Full Text
Introduction
Severe acute respiratory syndrome corona virus 2 (SARS-CoV-2) is a novel strain of corona virus that has not been previously identified in humans. It has been declared a pandemic by WHO on 11-3-2020 [1] and has infected at least 1,48,000 as on September 9th 2020. Transmission among humans occurs via close contact with an infected individual that produces respiratory droplets while coughing or sneezing within a range of about 6 ft (Ghiana et al. 2020). Patients have been shown to undergo acute respiratory distress syndrome, which is defined as cytokine storm. The diagnosis relies on detection of nucleic acid, IgG/IgM antibodies and computerised tomography scan (CT) of the suspected individuals. The genome of SARS-CoV-2 is similar to other corona viruses that comprise of ten open reading frames (ORFs). SARS-CoV-2 spike protein exhibits higher affinity to ACE2 receptor as compared with SARS-CoV. Transmission among humans occurs via close contact with an infected individual that produces respiratory droplets .The diagnosis of corona virus disease 2019 (COVID-19) was determined with at least two positive results of real-time reverse transcriptase-polymerase chain reaction (RT-PCR) assay for SARS-CoV-2. Patients absent of or with negative SARS-CoV-2 test results were also excluded from this study. The COVID-19 pneumonia has been classified to four types clinically for diagnosis and treatment of COVID-19 infection by the National Health Commission [2].
The classification of the four clinical types is as follow:
(1) Mild: Symptoms very mild, no pneumonia manifestation in CT;
(2) Ordinary: Fever, respiratory tract symptoms, and pneumonia manifestation in CT scan;
(3) Severe: Respiratory distress (respiratory rate > 30/min), oxygen saturation ≤ 93% at rest, and PaO2/ FiO2 ≤ 300 mmHg;
(4) Critical: Respiratory failure need mechanic ventilation, shock, and combined multi-organs failure.
After diagnosis of COVID-19 with symptomatology, laboratory medicine plays an important role for the disease diagnosing and monitoring its progression.
Many cytokines take part in the “cytokine storm” in COVID-19 patients, including IL-6, IL-1, IL-2, IL-10, TNF-α and IFN-γ; however, a crucial role seems to be played by IL-6, whose increased levels in the serum have been correlated with respiratory failure, ARDS, and adverse clinical outcomes [3] (Figure 1).
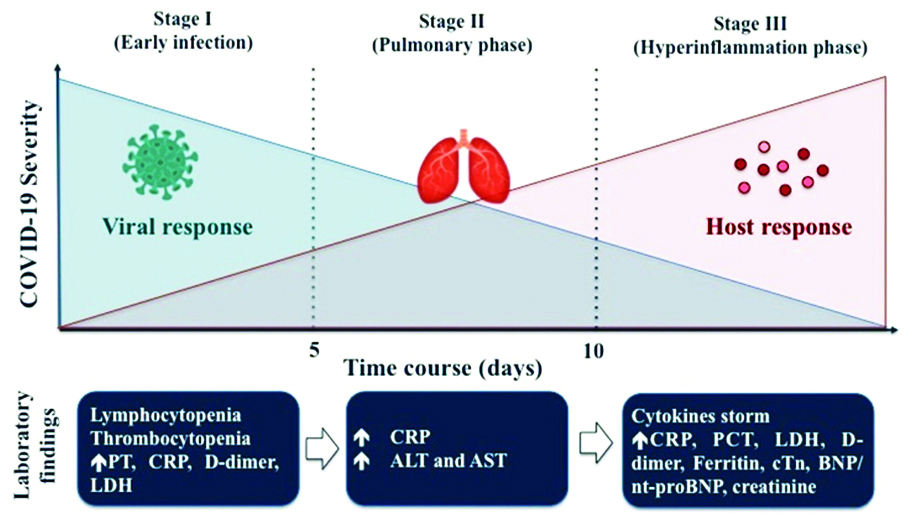
Figure 1: Laboratory findings – COVID-19 severity.
In the laboratory medicine, biochemical parameters help in diagnosis, monitoring, prognostication and therapeutic guide for the patient (Table 1).
Table 1: Laboratory parameter changes in COVID -19.
|
Haematological
|
↑WBC count
↑ neutrophil count
↑Lymphocyte count
↓Platelet count
↓Eosinphil count
↓Hemoglobin
|
|
Biochemical
|
↓Albumin
↑Alanine transferase
↑Aspartate transferase
↑Total bilirubin
↑Blood urea nitrogen
↑Creatinine
↑Creatinine kinase
↑ Lactate dehydrogenase
↑Myoglobin
↑CK-MB
|
|
Coagulation
|
↑Prothrombin time
↑ D-Dimer
|
|
Inflammatory biomarkers
|
↑ESR
↑CRP
↑Serum ferritin
↑PCT
↑IL-2R/IL-6/IL-8/IL-10
|
Coagulation profile and inflammatory biomarkers
Coagulation profile includes PT, aPTT, fibrinogen, D-dimer. COVID-19 patients exhibited a hypercoagulable state, featured by prolonged prothrombin time, elevated levels of D-dimer and fibrinogen, and near normal activated partial thromboplastin time. A few patients would finally progress to overt disseminated intravascular coagulation (DIC). Tang et al. reported that 71.4% of non-survivors and 0.6% of survivors of COVID-19 showed evidence of overt DIC. Indeed, more patients exhibited latent DIC characterized by a hypercoagulable state, as demonstrated by fibrin thrombus formation in post-mortem examination. A high proportion of acro-ischemia was also observed in deteriorating patients with COVID-19, indicating a hypercoagulable status before the final onset of overt DIC.
Inflammatory markers
The persistent inflammatory status in severe and critical COVID-19 patients acts as an important trigger for the coagulation cascade. Certain cytokines including IL-6 could activate the coagulation system and suppress the fibrinolytic system. In the setting of COVID-19, pulmonary and peripheral endothelial injury due to direct viral attack might be an equally important inducer of hyper coagulation. Endothelial cell injury can strongly activate the coagulation system via exposure of tissue factor and other pathways. Moreover, aggressive immune response could also be augmented by dysfunctional coagulation. These two processes may act in a feed-forward manner towards an uncontrolled endpoint. In addition, the emergence of antiphospholipid antibodies may intensify the coagulopathy. Various levels of anti-cardiolipin and anti-β2GP1 antibodies were detected in our COVID-19 patients.
Cytokines are vital in regulating immunological and inflammatory responses. Among them, IL-6 is of major importance because of its pleiotropic effects [4]. Circulating IL-6 are closely related to severity of COVID-19 infection. An increase in IL-6 levels has previously been observed in patients with respiratory dysfunction [5], implying a possible shared mechanism of cytokine-mediated lung damage caused by COVID-9 infection. Furthermore, it seems that the highly pathogenic SARS-CoV-2 is associated with rapid virus replication and a tendency to infect the lower respiratory tract, resulting in an elevated response of IL-6-induced severe respiratory distress. The serial measurement of circulating IL-6 levels are important in identifying disease progression among COVID-19-infected patients.
Cytokines are small proteins that regulate immune, Inflammatory and hematopoietic processes. The elevated leucocytosis seen in several infections with an absolute neutrophilia is due to IL1 and IL6. Pyogenic cytokines (Figure 2) as IL1, IL6, TNF, CNTF (ciliary neutropic factor) and interferon alpha encoded by separate gene cause fever. These pyogenic cytokines are released from the cells and enter systemic circulation on infection and induce fever by causing release of PGE2. The release of PGE2 into peripheral circulation causes myalgia and arthralgia along with fever. Release in systemic circulation causes raise in hypothalamic set point for raise of core temperature. The risk of respiratory failure for patients with IL-6 levels of ≥ 80 pg/ml was 22 times higher compared to patients with lower IL-6 levels. In the current situation with overwhelmed intensive care units and overcrowded emergency rooms, correct triage of patients in need of intensive care is crucial.

Figure 2: Cytokine storm.
Liver function tests
Compared to patients with normal liver tests at admission, those who had abnormal liver test results, especially in hepatocyte type or mixed type, had significantly higher risks of developing severe pneumonia. As almost all patients had liver tests at admission, liver test abnormalities can be used as a predictor for the severity of the disease. More than 90% of patients with abnormal liver tests were mild at admission and about 24% of them developed increased ALT and GGT levels to substantially more than 3× ULN during hospitalization. However, the increase in AST and TBIL to more than 3× ULN was moderate, and no increase in ALP was found. Patients with elevated liver enzymes classified as hepatocyte type at admission or during hospitalization had significantly higher odds of progressing to severe COVID-19. After admission, the use of drugs, especially lopinavir and ritonavir, was the most important risk factor for liver damage. The use of lopinavir/ ritonavir increased the odds of liver injury by 4-fold. Thus, it is suggested to closely monitor patients who used these particular therapies, especially in those who had abnormal liver test results at admission during hospitalization. Two recent studies showed that ACE2 was the key receptor for SARS-CoV-2 cell entry [6, 7], which was mainly localized in the heart, kidney, and testes, and expressed at a low level in many other tissues, especially in the colon and lung [8]. Another recent study showed that SARS-CoV-2 might directly bind to ACE2 positive cholangiocytes and cause liver damage [9], which may partially explain the contribution of SARSCoV- 2 infection to the liver test dysfunction.
Cardiac markers
It includes CPK-MB; TROP T; NT-PRO BNP; LDH; The exact pathway by which elevated biomarkers leads to death with COVID‐19 with systemic inflammatory activity may include myocarditis, thrombosis, and additionally unstable coronary atherosclerotic plaque rupture. Hence, beyond the predominant pulmonary complications, severity, and mortality sources include viral myocarditis, cytokine‐driven myocardial damage, microangiopathy, and acute coronary syndromes. Therefore, biomarkers may identify a heightened inflammatory response, including endothelial dysfunction and microvascular damage.
In the treatment of patients with COVID-19, the prevention and treatment of thrombus should be noted. It has been reported that reactive thrombocytosis occurred in 4% of patients, which may be related to the increased risk of thrombus [10]. In addition, considering that patients with COVID-19 might have increased blood viscosity due to high fever and excessive sweating, hypercoagulable state because of activation of coagulation system [11]. Together with the risk factors such as long-term bedridden, obesity and old age, the risk of thrombus is further increased. The diagnostic value of D-dimer levels for thrombus formation in COVID-19 patients is unclear. Whether higher D-dimer Levels in patients with COVID-19 suggest the need for more aggressive anticoagulant therapy deserves further discussion. Previous studies demonstrated high D-dimer levels in patients with CAP similar to patients with pulmonary embolism that decreased the reliability of the test for the differential diagnosis of CAP and pulmonary embolism [12]. As shown in our study, levels of D-dimer decreased with the disappearance of inflammation and the improvement of the disease, which indicates that it is not reasonable to judge whether anticoagulation is needed only according to D-dimer levels. Also, the low correlation between Padua VTE score and D-dimer levels weakened the role of D-dimer in the prediction of thrombosis. Interestingly, not all patients’’ D-dimer levels decreased with the decrease of inflammatory factors, suggesting the possibility of thrombosis. Thus, it should be noted that if levels of D-dimer are not synchronized with the regression of inflammation, anticoagulation therapy is needed. In addition, VTE risk assessment should also be considered in clinical decision-making. Because the mortality of COVID-19 increases with age, and elderly patients are more likely to have bleeding events, bleeding scores should also be included in clinical decisions.
Lactate dehydrogenase
Lactate dehydrogenase (LDH) is an enzyme implicated in the conversion of lactate to pyruvate in the cells of most body tissues and increased following tissue breakdown. Consequently, elevated serum LDH is present in numerous clinical conditions, such as haemolysis, cancer, severe infections and sepsis, liver diseases, hematologic malignancies, and many others. Nowadays, there was much evidence suggesting that the serum LDH levels serve as a non-specific indicator of cellular death in many diseases [13, 14]. The values of LDH give good predictivity of the disease severity in COVID-19 patients.
As multiple pulmonary CT scans and serial LDH determination provided reliable data. It was indicated that decrease or increase of LDH was indicative of corresponding radiographic improvement or progression [15].
Arterial blood gas analysis
The most predominant complication of COVID 19 is arterial hypoxemia thereby affecting lung compliance. Requiring mechanical ventilation due to which they are placed in a ventilator. Acid base imbalance is frequent association with patients suffering from serious viral illness and COVID being one such dreaded disease. To monitor acid base balance of patient arterial blood gas (ABG) is a routine investigation which is carried out.
ABG provides us information regarding patient’s oxygenation, ventilation adequacy and acid base levels. Patients of COVID 19 may develop acute respiratory distress, and CT chest is an effective tool to identify lung lesions in COVID19 pneumonia; however it cannot be repeatedly done to monitor those lung lesions as there is risk of radiological exposure.
In research by Shang et al., [16] it was confirmed that ABG values correlated with the presence and morphology of CT lesions and it can be done repeatedly for regular monitoring of critically ill patients (Table 2). Thus ABG is a rapid, cheaper and a widely used investigation and a valuable tool for preliminary prognostic assessment of patients with SARSCOV2 infection.
Table 2: Components of arterial blood gas.
|
Value
|
Arterial blood
|
|
pH
|
7.40 (7.35-7.45)
|
|
PaO2
|
80-100mm of Hg
|
|
O2 saturation
|
95%
|
|
PaCO2
|
35-45 mm of Hg
|
|
HCO3-
|
22-26mEq/L
|
|
BE
|
-2 TO +2
|
Ferritin
The mechanisms responsible for the association of hyperferritinemia and disease severity in patients with COVID-19 are unclear, but there are several possibilities for this phenomenon: (1) proinflammatory cytokines such as interleukin-I β (IL-l β), tumour necrosis factor-a (TNF-α), and IL-6 may increase ferritin synthesis [17]. Hence, we speculated that SARS-CoV-2-induced production of proinflammatory cytokines (i.e., IL-6, TNF-α), which are known to be elevated in COVID-19, might promote ferritin synthesis early in inflammation. (2) The cellular damage derived from inflammation can promote the leakage of intracellular ferritin, thus elevating serum ferritin [18]. (3) In acidosis, the micro vascular environment and increased production of reactive oxygen species (ROS) might liberate iron from ferritin, and it is this unliganded iron that can participate in Haber-Weiss and Fenton reactions, creating hydroxyl radicals, causing further cellular damage [18] and worsening tissue injury, thus causing a vicious cycle of inflammation.
Wu et al. investigated 201 confirmed cases of COVID-19 to study the clinical characteristics and outcomes in patients with COVID-19 pneumonia who developed acute respiratory distress syndrome (ARDS) or died; their findings showed that higher serum ferritin was an independent risk factor associated with ARDS development [19].
Procalcitonin
Procalcitonin (PCT) is a widely used biomarker to assess the risk of bacterial infection and disease progression. In patients with bacterial sepsis, suspected or confirmed lower respiratory tract infections, including community acquired pneumonia, acute bronchitis and acute exacerbations of COPD, PCT can be a useful decision-making tool for antibiotic therapy [20]. In addition, early evidence suggests that PCT may also be valuable tool in identifying COVID-19 patients who may be at risk for bacterial co-infection in all the types of infections from the lung such as bacterial pneumonia or other types of viral pneumonia; PCT helps to discriminate between milder cases and more severe cases.
PCT also helps to discriminate between severe bacterial pneumonia and mild viral pneumonia in all the types of infections from the lung such as bacterial pneumonia or other types of viral pneumonia, PCT helps to discriminate between milder cases and more severe cases. PCT also helps to discriminate between severe bacterial pneumonia and mild viral pneumonia. However, at a certain point, in the course of the disease, their PCT levels start to increase. This could be due to two reasons. One of them would be that the patient has acquired bacterial co-infection. This is common in patients with a viral infection because once the lung tissue gets damaged by the virus, it’s easier for normal bacterial flora to gain access and become invasive. This results in the development of secondary bacterial pneumonia in these patients, which is typically confirmed through blood cultures, sputum tests and radiological confirmation. If these tools show signs of bacterial pneumonia, it’s very important to start antibiotic treatment in these patients. If a patient has bacterial co-infection, his prognosis and mortality risk increases if early antibiotic treatment is not initiated. The other reason could be that a patient starts to deteriorate, his general condition becomes much worse, he goes into shock and develops an inflammatory syndrome – a COVID associated pneumonitis, which has a complex pathophysiology with endothelial dysfunction. During this severe inflammation and septic illness, there is also translocation of bacteria through the gut membranes and a very strong induction of different cytokines. This increases PCT production by bacterial translocation through the intestines but also directly because of the huge inflammatory boost and toxic syndrome that is developing in these patients. Overall, if a patient has milder COVID-19 infection, they generally are expected to have low PCT levels. This also confirms that it is not a bacterial infection but a viral infection. However, if, during the course of the disease, the patient gets worse, and his PCT levels increase, it must be taken seriously. This does not necessarily mean that there is bacterial co-infection. That could be a possibility, but it could also mean that the patient is going into severe inflammatory pneumonitis syndrome.
Renal markers
Serum urea, creatinine and cystatin C concentrations in severe COVID-19 patients were significantly higher than those in mild COVID-19 patients. In particular, serum biomarkers, including urea, Crea, CysC, which reflect glomerular filtration function, have some significance as potential indicators for the early diagnosis of severe COVID-19 and to distinguish it from mild COVID-19, suggesting that SARS-CoV-2 infection could damage the kidney Glomerular filtration function injury in severe COVID-19 patients should also be considered by clinicians [21].
Conclusion
This article is based on various studies done on all biochemical parameters. As of now, IL-6 is a good marker, superior to CRP, ferritin, liver enzymes to predict respiratory failure at cut off levels >80pg/ml. The other parameters like d-dimer, C-reactive protein, ferritin, lactate dehydrogenase, procalcitonin are also correlated positively with COVID-19 severity. Day by day symptomatology, severity of the disease by the virus are being changed, so extensive studies are further required to guide the clinician to treat the COVID-19 before getting complicated, reducing mortality and shortening the hospitalization period.
Conflicts of interest
Authors declare no conflicts of interest.
References
[1] World Health Organization (WHO). Corona virus disease (COVID-19) Technical Guidance: Infection Prevention and Control. Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/technical-guidance/infection-prevention-and-control
[2] Lin L, Li TS. Interpretation of “Guidelines for the diagnosis and treatment of novel coronavirus (2019-nCoV) infection by the National Health Commission (Trial Version 5)”. Zhonghua Yi Xue Za Zhi. 2020; 100:E001.
[3] Siddiqi, HK, Mehra, MR. COVID-19 illness in native and immune suppressed states: a clinical- therapeutic staging proposal. J Heart lung Transplant. 2020; 39(5):405–407.
[4] Chen X, Zhao B, Qu Y, Chen Y, Xiong J, et al. Detectable serum SARSCoV-2 viral load (RNAaemia) is closely associated with drastically elevated interleukin 6 (IL-6) level in critically ill COVID-19 patients. BioRxiv. 2020; Available from: http://dx.doi.org/10.1101/2020.02.29.20029520
[5] Wang H, Luo S, Shen Y, Li M, Zhang Z, et al. Multiple enzyme release, inflammation storm and hypercoagulability are prominent indicators for disease progression in COVID-19: a multi-centered, correlation study with CT imaging score. SSRN 2020; Available from: http://dx.doi.org/10.2139/ssrn.3544837.
[6] Hoffmann M, Kleine-Weber H, Schroeder S, Krüger N, Herrler T, et al. SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell. 2020; 181(2):271–280.e8.
[7] Yan R, Zhang Y, Li Y, Xia L, Guo Y, et al. Structural basis for the recognition of SARS-CoV-2 by full-length human ACE2. Science. 2020; 367(6485):1444–1448.
[8] Clarke NE, Turner AJ. Angiotensin-converting enzyme 2: the first decade. Int J Hypertens. 2012; 2012:307315.
[9] Chai X, Hu L, Zhang Y, Han W, Lu Z, et al. Specific ACE2 expression in cholangiocytes may cause liver damage after 2019-nCoV infection. Bio-Rxiv. 2020; Available from: https://doi.org/10.1101/2020.02.03.931766.
[10] Guan W, Ni Z, Hu Y, Liang WH, Ou CQ, et al. Clinical characteristics of 2019 novel corona virus infection in China. MedRxiv. 2020; Available from: https://www.medrxiv.org/content/10.1101/2020.02.06.20020974v1
[11] Tang N, Li D, Wang X, Sun Z. Abnormal coagulation parameters are associated with poor prognosis in patients with novel corona virus pneumonia. J Thromb Haemost. 2020; 18(4):844–847.
[12] Snijders D, Schoorl M, School M, Bartels PC, Vander Werf TS, et al. D-dimer levels in assessing severity and clinical outcome in patients with community-acquired pneumonia. A secondary analysis of a randomised clinical trial. Eur J Intern Med. 2012; 23(5):436–441.
[13] Kolev Y, Uetake H, Takagi Y, Sugihara K. Lactate dehydrogenase-5 (LDH-5) expression in human gastric cancer: association with hypoxia-inducible factor (HIF-1alpha) pathway, angiogenic factors production and poor prognosis. Ann Surg Oncol. 2008; 15(8):2336–2344.
[14] Uchide N, Ohyama K, Bessho T, Toyoda H. Lactate dehydrogenase leakage as a marker for apoptotic cell degradation induced by influenza virus infection in human fetal membrane cells. Intervirology. 2009; 52(3):164–173.
[15] Wu MY, Yao L, Wang Y, Zhu XY, Wang XF, et al. Clinical evaluation of potential usefulness of serum lactate dehydrogenase (LDH) in 2019 novel corona virus (COVID-19) Pnueumonia. Respir Res. 2020; 21(1):171.
[16] Shang Y, Xu C, Jiang F, Huang R, Li Y, et al. Clinical characteristics and changes of chest CT features in 307 patients with common COVID-19 pneumonia infected SARS-CoV-2: A multicenter study in Jiangsu, China. Int J Infect Dis. 2020; 96:157–162.
[17] Kell DB, Pretorius E. Serum ferritin is an important inflammatory disease marker, as it is mainly a leakage product from damaged cells. Metallomics. 2014; 6(4):748–773.
[18] Kobune M, Kohgo Y, Kato J, Miyazaki E, Niitsu Y. Interleukin-6 enhances hepatic transferrin uptake and ferritin expression in rats. Hepatology 1994; 19(6):1468–1475.
[19] Wu C, Chen X, Cai Y, Xia J, Zhou X, et al. Risk Factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern Med. 2020; 180(7):934–943.
[20] Phillip Scheutz. Role of procalcitonin for risk assessment and treatment of COVID –patients. Health Management, 2020; 20(5). ISSN=1377-7629. Available from: https://healthmanagement.org/c/healthmanagement/issuearticle/the-role-of-procalcitonin-for-risk-assessment-and-treatment-of-covid-19-patients
[21] Xiang J, Wen J, Yuan X, Xiong S, Zhou X, et al. Potential biochemical markers to identify severe cases among COVID-19 patients. MedRxiv. Available from: https://www.medrxiv.org/content/10.1101/2020.03.19.20034447v1