Abstract
Purpose: To compare the results of a single surgeon, arthroscopically assisted Anterior cruciate ligament (ACL) reconstruction with the Bone-patellar tendon-bone (BPTB) and the hamstring tendons grafts using aperture screw fixation.
Study design: Prospective cohort study.
Materials and methods: Two groups of patients, 30 each in BPTB group and hamstring group, were followed for at least 2 years. Patients with width of patellar tendon > 28mm had BPTB graft and all others received hamstring tendon graft.
Results: Cohorts were comparable with regard to demographic data. At two year follow-up there was no significant difference in knee scores (Modified Cincinnati, BPTB 96.07 ± 4.58 vs Hamstring 93.96 ± 5.54, p=0.123; Tegner Lysholm, BPTB 93.30 ± 5.70 vs Hamstring 91.40 ± 5.71, p=0.203). On clinical examination, laxity was found in more number of hamstring patients. None of the patients had recurrent symptoms and none required revision for any other reasons. Anterior knee pain was present in 5 patients in each group. Kneeling pain was significantly higher in BPTB group (7 vs 3). 28 patients in BPTB group and 27 in hamstring group were able to achieve pre-injury activity level.
Conclusion: Both graft options give excellent short term results. Proper selection of the patients based on their activity level and requirement of kneeling can improve functional results. BPTB may be preferred in high demand individuals. Use of two incision technique of graft harvest lead to fewer donor site complications in BPTB.
Keywords: ACL reconstruction; bone patellar tendon graft; hamstring tendon graft; aperture interference screw fixation
Full Text
Introduction
Anterior cruciate ligament (ACL) tear is the most common serious ligamentous injury to the knee joint [1]. Arthroscopic reconstruction of ACL is the worldwide accepted method of treatment with consistently good results. Bone-patellar tendon-bone (BPTB) and the hamstring tendon are the two most commonly used autografts for reconstruction [2-7]. Despite a tremendous amount of research on this topic, choice of graft still remains largely a matter of surgeon’s preference. BPTB autograft has been widely accepted as the gold standard for ACL reconstruction with a high success rate [2]. However hamstring tendon graft has become increasingly popular in last decade [8, 9].
BPTB grafts have the advantage of faster and stronger bone to bone healing, giving a more secure fixation [10-12]. The stiffness of BPTB graft is greater than original ACL [13], which transforms clinically into more static stability [14-16]. However anterior knee pain, especially on kneeling, is a very common complication which has been reported in literature [16, 17]. Dissatisfaction and potential inability to return to work have been reported in patients that perform kneeling as part of their occupation or religion. BPTB grafts had a clinically insignificant loss of extension and demonstrated a trend towards reduced extension strength according to a Cochrane review [17]. However, most of the studies conclude that return to pre-injury state is more in BPTB grafts, especially in high demand or athletic individuals [9].
Hamstring grafts avoid the disadvantages of donor site morbidity in the form of kneeling pain as seen with BPTB graft. They also have the advantage of better cosmesis, as incision required to harvest the graft is in the same location as starting point of the tibial tunnel. However, hamstring grafts are not without their disadvantages. Hamstring tendon grafts may increase in laxity over time. In a systemic review, Reinhardt et al. found hamstring grafts demonstrate increased laxity as compared to BPTB [18]. Another disadvantage of hamstrings tendon grafts is delayed soft-tissue to bone healing which is less reliable [11, 19, 20]. Many studies evaluating the morbidity of hamstring tendon harvest have demonstrated reduced knee flexion strength compared with the contralateral extremity, but similar to the loss of extension strength seen in some studies after BPTB autografts. It is unknown if this difference is clinically significant [17]. According to cohort study from Norwegian ligament registry, which included 14,034 patients and another retrospective analysis by Maletis et al., which included 9817 patients, hamstring grafts carry a slightly higher rate of revision [21, 22].
Both the graft options have their advantages as well as certain drawbacks. So, the choice of best graft for ACL reconstruction is debatable. Most of the published literature has various confounding variables like different surgeons using different grafts, different modes of fixation and postoperative rehabilitation protocols.
The aim of this study was to compare the results of arthroscopic ACL reconstruction using the BPTB and the hamstring tendon graft using aperture screw fixation with similar identical post operative protocols by a single surgeon.
Material and methods
This study comprises of 60 patients (30 in each group) with chronic unilateral rupture of the anterior cruciate ligament treated by arthroscopic reconstruction with use of either autologous bone-patellar tendon-bone or tripled hamstring tendon graft from December 2011 to March 2013 done by a single surgeon (SG).
Only patients with symptomatic instability with isolated ACL tear or ACL injury with meniscal tear, confirmed by clinical examination (positive pivot shift test) and radiologically by MRI were operated. Patients in the age group 15-45 years which could be followed up to minimum of two years were included in the study.
Patients with PCL injury, ACL injury to the contra lateral knee, medial or lateral collateral ligament injuries and re-injury to a previously reconstructed ACL were excluded from the study.
Graft selection criteria
Measurement of width of patellar tendon was done midway between inferior pole of patella and tibial tubercle. In patients with tendon width >28 mm, BPTB graft was taken. As the senior author (SG) considered 9mm width of BPTB graft to be critical to have sufficient strength, patients with tendon width <28 mm were given ipsilateral hamstring graft.
Surgical technique
Patients were operated under spinal anaesthesia under pneumatic tourniquet control. Preoperative antibiotic (Inj. Cefuroxime 1.5 gm i.v.) was given on induction. Standard anteromedial and anterolateral portals were made. Diagnostic arthroscopy was done and meniscus were examined. In case of meniscal injury, either repair or partial menisectomy was done depending on the site and type of tear.
Harvesting of graft
In hamstring group, semitendinosus tendon was harvested through a small longitudinal anteromedial incision over the pes anserinus insertion using an open stripper and then detached at the insertion. If graft diameter was found to be less than 7mm after tripling, gracilis was also harvested. Harvested graft was tripled using 2 ethibond with whiplash type sutures.
The BPTB autograft was harvested via two incision technique. One incision was given over the lower pole of patella (usually 2 cms in length), another was given over the medial part of tibial tuberosity (usually 2-3 cms in length). The second incision was given in such a way that it could also be used for preparing tibial tunnel. Central one-third of patellar tendon was harvested in sub tenosynovial fashion with 20-25 mm of bone blocks on either side with leading suture on the patellar side. The bone blocks were trimmed to cylindrical shape. The nibbled bone was filled in the defects at harvesting site and tendon sheath was closed.
Stumps of the torn ACL were left intact in cases of hamstring graft, whereas stumps were trimmed for BPTB graft. Notchplasty was not done. Foot prints of damaged stump were preserved. Tibial tunnel was prepared. Femoral tunnel was prepared by trans anteromedial portal technique. Graft was passed through the ACL remnant in a biological fashion. The graft was first fixed into the femoral tunnel using interference screws. After cyclical tensioning of graft, tibial end was fixed with interference screws with knee in 30 degrees of flexion.
Postoperative protocol
Knee range of motion exercises, quadriceps and hamstring strengthening and full weight bearing mobilisation were initiated from day 1, CPM was not used. Extension knee brace while walking was used for 6 weeks in cases with hamstring graft. No brace or support was used in BPTB group. Running, squatting was initiated at 3-4 months, light sports at 5-6 months and strenuous sports at 9-12 months, though there could have been a little variation in patient compliance. Postoperative protocol differed for patients in whom meniscal repair was done. They were kept in knee brace in extension for 6 weeks, following which flexion was allowed upto 90 degree till 3 months. After 3 months complete range of motion was allowed and activity level gradually increased.
Clinical evaluation
All patients were followed-up by the same surgeon as well as an independent observer. Clinical evaluation and scoring was performed by the independent observer at 6 months, 1 year and 2 years. The clinical outcome scores used were Tegner Lysholm score and Modified Cincinatti score.
The evaluation included supine range of motion measurements with goniometer, stability testing included the Lachman test, anterior drawer test and pivot shift test. Lachman’s test was compared with the normal knee and was classified as lax or not. The pivot shift test was graded as glide or clunk.
Results
Demographic data
60 patients were included in the study. There were 30 patients in the BPTB group and 30 patients in the hamstring group. Duration of follow-up evaluation was not different. Both groups had no significant difference in age and sex distribution. There was also no significant difference in the time duration between injury and operation, type and number of associated injuries and concomitant surgeries (Table 1).
Table 1: Patient demography and preoperative details.
| |
BPTB
|
HT
|
|
Age (in years)
|
29.5 (min=19, max=45)
|
29.4 (min=17, max=43)
|
|
M:F
|
30:0
|
29:1
|
|
BMI
|
24.1 (min=20, max=26)
|
25.2 (min=20, max=26.5)
|
|
Mild-moderate activity pre injury
|
13
|
18
|
|
Strenuous activity pre injury
|
17
|
12
|
|
Associated lateral meniscus injury
|
8
|
8
|
|
Associated medial meniscus injury
|
9
|
7
|
|
Meniscus repaired
|
3
|
2
|
|
Partial meniscectomy
|
14
|
13
|
|
Average time duration between injury and surgery (in days)
|
62
|
69
|
Stability testing
Manual Lachman and Pivot shift tests were used for stability testing. Tests were compared and concluded with respect to the unaffected knee. Slight excursion of operated knee on doing Lachman’s test when compared to the unaffected knee, was termed as positive. At follow-up of two years, number of patients which tested positive for laxity by Lachman’s test were higher in hamstring group (14, as compared to 8 in BPTB). Also, 4 patients in hamstring group had pivot shift glide as compared to 1 in BPTB group, but the difference was not found to be significant (Table 2). This difference could have been significant if a similar trend was present with more number of patients in each group. A larger study with adequate power can provide a more definite answer.
Table 2: Results of stability testing at two year follow-up.
|
At two years
|
BPTB (N=30)
|
Hamstring (N=30)
|
|
Lachman’s
Laxity +
Soft end point
|
8
0
|
14
0
|
|
Pivot shift
Glide
Clunk
|
1
0
|
4
0
|
Patient satisfaction
Patient satisfaction was found to be similar in both the groups. 28 patients in BPTB group and 27 patients in hamstring group could achieve pre-injury activity level and were happy with the surgery.
Clinical scores
Clinical scores (both Modified Cincinnati score and Tegner Lysholm score) were comparable in both the groups preoperatively (Modified Cincinatti, BPTB= 62.50 ± 7.77, Hamstring= 63.63 ± 8.34, P value= 0.588; Tegner Lysholm score, BPTB= 52.73 ± 9.50, Hamstring= 54.00 ± 10.30, P value= 0.623). After 1 year of surgery, scores were found to be significantly better in BPTB group (Modified Cincinnati, 96.90 ± 3.65 vs 94.57 ± 4.71, p=0.036; Tegner Lysholm, 93.83 ± 5.71 vs 91.67 ± 5.68, p=0.049), but it was not clinically relevant as both the groups fell in excellent category. But this difference in scores between these two groups was not significant at 2 years follow-up (Modified Cincinnati, 96.07 ± 4.58 vs 93.96 ± 5.54, p=0.123; Tegner Lysholm, 93.30 ± 5.70 vs 91.40 ± 5.71, p=0.203) (Table 3).
Table 3: Comparison of clinical scores at follow-up of 1 year and 2 years.
| |
|
BPTB
N=30
|
Hamstring
N=30
|
P value
|
|
Preoperative
|
Modified Cincinatti score
|
62.50 ± 7.77
|
63.63 ± 8.34
|
0.588
|
|
Tegner Lysholm score
|
52.73 ± 9.50
|
54.00 ± 10.30
|
0.623
|
|
1 Year
|
Modified Cincinatti score
|
96.90 ± 3.65
|
94.57 ± 4.71
|
0.036
|
|
Tegner Lysholm score
|
93.83 ± 5.71
|
91.67 ± 5.68
|
0.049
|
|
2 Year
|
Modified Cincinatti score
|
96.07 ± 4.58
|
93.96 ± 5.54
|
0.123
|
|
Tegner Lysholm score
|
93.30 ± 5.70
|
91.40 ± 5.71
|
0.203
|
To exclude the effect of meniscal injuries, both the groups were categorised into two sub-groups. Sub-group A comprised of isolated ACL injuries and sub-group B comprised of ACL + meniscal injuries. Comparison of sub-group A of BTB group (n=13) with sub-group A of Hamstring group (n=15) revealed significantly better Tegner Lysholm score in BPTB (98.88 ± 1.96 vs 95.67 ± 3.55, p=0.01) at the end of 1 year, but no difference by 2 year follow-up (Table 4).
Table 4: Comparison of isolated ACL injuries treated with BPTB versus Hamstring graft.
| |
|
Isolated ACL BPTB, N=13
|
Isolated ACL Hamstring, N=15
|
P value
|
|
Preoperative
|
Modified Cincinatti score
|
51.92 ± 11.01
|
54.13 ± 12.13
|
0.620
|
|
Tegner Lysholm score
|
60.00 ± 8.93
|
64.00 ± 10.90
|
0.303
|
|
1 Year
|
Modified Cincinatti score
|
96.08 ± 4.09
|
92.87 ± 4.92
|
0.075
|
|
Tegner Lysholm score
|
98.88 ± 1.96
|
95.67 ± 3.55
|
0.010
|
|
2 Year
|
Modified Cincinatti score
|
95.92 ± 3.79
|
92.73 ± 5.10
|
0.076
|
|
Tegner Lysholm score
|
97.92 ± 2.46
|
95.42 ± 4.90
|
0.116
|
To reveal the effect of concomitant meniscal injuries in clinical outcome of ACL reconstruction surgeries, we also compared clinical scores of patients with isolated ACL injuries (i.e., sub-group A of both BPTB and Hamstring groups) with that of patients with associated meniscal injuries (i.e., sub-group B of both BPTB and Hamstring groups). Patient with only ACL injuries had significantly better scores at end of 1 year and 2 years (Table 5).
Table 5: Comparison of isolated ACL injuries versus ACL with concomitant meniscal injuries at follow-up of 1 year and 2 years.
| |
|
Isolated ACL
N=28
|
ACL + meniscus
N=32
|
P value
|
|
Preoperative
|
Modified Cincinatti score
|
53.11 ± 11.47
|
53.59 ± 8.36
|
0.851
|
|
Tegner Lysholm score
|
62.14 ± 10.06
|
63.88 ± 5.71
|
0.408
|
|
1 Year
|
Modified Cincinatti score
|
94.36 ± 4.76
|
91.34 ± 6.24
|
0.042
|
|
Tegner Lysholm score
|
97.11 ± 3.28
|
94.53 ± 4.82
|
0.021
|
|
2 Year
|
Modified Cincinatti score
|
94.21 ± 4.74
|
90.72 ± 6.10
|
0.017
|
|
Tegner Lysholm score
|
96.72 ± 3.96
|
93.78 ± 5.60
|
0.030
|
Complications
None of the patient in any group had recurrent instability or giving away. Even though, on stability testing, a number of knees were found to be slightly lax (14 in hamstring group and 8 in BPTB group), this did not transform into symptomatic instability. Five patients in each of the group had complaints of anterior knee pain which was intermittent, dull and aggravated by strenuous activities. Incidence of kneeling pain was significantly higher in BPTB group, seven patients as compared to three in hamstring group. These patients had to modify their activities to avoid pain. None of the patients had any extension deficit or loss of range of motion as compared to the unaffected side. Three patients had superficial infection postoperatively, one in BPTB group and two in Hamstring group. This was managed by oral antibiotics and local debridement and dressing. None of the patients required revision of surgery (Table 6).
Table 6: Complications.
| |
BPTB (n=30)
|
Hamstring (n=30)
|
|
Anterior knee pain
|
5
|
5
|
|
Kneeling pain
|
7
|
3
|
|
Giving away
|
0
|
0
|
|
Extension deficit
(>10 degrees)
|
0
|
0
|
|
Patellar fracture
|
0
|
0
|
|
Superficial infection
|
1
|
2
|
Discussion
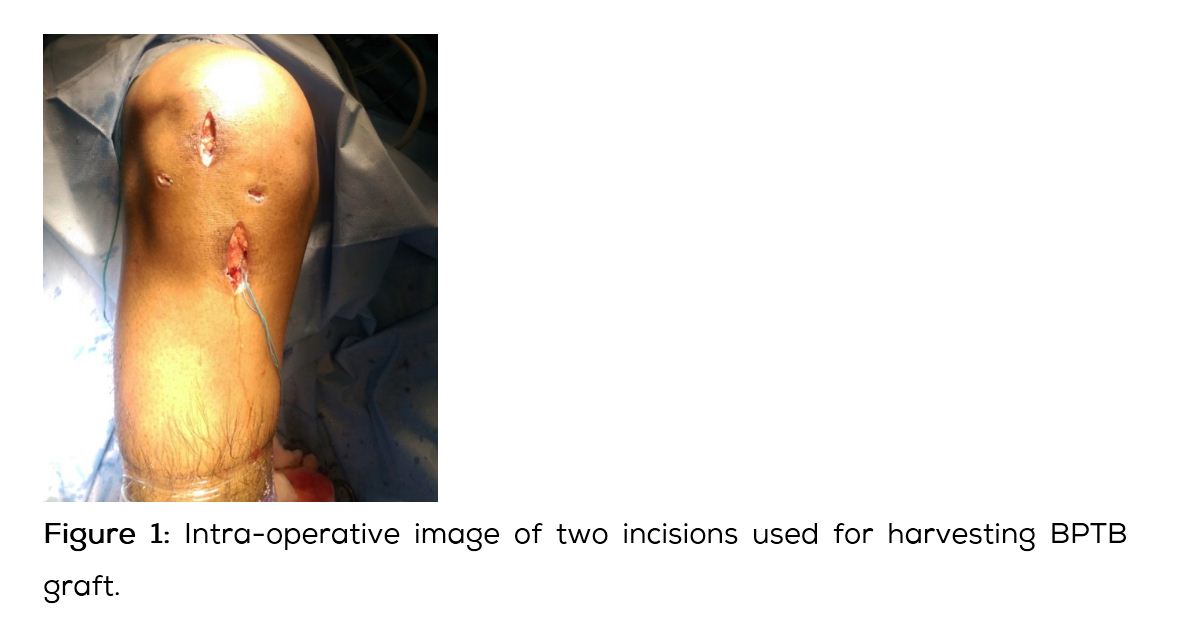
Results of the present study clearly show that both BPTB and hamstring tendon grafts effectively improve knee stability and functions after ACL reconstruction (Figure 1). At last follow-up evaluation, both groups had similar outcomes as assessed by Modified Cincinnati and Tegner Lysholm knee score. There have been many prospective randomized control studies comparing the two groups published in recent years. In a similar study, Corry et al. found that the two grafts did not differ in terms of clinical stability, range of motion and general symptoms [23]. Results from various other studies also show that the two groups had similar outcomes at the 2-5 year period [4-6, 24, 25]. Our study adds more supporting evidence to this literature.
A very important criteria for judgement of success of surgery is “return to pre-injury level”. In BPTB group there were more number of patients involved in strenuous physical activity including professional sports when compared to hamstring group. Nonetheless, recovery in both the cohorts was good, signifying good results.
Donor site morbidity is a major drawback of the BPTB graft. Significant number of patients in our study experienced kneeling pain, though incidence of anterior knee pain was equal in both the groups. In studies published by other authors [4-6, 8, 17] incidence of kneeling pain and anterior knee pain has been even higher in the BPTB group, which can be attributed to the painful neuroma formed by the infrapatellar branch of saphenous nerve which gets damaged during harvesting of the graft. Due to similar reason, a few authors have also reported disturbance of anterior knee sensation in these patients [23, 26]. In our patients we have tried to minimize this by harvesting the graft sub teno-synovially by a two incision technique, thus avoiding transection of the nerve. In most of the BPTB patients experiencing kneeling pain and anterior knee pain, it was localised to tibial tubercle. So, probably it was due to impingement of the tendon against the edge of the bone defect produced due to harvesting of graft. We did put bone graft from the nibbled bone blocks of BPTB graft into the defect, but that probably is insufficient. Using the cancellous bone graft harvested from the core harvester while reaming the femur and tibia tunnels may help in further decreasing the kneeling pain [27].
In the hamstring group, anterior knee pain may be a reflection of slight laxity in the joint which could lead to overload of patella-femoral articulation. The laxity may be due to less stiffness of the hamstring as compared to native ACL or BPTB. With similar prospective randomized comparisons, Beynnon et al. found that after three years of follow-up, the objective results of anterior cruciate ligament reconstruction with a BPTB were superior to those of reconstruction with a two-strand semitendinosus-gracillis tendon graft with regard to knee laxity, pivot shift grade, and strengths of the knee flexor muscle [7]. However, the two groups had comparable results in terms of patient satisfaction, activity level, and knee functions. In 2001, Yunes et al. were the first to report a meta-analysis conducted from controlled trials of patellar tendon versus hamstring tendons for ACL reconstruction [14]. They found that the patellar tendon patients had a greater chance of attaining a statically stable knee and nearly a 20% greater chance of returning to preinjury activity levels. They concluded that although both techniques yielded good results, patellar tendon reconstruction led to higher postoperative activity levels and greater static stability than hamstring reconstruction. In 2003, using the same and extended numbers of controlled trial, Freedman et al. found that the rate of graft failure in the patellar tendon group was significantly lower and a significant higher proportion of patients in the patellar tendon group had a side-to-side difference of less than 3 mm on KT-1000 arthrometer testing than in the hamstring tendon group [15].
In this study, choice of graft was dictated by the anatomy of the patient’s patellar tendon. In patients where the width of patellar tendon midway between tibial tubercle and lower pole of patella was less than 28 mm, BPTB was not harvested. The surgeon considered nine mm to be critical width of the flat patellar tendon to allow adequate cross-sectional area for sufficient strength. In these patients, hamstring graft was harvested and attaining sufficient diameter of the graft was not found to be difficult. In this regard, hamstring tendons have an advantage over BPTB that their diameter can be varied and not getting thick enough graft even after harvesting both semitendinosus and gracilis is a rare occurrence. Considering that Indian patients’ stature is smaller as compared to western population, it may not be always possible to get a sufficiently thick BPTB graft.
The evidence in literature is conflicting regarding choice of graft for ACL reconstruction. Minimization of variables is an important aspect in our study. All the cases were operated by a single surgeon who is well versed with both the techniques. Same fixation method (aperture fixation with interference screws) was used in both the groups, thus, eliminating effect of fixation technique on the results. Basic surgical technique and steps were same. Similar physiotherapy protocol was followed for both the groups. Hence we were able to have a true comparison between the graft options. All the cases were followed up and scored by an independent observer, thus reducing bias. Also, subgroup analysis was done to exclude the effect of meniscal injuries on outcome.
There are also a few limitations of the study. Study sample size is small. Exact quantification of laxity in the knee joint could not be measured postoperatively due to unavailability of arthrometer. The duration of follow-up is only two years.
Conclusion
Both the BPTB and the hamstring tendon grafts result in significantly improved knee stability and functions, with high patient satisfaction. Authors/surgeon cannot recommend a any graft universally as there are advantages and drawbacks for both the grafts. But proper selection of the patients based on their activity level and requirement of kneeling can improve functional results. BPTB can be given preference in view of better stability, especially in high demand individuals. Modification of graft harvesting techniques can lead to fewer donor site complications in BPTB. In low demand individuals, people who require frequent kneeling for religious or occupational purposes, hamstring graft may be preferred.
Conflicts of interest
Authors declare no conflicts of interest.
References
[1] Miyasaka KC, Daniel DM, Stone ML. The incidence of knee ligament injuries in the general population. Am J Knee Surg. 1991; 4:3-8.
[2] Shaieb MD, Kan DM, Chang SK, Marumoto JM, Richardson AB. A prospective randomized comparison of patellar versus semitendinosus and gracillis tendon autografts for anterior cruciate ligament reconstruction. Am J Sports Med. 2002; 30(2):214-220.
[3] Barrett GR, Noojin FK, Hartzog CW, Nash SR. Reconstruction of the anterior cruciate ligament in females: A comparison of hamstring versus patellar tendon autograft. Arthroscopy. 2002; 18(1): 46-54.
[4] Ejerhed L, Kartus J, Sernert N, Kohler K, Karlsson J. Patellar tendon or semitendinosus tendon autografts for anterior cruciate ligament reconstruction: A prospective randomized study with a two-year follow-up. Am J Sports Med. 2003; 31(1):19-25.
[5] Jansson KA, Linko E, Sandelin J, Harilainen A. A prosective randomized study of patellar versus hamstring tendon autografts for anterior cruciate ligament reconstruction. Am J Sports Med. 2003; 31(1):12-18.
[6] Pinczewski LA, Deehan DJ, Salmon LJ, Russell VJ, Clingeleffer A. A five-year comparison of patellar tendon versus four-strand hamstring tendon autograft for arthroscopic reconstruction of the anterior cruciate ligament. Am J Sports Med. 2002; 30(4):523-536.
[7] Beynnon BD, Johnson RJ, Fleming BC, Kannus P, Kaplan M, et al. Anterior cruciate ligament replacement: comparison of bone-patellar tendon-bone grafts with two strand hamstring grafts. J Bone Joint Surg Am. 2002; 84-A(9):1503-1513.
[8] Poolman RW, Farrokhyar F, Bhandari M. Hamstring tendon autograft better than bone patellar-tendon bone autograft in ACL reconstruction: A cumulative meta-analysis and clinically relevant sensitivity analysis applied to a previously published analysis. Acta Orthop. 2007; 78(3):350-354.
[9] Mascarenhas R, Tranovich MJ, Kropf EJ, Fu FH, Harner CD. Bone-patellar tendon-bone autograft versus hamstring autograft anterior cruciate ligament reconstruction in the young athlete: a retrospective matched analysis with 2–10 year follow-up. Knee Surg Sports Traumatol Arthrosc. 2012; 20(8):1520-1527.
[10] Gulotta LV, Rodeo SA. Biology of autograft and allograft healing in anterior cruciate ligament reconstruction. Clin Sports Med. 2007; 26(4):509-524.
[11] Papageorgiou CD, Ma CB, Abramowitch SD, Clineff TD, Woo SL. A multidisciplinary study of the healing of an intraarticular anterior cruciate ligament graft in a goat model. Am J Sports Med. 2001; 29(5):620-626.
[12] Park MJ, Lee MC, Seong SC. A comparative study of the healing of tendon autograft and tendon-bone autograft using patellar tendon in rabbits. Int Orthop. 2001; 25(1):35-39
[13] Cooper DE, Deng XH, Burstein AL, Warren RF. The strength of the central third patellar tendon graft. A biomechanical study. Am J Sports Med. 1993; 21(6):818-824.
[14] Yunes M, Richmond JC, Engels EA, Pinczewski LA. Patellar versus hamstring tendons in anterior cruciate ligament reconstruction: A meta-analysis. Arthroscopy. 2001; 17(3):248-257.
[15] Freedman KB, D’Amato MJ, Nedeff DD, Kaz A, Bach BR. Arthroscopic anterior cruciate ligament reconstruction: A metaanalysis comparing patellar tendon and hamstring tendon autografts. Am J Sports Med. 2003; 31(1):2-11.
[16] Mohtadi NG, Chan DS, Dainty KN, Whelan DB. Patellar tendon versus hamstring tendon autograft for anterior cruciate ligament rupture in adults. Cochrane Database Syst Rev. 2011; 9:CD005960.
[17] Kraeutler MJ, Bravman JT, McCarty EC. Bone–patellar tendon–bone autograft versus allograft in outcomes of anterior cruciate ligament reconstruction: A meta-analysis of 5182 patients. Am J Sports Med. 2013; 41(10):2439-2448.
[18] Reinhardt KR, Hetsroni I, Marx RG. Graft selection for anterior cruciate ligament reconstruction: A level I systematic review comparing failure rates and functional outcomes. Orthop Clin North Am. 2010; 41(2):249-262.
[19] Goradia VK, Rochat MC, Grana WA, Rohrer MD, Prasad HS. Tendon-to-bone healing of a semitendinosus tendon autograft used for ACL reconstruction in a sheep model. Am J Knee Surg. 2000; 13(3):143-151.
[20] Tomita F, Yasuda K, Mikami S, Sakai T, Yamazaki S, et al. Comparisons of intraosseous graft healing between the doubled flexor tendon graft and the bone-patellar tendon bone graft in anterior cruciate ligament reconstruction. Arthroscopy. 2001; 17(5):461-476.
[21] Persson A, Kjellsen AB, Fjeldsgaard K, Engebretsen L, Espehaug B, et al. Registry data highlight increased revision rates for endobutton/biosure HA in ACL reconstruction with hamstring tendon autograft: a nationwide cohort study from the Norwegian Knee Ligament Registry, 2004-2013. Am J Sports Med. 2015; 43(9):2182-2188.
[22] Maletis GB, Inacio MC, Desmond JL, Funahashi TT. Reconstruction of the anterior cruciate ligament: association of graft choice with increased risk of early revision. Bone Joint J. 2013; 95-B:623–628.
[23] Corry IS, Webb JM, Clingeleffer AJ, Pinczewski LA. Arthroscopic reconstruction of the anterior cruciate ligament. Am J Sports Med. 1999; 27(4):444-454.
[24] Anderson AF, Snyder RB, Lipscomb AB. Anterior cruciate ligament reconstruction: A prospective randomized study of three surgical methods. Am J Sports Med. 2001; 29(3):272-279.
[25] Eriksson K, Anderberg P, Hamberg P, Lofgren AC, Bredenberg M, et al. A comparison of quadruple semitendinosus and patellar tendon grafts in reconstruction of the anterior cruciate ligament. J Bone Joint Surg Br. 2000; 83(3):348-354.
[26] Aglietti P, Giron F, Buzzi R, Biddau F, Sasso F. Anterior cruciate ligament reconstruction : bone-patellar tendon-bone compared with double semitendinosus and gracilis tendon grafts. A prospective, randomized clinical trial. J Bone Joint Surg Am. 2004; 86-A(10):2143-2155.
[27] Tsuda E, Okamura Y, Ishibashi Y, Otsuka H, Toh S. Techniques for reducing anterior knee symptoms after anterior cruciate ligament reconstruction using a bone-patellar tendon-bone autograft. Am J Sports Med. 2001; 29(4):450-456.
[28] Noyes FR, Matthews DS, Mooar PA, Grood ES. The symptomatic anterior cruciate-deficient knee. Part II: the results of rehabilitation, activity modification, and counseling on functional disability. J Bone Joint Surg Am. 1983; 65(2):163-174.