capillary bed, extravasation and multiplication in organ parenchyma [10]. Although this condition is uncommonly encountered in clinical practice, the possibility of metastatic involvement of the bladder should be ruled out before primary adenocarcinoma has to be diagnosed. The prognosis of such cases is poor as seen in our case.
Conclusion
The spectrums of microscopic forms of bladder carcinoma have been expanded recently to include several histological variants. Hence recognition of these rare histological variants of bladder carcinoma may be helpful in selecting appropriate therapeutic approach and to predict the prognosis of the patients.
Acknowledgements
The Department of Urology, Sri Venkateswaraa Medical College Hospital and Research Centre, Puducherry.
Conflicts of interest
Authors declare no conflicts of interest.
References
[1] Yuvaraja TB, Waigankar S, Bakshi G, Prakash G. Genitourinary cancers: Summary of Indian data. South Asian J Cancer. 2016; 5:122–124.
[2] Gupta P, Jain M, Kapoor R, Muruganandham K, Srivastava A, et al. Impact of age and gender on the clinicopathological characteristics of bladder cancer. Indian J Urol. 2009; 25:207–210.
[3] Wishahi M, Elganzoury H, Badawy M. Squamous cell carcinoma and squamous differentiation histologic variant of urothelial carcinoma of urinary bladder: oncological outcome following definitive surgical treatment. Int J Cancer Clin Res. 2014; 1:1.
[4] Liu Y, Bui M, Xu B. Urothelial carcinoma with squamous differentiation is associated with high tumor stage and pelvic lymph-node metastasis. Cancer Control. 2017; 24:78–82.
[5] Chalasani V, Chin J, Izawa J. Histologic variants of urothelial bladder cancer and nonurothelial histology in bladder cancer . CUAJ. 2009; 3:S193–S198.
[6] Thomas DG, Ward AM, Williams JL. A study of 52 cases of adenocarcinoma of the bladder. Br J Urol. 1971; 43:4–15.
[7] Chang CL, Chen YT. Metastatic colon cancer to the urinary bladder: a case report. J Soc Colon Rectal Surgeon. 2009; 20:39–42.
[8] Jagtap SV, Sarda DS, Demde RB, Huddedar AD, Jagtap SS. Primary squamous cell carcinoma of urinary bladder – rare histological variant. J Clin Diag Res. 2015; 9:ED03–ED04.
[9] Rogers CG, Palapattu GS, Shariat SF, Karakiewicz PI, Bastian PJ, et al. Clinical outcome following radical cystectomy for primary non transitional cell carcinoma of the bladder compared to transitional cell carcinoma of the bladder. J Urol. 2006; 175:2048–2053.
[10] Gutman M, Fidler IJ. Biology of human colon cancer metastases. World J Surg. 1995; 19:226–234.