Full Text
As the Science is advancing the complications are also on the increase. The incidence of placenta percreta has increased and seems to parallel the Incidence of cesarean section rate. Incidence of adherent placenta is one in 533 pregnancies for the period of 1982-2002, which was one in 4027 in 1970s. The increasing scars on the uterus as a result of any procedure like myomectomy, excision of the rudimentary horn, conservative surgery for partial ruptures, also contributory to the present status to encounter more number of cases of adherent placenta.
Here is a case of placenta percreta in our Institute of Obstetrics and Gynecology Department, KGH., Visakhapatnam.
Case report
A 31 year old female was admitted on 27 January 2015 in KGH in view of post cesarean pregnancy, hypothyroidism complicating pregnancy with cervical stitch in situ for safe institutional delivery.
On admission she was 37 weeks period of gestation with breech presentation. Her last menstrual period (LMP) was 10.5.2014 and estimated due date (EDD) was 17.2.2015. Her marital life was 9 years and was non consanguineous. Her first 5 pregnancies were spontaneous conceptions, ending in spontaneous abortions in the 1st trimester. She underwent surgical evacuation for all miscarriages. All pregnancies occurred with a gap of 6 months. Her 6th pregnancy was also spontaneous, had regular antenatal checkups, supported by drugs probably hormones, had cervical enciclage at the end of 3rd month She had cesarean section in view of PPROM (preterm PROM) at 36 weeks with precious pregnancy, in KGH, Visakhapatnam, delivered alive Mch wt. 2 kgs and the age of child is 6 yrs. Intraoperatively placenta acreta (Figure 1) was diagnosed, placenta was left in situ and given methotrexate. There was history of expulsion of placenta 25 days after surgery at home. Her 7th pregnancy was again spontaneous conception, 4 years after previous LSCS, MTP was done at KGH, 1 ½ years back.
Her 8th pregnancy is the present one, spontaneous conception. She had regular antenatal checkups in a remote rural private hospital in this pregnancy. She was having hypothyroidism for the past 3 years and was using tablet eltroxin 150mg/day. Cervical encirclage was done at the end of 12 weeks. She was on injectable as well as oral progesterone and also on duvadilan till 9th month.
On examination her general condition was fair, vital data are normal. On per abdominal examination, pfannenstiel scar was present, uterus term, breech, FHS good, uterus relaxed. On P/V Cx tubular, OS closed, cervical stich was in situ, pp breech high up, and outlet contraction was present.
She was investigated for routine preoperative, haematological and thyroid function tests. Ultrasonography showed SLF, breech, 37 weeks, 2.4 kgs AFI-7, placenta fundal & anterior grade II. With suspicion of placenta percreta MRI was done, which showed gravid bicornuate/ arcuate uterus in breech presentation with fundal placenta along right lateral aspect. Thinned out myometrium with subtle loss of interface between placenta and myometrium along left lateral aspect of placenta. Heterogenous placenta with T2W hypointense areas – suggestive of intermediate possibility of placenta accreta. Uterine serosa is intact.
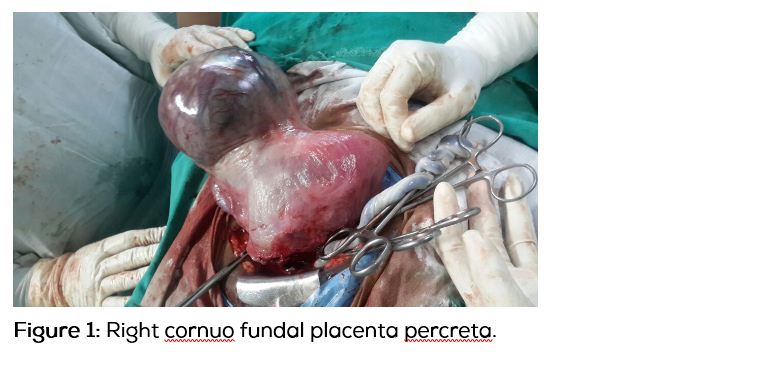
Elective cesarean Hysterectomy is planned with 2 Units of blood, after taking consent for Hysterectomy and high risk is explained to the attendants. Under spinal anesthesia, the abdomen was opened. Baby was presented as breech. Delivered alive female child of birth weight 3.2 kg with Apgar–10. After watching for 3 minutes for placental separation, as there no spontaneous expulsion, Uterus was delivered out of incision, a 15x15 cm (fetal head size) bulge over the right side of the fundus was noticed. It was nothing but blood filled sac covered with serosa. Placenta is adherent to the serosa. Placenta percreta is diagnosed and proceeded for Total Hysterectomy (Figures 2 and 3), after securing haemostatis at the cut edges of uterine incision. On cut section 1/3rd of the placenta is in the sac. Uterus was arcuate. Specimen was sent for Histopathological confirmation.
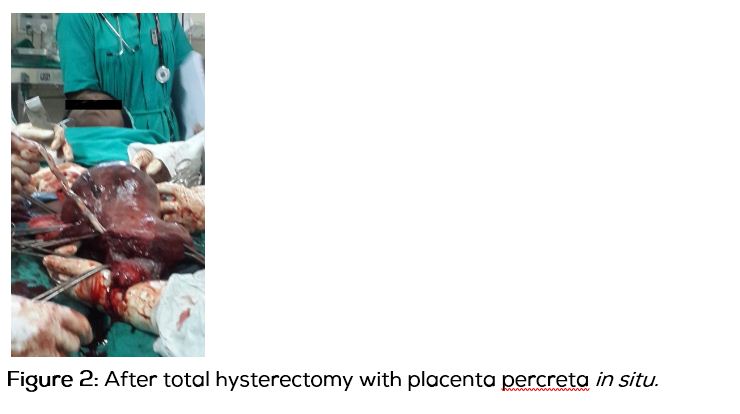
Pathology report showed placental villi invading the total myometrium of the uterus. Features are suggestive of placenta percreta. Postoperative period was uneventful. Patient was dischaged on 9th po day in good condition.
Discussion
Morbidly adherent placenta is defined as an abnormal adherence either in whole or in part of the placenta to the under lying uterine wall. Based on depth of adherence, the adherent placenta are classified as accreta (villi are attached to the myometrium) Increta (villi invade the myumetrium) and percreta (villi invades up to serosa or into adjacent organs) [1, 2].
Frequencies of occurrence of these types are: Accrete - 79%; Increta - 14%; Percreta - 7%.
Depending on the extent of placental tissue involved sub types are total (entire placenta is adherent) partial (some portions of the placenta are adherent) and focal (a single cotyledon is adherent). The occurrence of adherent placenta in an unscarred uterus is rare. But the implantation sites at risk for adherent placenta include Sub Mucous fibroids, rudimentary horn and uterine cornua.
Adherent placenta can occur in any condition resulting in myometrial tissue damage followed by a secondary collagen repair such as i) Prior uterine surgery (cesarean section, Uterine curettage, Myomectomy, Manual removal placenta and treatment for Asherman syndrome, Thermal ablation and uterine artery embolisation). Approximately 50% of pregnancies complicated by accreta are preceeded by a cesarean delivery in a prior pregnancy); ii) Advancing maternal age: Women above the age of 35 years are estimated to have a 5 times increased risk of adherent placenta; iii) Increasing parity; iv) placenta previa; v) Prior placenta accrete: Recurrence rate of placenta accrete ranges from 18–29%. Therefore prior placenta accrete may be a major risk factor as well.
Treatment of placenta percreta is caesarian hysterectomy, electively at 36wks. Attempt at removal of placenta before hysterectomy increases morbidity.Preoperative (after delivery of baby) bilateral uterine artery ligation may reduce morbity. There is no benefit from internal artery ligation. Placenta accrete is the leading cause for PPH & emergency hysterectomy. Maternal mortality can be as high as 7 – 10%. There may be perinatal complications related to preterm births, as well.
Conclusion
Antenatal diagnosis of adherent placenta requires a high index of suspicion. 95% of women with morbidly adherent placenta have identifiable risk factors. However no diagnostic test offers 100% assurance either of ruling in or ruling out the presence of placenta accreta. A definitive diagnosis is made intra operatively and histologically. A multi-disciplinary approach with surgical expertise, availability of transfusion facilities and further interventions including interventional radiology is essential and may result in reduced maternal mortality and morbidity. Early identification of patients with risk factors is essential for an effective management plan. Antenatal diagnosis relies on a high degree of suspicion and can be made by characteristic ultra sound & MRI finding in women with risk factors. Elective cesarean hysterectomy at an appropriately equipped Institution is the treatment of choice.
References
1. World Clinics Obstetrics & Gynecology. 2012; 2(2):217.
2. Wu S, Kocherginsky M, Hibbard JU. Abnormal placentation: twenty-year analysis. Am J Obstet Gynecol. 2005; 192(5):1458–1461.
3. Daskalakis G, Anastasakis E, Papantoniou N, Mesogitis S, Theodora M, et al. Emergency obstetric hysterectomy. Acta Obstet Gynecol Scand. 2007; 86(2):223–227.
4. Eller AG, Porter TF, Soisson P, Silver RM. Optimal management strategies for placenta accreta. BJOG. 2009; 116(5):648–654.