Abstract
Purpose: We report a rare case of recurrent conjunctivitis caused by gram positive aerobic microorganism Kocuria varians, which is a nonpathogenic commensal of skin, mucosa and oropharynx.
Methods: A 58-year-old male with diabetes mellitus and hypertension presented to us with both eyes recurrent redness, watering, discharge and burning sensation since 3 months. On examination his best corrected visual acuity (BCVA) was 6/9, N6 in right eye and 6/6, N6 in left eye. On anterior segment examination there was upper and lower lid edema with matting of lashes, diffuse congestion, chemosis and pseudomembranes in both eyes. In view of recurrent conjunctivitis, conjunctival swab was taken and sent for culture and sensitivity.
Results: The organism was identified as Kocuria varians sensitive to chloramphenicol, gentamycin and resistant to levofloxacin. 2 weeks post treatment with chloramphenicol, patient improved symptomatically and repeat culture showed no growth.
Conclusion: With increasing reports of infections associated with these bacteria, it is now important for clinical microbiologists to identify and enumerate the virulence and antibiotic susceptibility patterns of such bacteria and for ophthalmologists in improving the patient care and management.
Keywords: Kocuria varians; recurrent conjunctivitis; immunocompromised individuals; ocular infection; chloramphenicol
Full Text
Introduction
Kocuria spp. are gram-positive cocci which are morphologically similar to both staphylococci and the micrococci, usually found as nonpathogenic commensals of skin, mucosa and oropharynx. Recently there has been a rise in the incidence of infections caused by Kocuria spp. causing both superficial and deep-seated/ invasive infections involving both immunocompromised as well as immunocompetent individuals.
The predisposing factors associated with infections related to Kocuria spp. include congenital deformities (short bowel syndrome), chronic catheterization (in cases of total parenteral nutrition), malignancies (ovarian cancer, gastric cancer, myelodysplastic syndrome, acute myelogenous leukaemia, non-Hodgkin’s disease) and patients with end-stage renal disease undergoing continuous ambulatory peritoneal dialysis. Other underlying conditions associated with Kocuria infection include diabetes mellitus, tuberculosis, stem cell transplant patients, patients suffering from gallstones, methylmalonic aciduria and pancreatic pseudocyst etc. So far Kocuria spp. were found to be associated with include urinary tract infections, cholecystitis, catheter-associated bacteremia, dacryocystitis, canaliculitis, keratitis [1, 2] native valve endocarditis, peritonitis, descending necrotizing mediastinitis, brain abscess and meningitis.
We present a rare case of recurrent conjunctivitis caused by Kocuria varians in a diabetic patient which responded to treatment with chloramphenicol eye drops based on the culture and sensitivity report. With increasing reports of infections associated with these bacteria, it is now important for clinical microbiologists to identify and enumerate the virulence and antibiotic susceptibility patterns of such bacteria and for Ophthalmologists in improving the patient care and management.
Case report
A 58-year-old male visited us with complaints of redness, watering, discharge and blurring of vision in both eyes since last 3 months. He was a known diabetic and hypertensive since last 10 years and on regular medications. Prior to visiting us he was treated with moxifloxacin, loteprednol, tobramycin and prednisolone eye drops without any symptomatic relief. Earlier culture and sensitivity report 2 months following conjunctivitis showed no growth.
At presentation his best corrected visual acuity was 6/9 N6 in right eye and 6/6 N6 in left eye respectively. On slit lamp biomicroscopy examination there was upper and lower lid oedema with matting of lashes, diffuse congestion, chemosis, and pseudomembranes in both eyes. In view of recurrent conjunctivitis conjunctival swabs were taken from both eyes upper and lower fornices and sent for culture and sensitivity. The sample was incubated at 37o C for 48 hours on blood agar, culture on blood agar revealed small round, raised, convex, whitish colony with no haemolysis as shown in Figure 2a. Gram’s stain of the isolated bacterium showed large gram-positive cocci arranged in singles, pairs, short chains, tetrads and clusters as shown in Figure 2b. The isolated bacterium was coagulase negative, catalase positive and was identified as Kocuria varians. Susceptibility testing using Vitek 2 system showed sensitivity to gentamycin (MIC < 4), chloramphenicol (MIC <4) (Figure 3) and resistance to levofloxacin (MIC >8), azithromycin (MIC >2), ciprofloxacin (MIC >4), ofloxacin (MIC >8). Patient was treated with chloramphenicol eye drops and tear substitutes 4 times a day. During 2 weeks follow up patient was symptomatically better with subsidence of lid edema and congestion (Figure 4). Repeat conjunctival swab culture from both eyes after 3 weeks showed no bacterial growth (Figure 5). Thereafter patient was apparently asymptomatic without any history of recurrence with strict glycemic control.
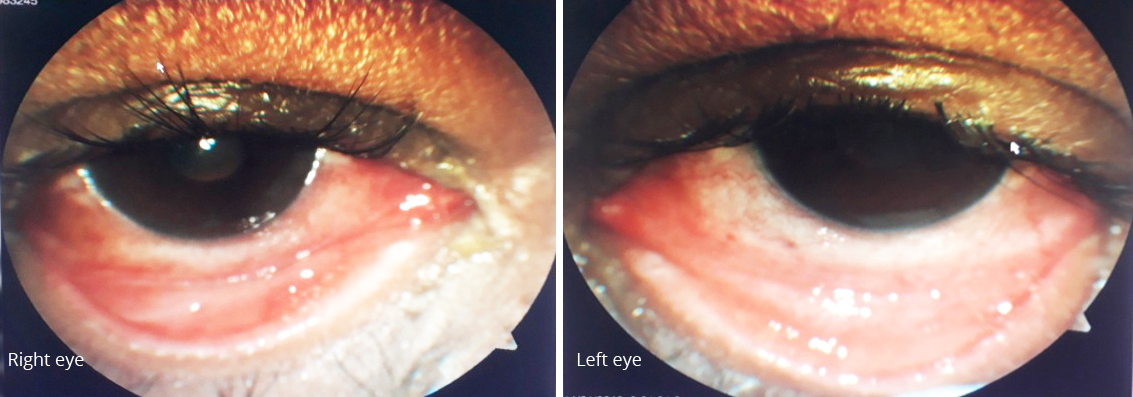
Figure 1: Anterior segment photographs showing chemosis, diffuse congestion and pseudomembrane formation in both eyes.

Figure 2: (a) Blood agar culture plate small round raised, convex, whitish colony with no hemolysis, (b) Gram’s stain of Kocuria varians showing large sized cocci arranged in pairs, short chains, tetrads, clusters.
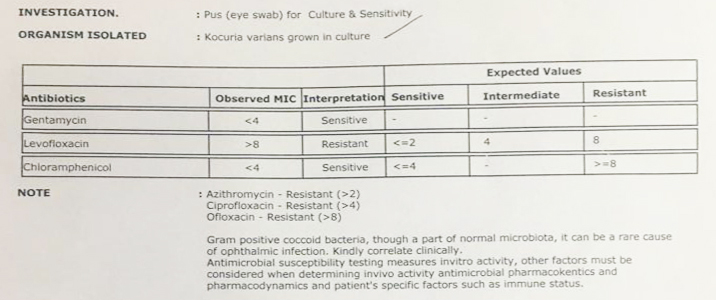
Figure 3: Culture and sensitivity report showing Kocuria varians organism isolated from conjunctival swab and its sensitivity to gentamycin and chloramphenicol.
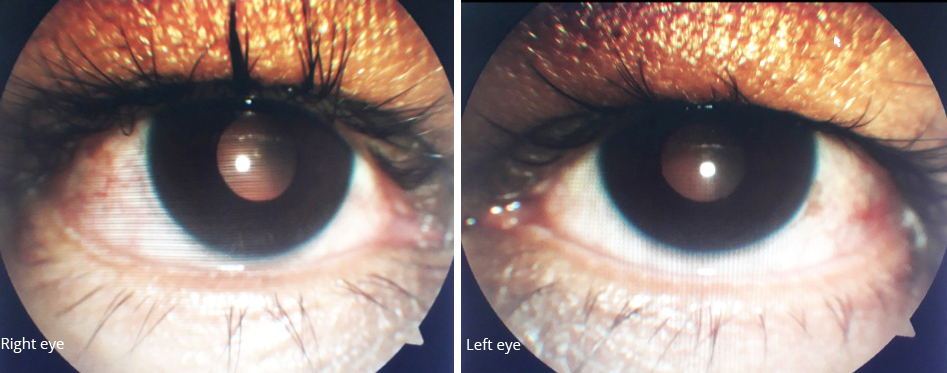
Figure 4: Anterior segment photographs post treatment after 2 weeks.

Figure 5: Culture and sensitivity report showing no growth 3 weeks post treatment.
Discussion
Kocuria spp. is Gram-positive cocci arranged in pairs, short chains, tetrads, cubical packets of eight and irregular clusters. Kocuria belongs to the phylum Actinobacteria, class Actinobacteria, order Actinomycetales, sub order Micrococcinae and family Micrococcaceae [3]. This bacterium was first identified and described by Miroslav Kosur, a Slovakian microbiologist. Currently, there are more than 18 species of Kocuria identified based on the 16S rRNA phylogenetic studies [4]. These are nonpathogenic commensals found on the skin and mucous membrane of human and animals.
In the clinical microbiology laboratory this bacterium is normally misidentified as coagulase-negative Staphylococci (CoNS) based on its gram reaction, catalase positive and coagulase negative properties. Other physiological and biochemical properties of Kocuria are the formation of non-hemolytic colonies on blood agar, non-capsulated, non-spore forming, non-motile, non-acid fast and positive for Voges-Proskauer test (VP). It has also been observed that various species of Kocuria react differently to routine biochemical tests like the oxidase, amylase, urease, citrate utilization test, gelatinase, phosphatase tests, utilization of inulin, arabinose, N-acetyl-L-glutamic acid, and nitrate reduction test [5]. This could be attributed to the reason behind the inaccurate identification by both conventional and an automated bacterial identification systems. With the availability of new automated identification systems that include VITEK (BioMe´rieux Inc., Durham, NC, USA), VITEK 2 (BioMe´rieux Inc., Durham, NC, USA), API (BioMe´rieux Inc., Durham, NC, USA) and the BD Phoenix™ Automated Microbiology System (BD Diagnostic Systems, Sparks, MD) identification systems, it is now possible to differentiate Kocuria from CoNS and identify all species of Kocuria [6]. In the case of non-availability of molecular and advanced laboratory methods, Kocuria can still be identified and differentiated from Staphylococci and Micrococci using morphological, cultural characteristics and differential antibiotic discs.
Infections of Kocuria spp. normally involve patients with various debilitated conditions. In the era of drug resistance, and prevalence of multi-drug resistant bacteria, occurrence of Kocuria spp. in hospitalized patients should not always be ignored as contaminants [7]. Further studies emphasizing the determination of the virulence, pathogenic potential, predisposing factors and antimicrobial susceptibility patterns of Kocuria spp. are warranted. A recent research report has highlighted the significance of Kocuria in causing hospital-acquired infections. The same study has also noted that although Kocuria spp. are commensals of humans, animals and are present in the environment, they should be considered as potential pathogens in patients who are immunocompromised, undergoing critical care treatment and neonates.
Conclusion
To the best of our knowledge, this is a rare case report of recurrent conjunctivitis caused by Kocuria varians in a diabetic and hypertensive patient. Precise strain diagnosis and accurate determination of the antimicrobial susceptibility to unusual organisms causing bacterial conjunctivitis are important for the effective treatment of it. In conclusion, ophthalmologists should be aware of Kocuria keratitis could be sight threatening corneal complication of Kocuria conjunctivitis, and that rapid diagnosis and treatment of Kocuria conjunctivitis may improve the visual prognosis and provide symptomatic relief.
Acknowledgement
Our sincere thanks to Dr. Anil Kumar Bilolikar, Senior Consultant, Microbiology Department, Dr. Poonam and all Microbiology department staff for their co-operation and support. We are also thankful to all optometrists and staff of Ophthalmology department.
Conflict of interest
Authors declare no conflict of interest.
References
[1] Matterm RM, Ding J. Keratitis with Kocuria palustris and Rothia mucilaginosa in vitamin A deficiency. Case Rep Ophthalmol. 2014; 27:72–77.
[2] Pedro-Aguilar L, Ramirez-Miranda A, Bautista-de Lucio VM, Navas A, Ortiz-Casas M, et al. Epidemiology and outcomes of kocuria keratitis. Eye Contact Lens. 2016; 42(5):e20–24.
[3] Stackebrandt E, Koch C, Gvozdiak O, Schumann P. Taxonomic dissection of the genus Micrococcus: Kocuria gen. nov., Nesterenkonia gen. nov., Kytococcus gen. nov., Dermacoccus gen. nov., and Micrococcus Cohn 1872 gen. emend. Int J Syst Bacteriol. 1995; 45(4):682-692.
[4] Park EJ, Kim MS, Roh SW, Jung MJ, Bae JW. Kocuria atrinae sp. nov., isolated from traditional Korean fermented seafood. Int J Syst Evol Microbiol. 2010; 60:914–918.
[5] Savini V, Catavitello C, Masciarelli G, Astolfi D, Balbinot A, et al. Drug sensitivity and clinical impact of members of the genus Kocuria. J Med Microbiol. 2010; 59 (Pt 12):1395–1402.
[6] Boudewijns M, Vandeven J, Verhaegen J, Ben-Ami R, Carmeli Y. Vitek 2 automated identification system and Kocuria kristinae. J Clin Microbiol. 2005; 43(11):5832.
[7] Lee MK, Choi SH, Ryu DW. Descending necrotizing Mediastinitis caused by Kocuria rosea: a case report. BMC Infect Dis. 2013; 13:475.