Full Text
Neuropathic arthropathy is a chronic, progressive degenerative joint disease secondary to abnormal sensory innervation of such articulation [1]. Neuropathic arthropathy of elbow is rare and constitutes 3-8% of all the cases of neuropathic joints [2]. Syringomyelia is the most common cause of neuropathic elbow and the diagnosis is often missed [1, 3]. Very few cases of neuropathic elbow with septic arthritis are reported in the literature [2, 4-6]. There is a paucity of literature guiding the effective management of complicated and delayed presentations of neuropathic arthropathy of elbow [3, 4, 7]. This article highlights an effectively managed case of neuropathic elbow with complex presentation.
Case presentation
A forty seven year old right handed man presented with a swelling over his left elbow since nine months, pain, fever and discharge of pus from the wound over his left elbow since two weeks. The swelling was insidious in onset, slowly progressing in size and there was no history of trauma. Patient complained of high grade fever with elbow pain followed by ulceration and discharge of pus (Figure 1).
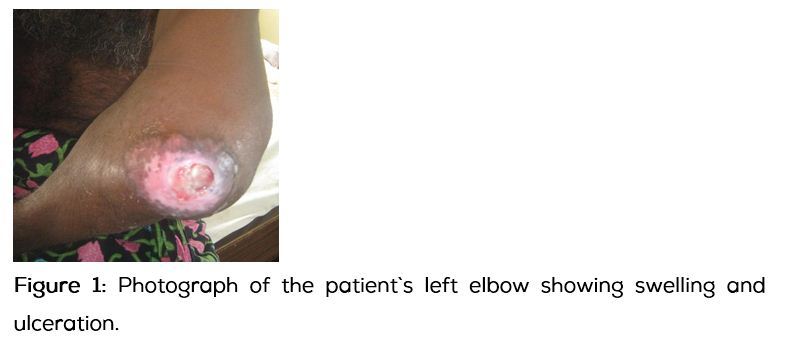
In the past, he had multiple consultations elsewhere for his elbow swelling where magnetic resonance imaging (MRI) of elbow and open biopsy were done. Differential diagnosis of tenosynovial giant cell tumor/ synovial chondrosarcoma/ aggressive infectious synovitis with arthritis/ neuropathic joint were put forth for consideration from the MRI findings of his left elbow. Biopsy was suggestive of giant cell tumor of tendon sheath. He was advised above elbow amputation with a diagnosis of infected, ulcerated, giant cell tumour of tendon sheath. He refused amputation and presented to us with a request for limb salvage.
On examination, patient had diffuse elbow swelling with an ulcer over the posterolateral aspect associated with local raise of temperature and tenderness. The skin around the swelling was stretched and shiny with engorged veins. Attempted movements at the elbow were painful. Neurological examination revealed wasting of intrinsic muscles of the hand with loss of grip strength, diminished touch and pain sensations in the arm, forearm, hand and upper half of trunk on left side. Distal arterial pulses were normal. A boggy painless swelling was noted over the base of the left thumb.
His total leucocyte count was 10,500/cumm with 79% neutrophills, C-reactive protein was elevated and ESR was 142mm/h. Radiograph of left elbow showed resorption of the articulating surfaces with elbow dislocation and flecks of calcification in the diffuse soft tissue mass around the elbow (Figure 2). Radiograph of left hand revealed destruction of trapezo-metacarpal joint with surrounding soft tissue mass. With a high index of suspicion to rule out neuropathic arthropathy of elbow, MRI of cervical spine was done. The MRI of cervical spine revealed low lying cerebellar tonsils extending up to first cervical vertebra with enlargement of central canal of the cervical spine predominantly to left side suggestive of Chiari type I malformation with syringomyelia (Figure 3). Culture of pus from the ulcerated swelling has shown growth of methicillin sensitive staphylococcus aureus (MSSA) sensitive to clindamycin, ceftriaxone and amikacin. Intravenous antibiotic therapy with clindamycin was started.
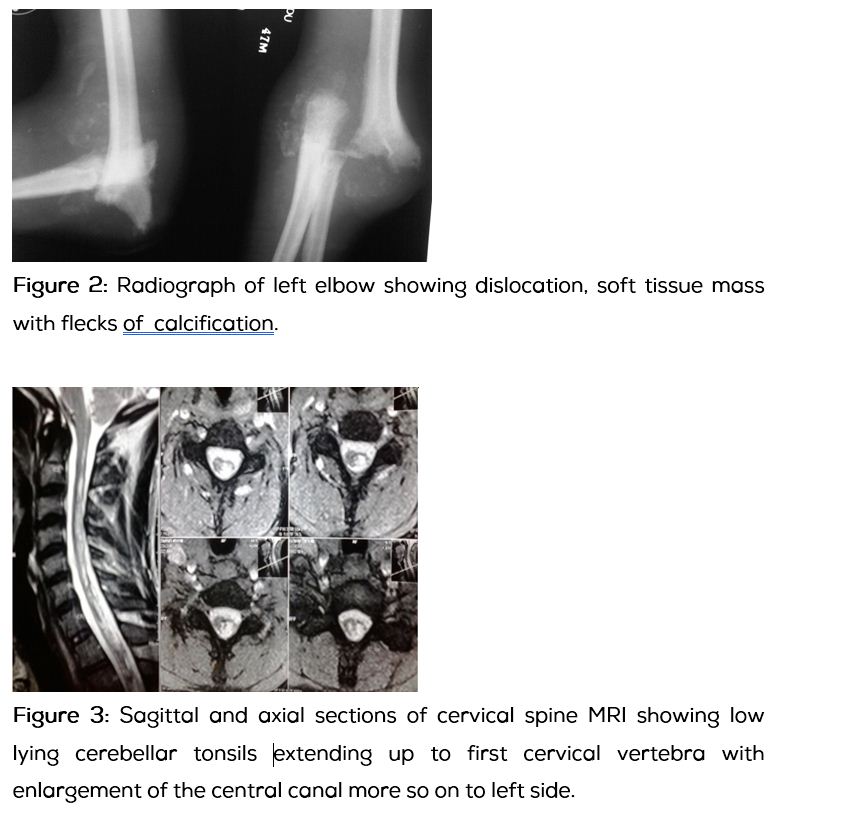
Critical review and second opinion of the biopsy report and histopathology slides confirmed neuropathic arthropathy. Thus a diagnosis of neuropathic arthropathy of elbow secondary to Chiari malformation and syringomyelia with septic arthritis was made. Neurosurgeon consultation was sought to address the posterior fossa malformation and syringomyelia for which he advised observation and follow up.
Under the antibiotic cover, surgical management with open debridement and elbow arthrodesis with spanning external fixator and lag screw was done (Figure 4). Oral antibiotic therapy was continued for eight weeks. External fixator was removed after ten weeks when all the inflammatory signs have disappeared and stability of the elbow joint was confirmed. Patient was advised to use an elbow brace following the removal of the external fixator, which he did not abide by. He started using his operated elbow for his routine agricultural works.
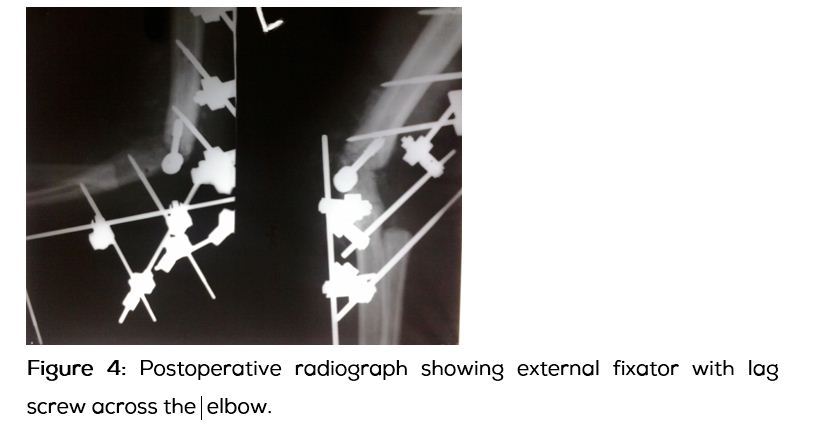
Four weeks later patient came back with recurrence of the swelling. Loss of fixation was noted in the radiograph of left elbow (Figure 5). A repeat attempt of arthrodesis was done using cross pin fixation augmented with a plaster cast followed by an above elbow brace (Figure 6). Patient was referred to Neurosurgeon for the treatment of his neurological malformation. Foramen magnum decompression with excision of posterior arch of first cervical vertebra was done. His neurological symptoms have improved significantly after the neurosurgical intervention. Four months following the neurological decompression adequate bridging callus was noted across the elbow (Figure 7).
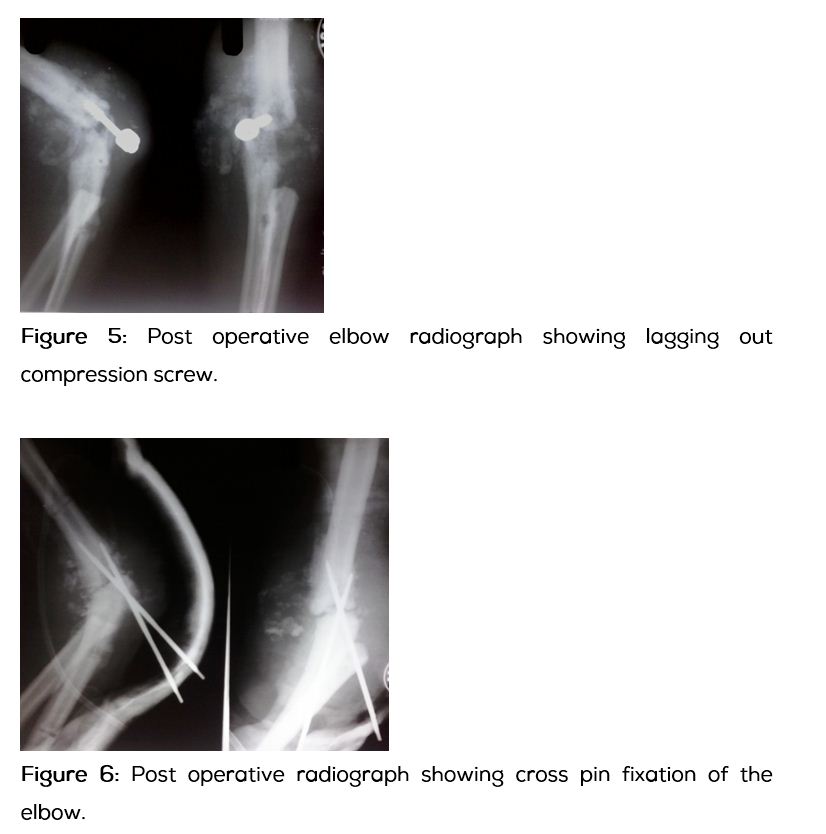
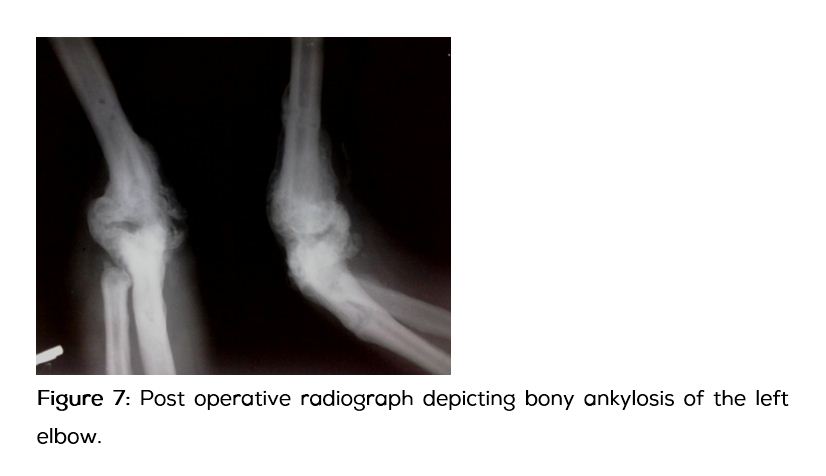
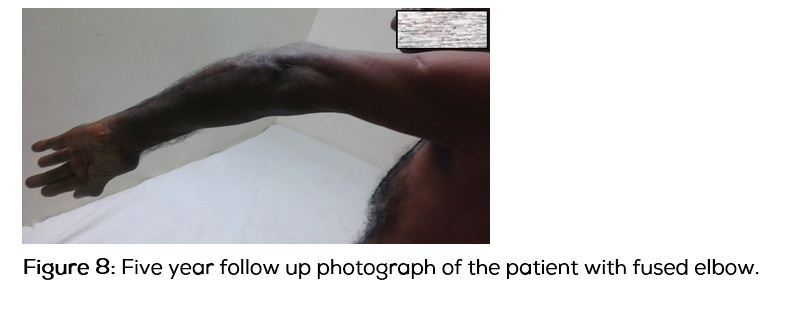
Patient was followed up for five years from the date of initial presentation (Figure 8). Amputation was averted and a functional limb with stable elbow was achieved. He can now perform his routine activities with minimal life style modifications.
Discussion
Neuropathic arthropathy is classically described as a painless lesion but one third of the patients can have pain as in this case [1, 2]. The diagnosis of neuropathic arthropathy can be made only in the presence of an underlying neurological disorder [1]. Syringomyelia is the most common cause of upper limb neuroarthropathies [1] and MRI of cervical spine will aid in its diagnosis. High index of suspicion is essential for the early diagnosis of neuropathic arthropathy [8] and improved outcomes depend on early diagnosis which is often missed [3]. In this case an early MRI of cervical spine would have avoided the delayed and complex presentation.
The classical histopathological feature of neuropathic arthropathy is joint debris located deep in the hyperplastic synovium [1]. Giant cell reaction with hemosiderin pigment often seen in histopathology [1, 8] of neuropathic arthropathy should not be confused with giant cell tumor of tendon sheath which was the case herein before. Proper clinical and radiological correlation of histopathology is essential to avoid misdiagnosis.
Neuropathic arthropathy of elbow presenting as septic arthritis is rarely reported in the literature [2, 4-6] and most of them were managed by debridement and temporary external fixation without any attempt to achieve stability by bony fusion. Elbow arthrodesis is thought to be extremely difficult in a neuropathic joint [1, 4, 7]. Elbow arthrodesis was done in this case in view of delayed presentation with gross instability and infection, as instability and repetitive trauma in an insensate joint leads to the vicious cycle of propagation of bone and joint destruction [1, 8, 9]. The surrounding bony debris consolidated well on stabilisation of the elbow aiding in arthrodesis. The usually followed method of using a pre-bent plate for elbow arthrodesis [7] could not be adopted in this case because of the pre-existing infection.
It is recently reported that early management of primary neurological condition may prevent the progression of neuropathic arthropathy [3]. There is a deficiency in the literature highlighting the necessity of combining the neurosurgical and orthopaedic procedures for effective management of delayed and complicated presentations of neuropathic elbow. Elbow arthrodesis combined with decompression of posterior cranial fossa in this case has resulted in improved functional outcome and bony ankylosis with minimal hardware.
Conclusion
The diagnosis of neuropathic arthropathy of elbow is often missed. The clinical presentation often mimics an aggressive soft tissue tumour. High index of suspicion is essential for the early diagnosis of neuropathic elbow. Thorough neurological examination and MRI of cervical spine should be carried out to detect the neurological and joint pathology precisely. Histopathological evidence of bone and cartilage debris located deep in the hyperplastic synovium adds to the confirmation of diagnosis. It is advisable to initiate appropriate measures early and target both the entities to achieve optimal results. A combination of elbow arthrodesis and foramen magnum decompression may be considered to effectively treat the delayed and complicated presentations of neuropathic arthropathy of elbow secondary to Chiari malformation and cervical syringomyelia.
Consent
Informed consent of the patient is obtained for publication of case details including clinical photographs.
Acknowledgements
We are grateful to Dr. Rapur Siva Prasad, Professor and HOD-Department of Orthopaedics, Mediciti Institute of Medical sciences, Hyderabad for his immense support and guidance.
We thank Dr. Shantveer G Uppin, Consultant pathologist and Associate Professor of pathology, Nizam`s Institute of Medical Sciences, Hyderabad for his critical review of histopathology slides aiding in definitive diagnosis of this case. We thank Dr. Madhulatha. K for proof reading and critical review of the article.
Conflict of interest
The authors declare that they have no conflict of interest.
References
1. Alpert SW, Koval KJ, Zuckerman JD. Neuropathic Arthropathy: Review of Current Knowledge. J Am Acad Orthop. Surg. 1996; 4(2):100–108.
2. Unnanuntana A, Waikakul S. Neuropathic Arthropathy of the Elbow: A Report of Two Cases. J Med Assoc Thai. 2006; 89(4):533–540.
3. Deng X, Wu L, Yang C, Xu Y. Neuropathic arthropathy caused by syringomyelia. J Neurosurg Spine. 2013; 18(3):303–309.
4. Yeap JS, Wallace AL. Syringomyelic neuropathic ulcer of the elbow: Treatment with an external fixator. J Shoulder Elbow Surg. 2003; 12(5):506–509.
5. Ruette P, Stuyck J, Debeer P. Neuropathic arthropathy of the shoulder and elbow associated with syringomyelia: A report of 3 cases. Acta Orthop Belg. 2007; 73(4):525–529.
6. Strike SA, Johnston JC, Farjoodi P. Septic elbow in the setting of neuropathic joint as the initial presentation of a cervical syrinx. Orthopedics. 2011; 34(4):313.
7. Vaishya R, Singh AP, Singh AP. Arthrodesis in a neuropathic elbow after post tubercular spine syrinx. J Shoulder Elbow Surg. 2009; 18(4):e13–16.
8. Sandro Vella, Mario J. Cachia. Charcot neuroarthropathy: Pathogenesis, diagnosis and medical management. Malta Medical Journal. 2008; 20(3):13–19.
9. Bhaskaran R, Suresh K, Iyer GV. Charcot's elbow (a case report). J Postgrad Med. 1981; 27(3):194–196.