Full Text
Introduction
Normal mineralization of bones and formation of dental enamel depend upon fluorine partially. Fluorine is amply available in nature. The human body contains 96% fluoride in bones and teeth. The biological half life of fluoride in bone is about 20 yrs. The factors that influence musculoskeletal changes due to excess of fluorides include endemic areas, age, diet, drinking water, dose, duration and hormonal responses. Consumption of drinking water from wells, food from sea fish, vegetables grown in fluoride area and milk from the cattle, influence the extent of fluorosis. This is a public health problem and is preventable. If detected early it is curable.
About 66 million people in India drink water containing elevated levels of fluoride. Inhalation of fluorine in aluminum industrial workers and farmers using fertilizers may also get fluorosis. When a mother is exposed to excess of fluorides, the infant may have respiratory distress. Fluorosis is endemic in 20 states in India. Andhra Pradesh, Gujarat and Rajasthan are the major centres (Figure 1).
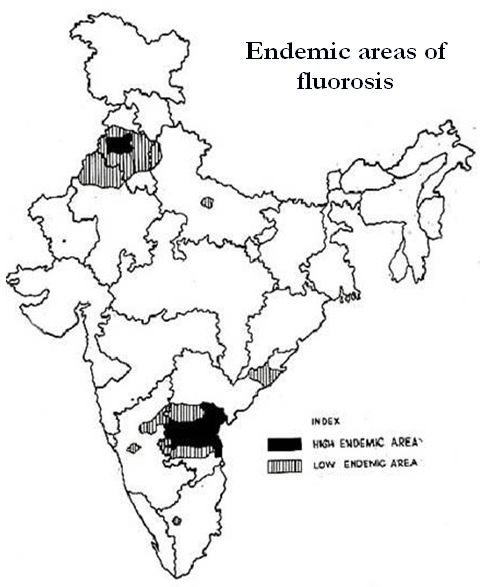
Figure 1: Endemic areas of fluorosis in India; Other centers include north, south and eastern states of India.
Pathophysiology
Continuous intake of 2.5mg of fluoride for more than six months deposits, four thousand to six thousand mg per kg of fluoride which causes detectable radiological changes in musculoskeletal system. The hydroxyapatite in bone is altered in size and structure of its crystal. The fluoroapatite crystal decreases the mechanical competence of the bone. The poor quality of bone results in fractures and osteoarthritis. Musculoskeletal fluorosis is aggravated by deficiency in calcium and vitamin ‘D’ particularly in children.
The histology presents as cement lines, increased osteocytes, disoriented lamellae, altered enzymatic action and poorly formed Haversian system.
Radiological findings
Musculoskeletal fluorosis involves all the bones from head to toe. The paraarticular soft tissue structures that are involved include musculotendinous areas, ligaments, fascia, bursae and other structures.
In the skull, calcifications of petroclinoid ligaments, diaphragma sella, ligamentum nuchae etc., are observed. In the calvarium, diploic thickening prominent occiput and frontal ridges are noted (Figure 2).
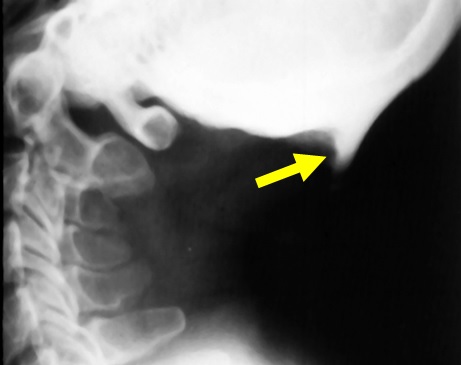
Figure 2: Fluorosis with occipital exostotic ossification; Sutural sclerosis and irregular narrowing of foramen magnum are also present.
In children and women, rickets and osteomalacia are present due to deficiency of calcium and vitamin ’D’. Rachitic changes include widening of the physies and metaphyseal cupping (Figure 3a). Stress lines may be detected depending upon the health status of the child (Figure 3b).
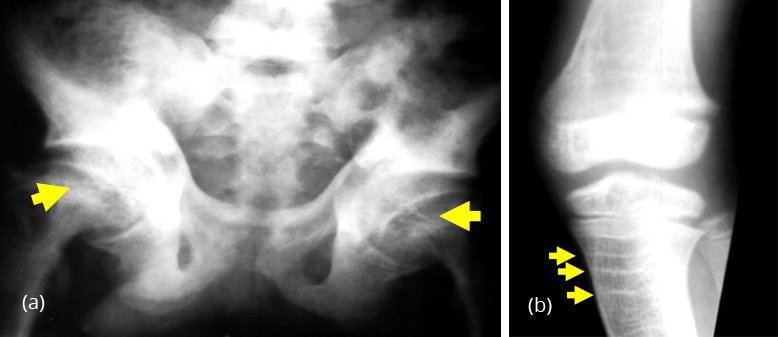
Figure 3: (a) 12 yr old - Fluorosis with rickets. Note widening of physes, (b) Rickets + Stress lines.
In adults, osteomalacia is noted as ground glass appearance of bones which are soft with Looser zones (Figure 4).
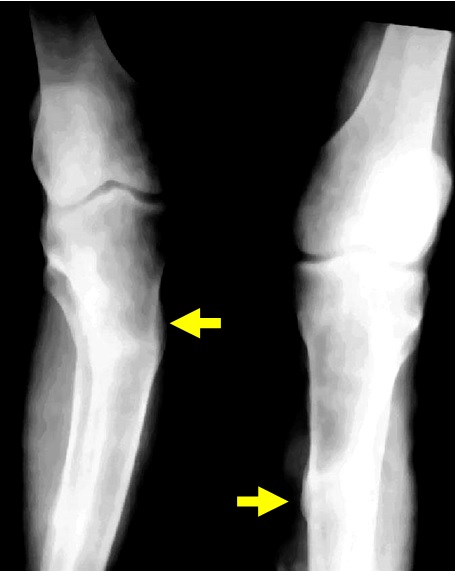
Figure 4: Fluorosis - Healing looser zones.
In adults, diffuse sclerosis of the axial skeleton with enthesopathy, calcification of the paravertebral limgaments and ligamentum flava are noted (Figure 5a,b). In the cervical spine, the anterior longitudinal ligament may have flowing hyperostosis simulating diffuse idiopathic skeletal hyperostosis (DISH) (Figure 5c).

Figure 5: (a) Fluorosis – C. Spine, (b) Lateral - C. spine. (c) Fluorosis with flowing ossification of anterior longitudinal ligament simulating idiopathic skeletal hyperostosis.
In the thoracic spine diffuse sclerosis with enthesopathy is noted (Figure 6ab).
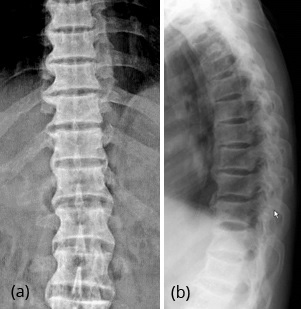
Figure 6a, b: Fluorosis – Thoracolumbar spine with sclerosis and enthesopathy.
Ossification of ligamentum flava may produce pressure effects on spinal cord. Degenerative changes may be super imposed in spine. Early on, osteoporosis may be noted. In the thoracic cage, the ribs show diffuse sclerosis with saw tooth like appearance in the superior and inferior borders due to calcification at the attachment of intercostal muscles and interosseous membranes (Figure 7a,b).
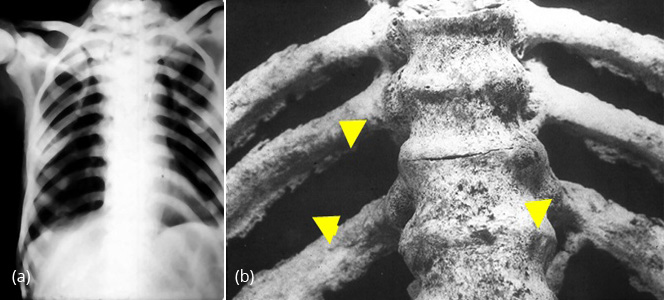
Figure 7: (a) Fluorosis thoracic cage, (b) Fluorosis specimen - Interosseous muscular attachments.
In the pelvis, ligamentous calcification is noted in obturator membrane, sacrospinous, sacrotuberous and paraarticular ligaments. Lumbosacral limgament is also ossified. These appearances depend upon the degree of toxicity. Bony excrescencies simulating exostosis are noted in the iliac crest. Ischial tuberosities and bony protuberances. The ischial changes show simulating “whiskerng” noted in ankylosing spondylitis (Figure 8 abcd).
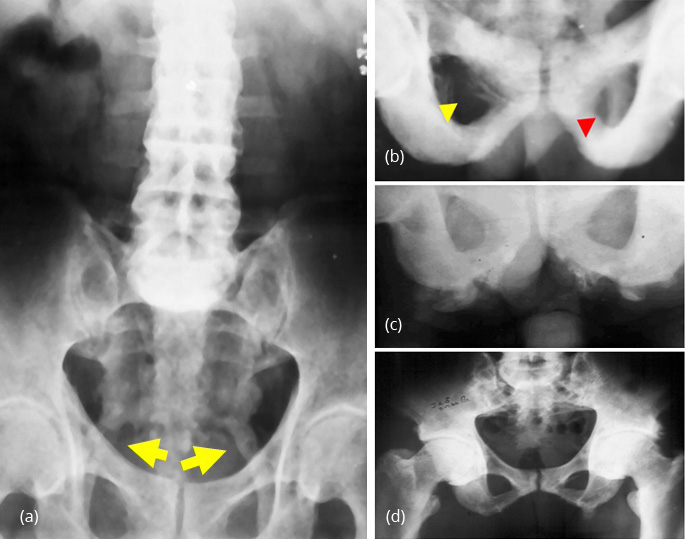
Figure 8: (a) Fluorosis - Calcified sacrospinal and sacrotuberous ligaments, (b) Fluorosis – Calcification of the obturator membrane and ischiosacral ligament, (c) Fluorosis - Exuberant enthesopathy at ischial tuberosities, (d) Fluorosis + degenerative changes in hip joints and ischial enthesopathy.
The appendicular skeleton shows variable changes depending upon the stage of fluorosis. The primary trabeculae appear to be rough and sclerotic. These thick primary trabecuale merge with secondary trabecuale to make bones homogenously dense. The contours of bone are uneven due to subperiosteal new bone opposition. The long bones of the limbs show encroachment of the medullary cavities with endosteal new bone. Calcification of the interosseous membrane of the forearm is classical of fluorosis, although it may be occasionally noted in diffuse idiopathic skeletal hyperostosis. Sclerotic changes and periosteal proliferation in the bones of the forearm and hand are common and periosteal proliferation may simulate exostoses (Figure 9a). Pathological fractures of banana type may noted (Figure 9b).
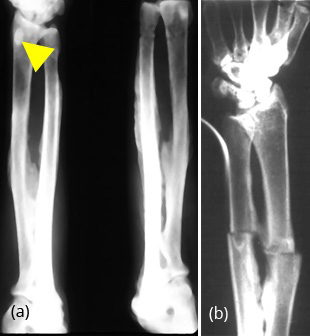
Figure 9: (a) Fluorosis with calcification of the interosseous membrane with exostosis of radius, (b) Fluorosis with banana type of fractures of radius and ulna.
Often, degenerative changes are noted in the knee joints with calcification of paraarticular structures and tendons resulting in deformities (Figure 10a,b,c).
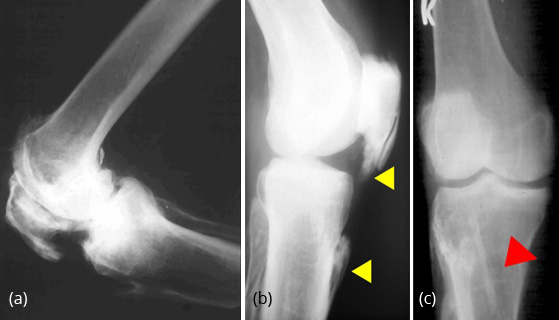
Figure 10: (a) Advanced degenerative changes with flexion deformity of knee, (b) Fluorosis - Calcification of patellar and infra patellar tendon, (c) Fluorosis with osteoporosis. Calcification of soleal line with periosteal exostosis.
In the bones of the foot and ankle, similar changes are noted with extensive calcification/ ossification at the insertion of tendoachilles at the calcaneum (Figure 11).
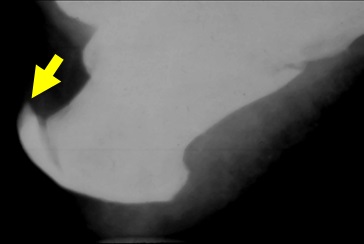
Figure 11: Fluorosis with dorsal calcaneal spur In the teeth, white patches on enamel, faint yellow lines leading to brown stain and pitting of enamel with clipped of edges are noted.
Ct imaging
CT is the best imaging modality to study the bone pathology (Figure 12).
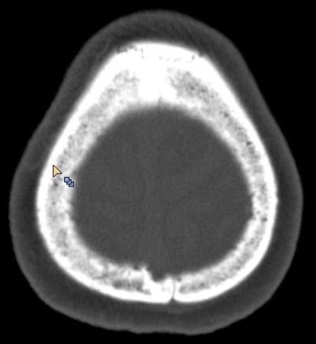
Figure 12: Fluorosis – CT skull showing diffuse sclerosis.
It shows enthesopathy and calcification of the ligaments (Figure 13).
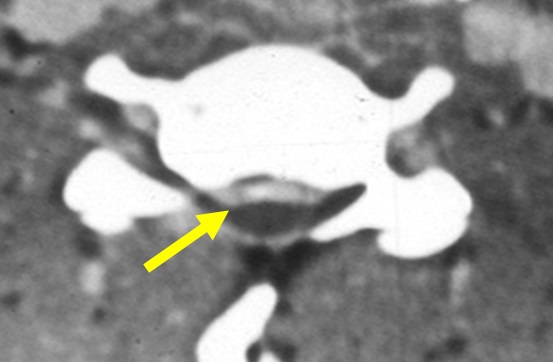
Figure 13: Fluorosis CT – C. Spine - Ossification of posterior longitudinal ligament (arrow) (OPLL).
Spinal and root canal stenosis are well appreciated with concomitant changes in the spinal cord. The facet joints and the calcification of ligamentum flava are well depicted (Figure 14a,b).
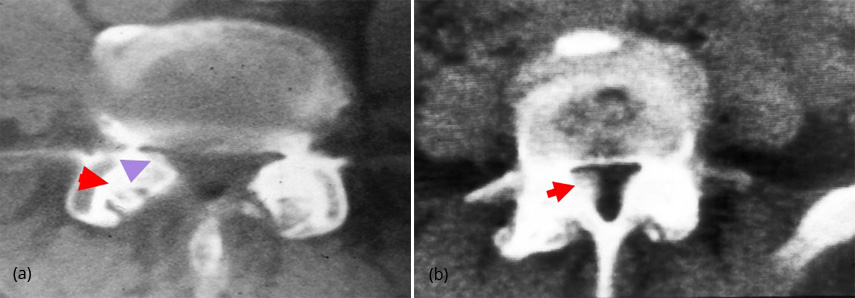
Figure 14: (a) Fluorosis CT – Lumbar canal stenosis with calcified ligamentum flavum, (b) Fluorosis CT – Lumbar canal stenosis with calcified ligamentum flavum.
MRI imaging
Although it is costly, it is non invasive and radiation free. Spinal cord changes as well as the soft tissues are well demonstrated. The spinal cord changes are mainly due to prolonged compression and secondary vascular compromise producing myelomalacia. Fluorotic vertebrae are hypointense in both T1 & T2 weighted images. Myelomalacia, cavitation and necrosis show high intensity signal in T2 weighted images (Figure 15a,b,c,d).
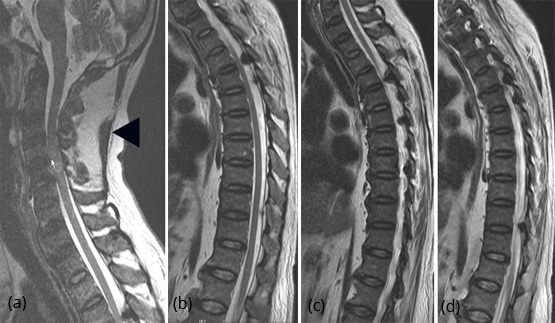
Figure 15: (a) Fluorosis MRI – C. Spine. Note the ischemic changes in the cord and ossification of ligamentum nuchae (Black arrow), (b) Fluorosis MRI – Extensive calcification of ligamentum flava, (c, d) Fluorosis MRI – Extensive ossification of ligamentum flava with compression of the cord.
Scintigraphy
Radionuclide bone scans are mostly performed by technetium labeled methylene diphosphonate. It mostly shows super scan and in most cases joint abnormalities. The tracer concentration is high in the articular margins. In general, scintigraphy is useful in displaying skeletal fluorosis.
Differential diagnosis
Myelofibrosis, osteoblastic metastasis, renal osteodystrophy, ankylosing spondylitis, Paget’s disease etc., are to be considered. Sclerosing dysplasias are diagnosed by skeletal survey.
Complications
The complications include degenerative arthritis, degenerative spondylosis, pathological fractures, neurological abnormalities and secondary hyperparathyroidism.
Conclusion
Fluorosis is a public health problem which is preventable. The radiological changes of musculoskeletal fluorosis depend upon the stage of fluorosis. Conventional radiology is the basic screening method. CT and MRI are helpful to detect changes in the spinal cord. CT detects early calcification better than conventional radiology. MRI helps in the study of changes in the spinal cord. If detected early, the skeletal changes are reversible.
Conflicts of interest
Author declares no conflicts of interest.
References
1. Christie DP. The spectrum of radiological bone changes in children with fluorosis. Radiology 1980, 136:85.
2. Dandona P, Menon RK, Shenoy R, Houlder S, Thomas M, et al. Low 1,25-dihydroxyvitamin D, secondary hyperparathyroidism, and normal osteocalcin in elderly subjects. J Clin Endocrinol Metab 1976, 63:459.
3. Gruber HE, Baylink DJ. The effects of fluoride on bone. Clin Orthop Rel Res 1991, 267:264–277.
4. Jolly SS, Singh BM, Mathur OC. Endemic fluorosis in Punjab (India). Am J Med 1969, 47:553.
5. Krishnamachari KAVR. Further observations in syndrome of endemic genu valgum. Ind J Med Res 1976, 64:284.
6. Krishnamachari KAVR, Krishnaswamy K. Genu valgum and osteoporosis in an area of endemic fluorosis. Lancet 1973, 2:887.
7. Naidu MR, Sastry KV, Reddy PK, Reddy DR. Skeletal fluorosis secondary to occult renal disease. Fluoride 1986, 19:166-168.
8. Pandit CG, Raghavachari TN, Rao DS, Krishnamurthi V. Endemic fluorosis in south India. Indian J Med Res 1940, 28:533-558.
9. Raja Reddy D, Srinkath DR, Fluorosis in Andhra Pradesh – Fluorosis Vimukthi-2012.
10. Raja Reddy D. Neurology of endemic skeletal fluorosis Department of Neurosurgery, Room No. 39, Apollo Hospital, Jubilee Hills, Hyderabad - 500 033, India.
11. Rhyan, International fluorosis diagnosic counseling centre, New Delhi, India, Email: fr_rtf@gmail.com.
12. Reddy DR. Some observations of fluoride toxicity. NIMHANS J 1985, 3:79-86.
13. Reddy DR, Deme SR, Sesikaran B, Krishnamurthi D, Rao SH, et al. Muscle and nerve pathology in skeletal fluorosis, Reprinted from: 11th International congress of neurological surgery. Amsterdam The Netherlands: July 6-11, 1997, p.2125-2132.
14. Reddy SG, Rao NBS. Effect of dietary calcium, vitamin C and protein in development of experimental skeletal fluorosis. II. Calcium turnover with 45Ca; calcium and phosphorus balances. Metabolism 1971, 20:650.
15. Reddy DR, Skeletal fluorosis. In: Vinken PJ, Bruyn GW, editors. Handbook of clinical neurology. Vol. 36. Amsterdam: North Holland Publishing Co; 1979. p. 465-504.
16. Sesikaran B, Harinarayanan Rao S, Krishnamurthi D, Reddy DR. Studies on skeletal muscle biopsies in endemic skeletal fluorosis. Neurol India 2000, 48:187-198.
17. Shortt HE, McRobert GR, Barnard TW, Nayar AS. Endemic fluorosis in the Madras presidency. Indian J Med Res 1937, 25:553-568.
18. Siddique AH. Fluorosis in Nalgonda district, Hyderabad, Deccan. Br Med J 1955, 2:1408.
19. Teotia SPS, Teotia M. Secondary hyperparathyroidism in endemic fluorosis. Br Med J 1973, 1:637.
20. Teotia M, Teotia SPS, Kunwar KB, et al. Endemic skeletal fluorosis, Arch Dis Child 1971, 46:686-691. doi:10.1136/adc.46.249.686.
21. World Health Organization. Environmental Health Criteria 227, Fluorides, Geneva: W.H.O. 2002. p.14-16.