Original Research
2015
June
Volume : 3
Issue : 2
Study of bone markers in hyperthyroidism: Single centre experience from south India
Babulreddy Hanmayyagari, Mounika Guntaka, Rakesh Sahay, Ramesh Jayanthy, Nagesh Sri
Pdf Page Numbers :- 53-56
Babulreddy Hanmayyagari1,*, Mounika Guntaka2, Rakesh Sahay3, Ramesh Jayanthy3 and Nagesh Sri4
1Department of Endocrinology, Krishna Institute of Medical Sciences, Kondapur, Hyderabad -500084, India
2Department of Biochemistry, Chalmeda Anand Rao Institute of Medical Sciences, Bommakal, Karimnagar, Telangana 505001, India
3Department of Endocrinology, Osmania general hospital, Hyderabad-500012, India
4Department of Endocrinology, Care Hospital, Banjara hills, Hyderabad, India
*Corresponding author: Dr. H. Babul Reddy, Department of Endocrinology, Krishna Institute of Medical Sciences, Kondapur, Hyderabad - 500084, India. Mobile: +91 9985661434; Email: babulreddy78@gmail.com
Received 20 January 2015; Revised 10 March 2015; Accepted 17 March 2015; Published 24 March 2015
Citation: Babulreddy H, Mounika G, Rakesh S, Ramesh J, Nagesh S. Study of bone markers in hyperthyroidism: Single centre experience from south India. J Med Sci Res. 2015; 3(2):53-56. DOI: http://dx.doi.org/10.17727/JMSR.2015/3-010
Copyright: © 2015 Babulreddy H, et al. Published by KIMS Foundation and Research Center. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Aim: To evaluate bone health markers and vitamin D status in patients with hyperthyroidism comprehensively, and comparison of same with matched controls.
Materials and methods: The study has been done on 30 newly diagnosed hyperthyroid patients and matched controls. Cases were selected after careful exclusion of conditions which adversely affect bone health. Statistical comparisons were performed with Student’s t test.
Results: The study group has shown normal calcium (20% had hypocalcemia), normal phosphorus, normal PTH values, raised alkaline phosphatase levels & significant rise in both bone formation (Osteocalcin) and resorption (β-cross laps) markers (P<0.05). In addition 95% of our subjects (patients and controls) were vitamin D deficient (mean-17.2 ng/dl). There is no specific increase in vitamin D deficiency in hyperthyroidism patients.
Conclusion: Hyperthyroidism is associated with increased rate of bone remodeling & changes in mineral homeostasis, thereby increases risk of fractures. Associated vitamin D deficiency further deteriorates bone quality. So it is suggested therapeutic vitamin D and calcium supplementation in addition to antithyroid medication.
Keywords: hyperthyroidism; vitamin D; osteocalcin; β-crosslaps
Full Text
Hyperthyroidism is a common endocrine disorder associated with significant impact on bone health. Predominant effects seen are, increased rate of bone remodeling, thereby changes in mineral homeostasis ultimately leading to a reduction in bone mineral density (BMD). These changes are in turn associated with osteoporosis, and have increased risk for fracture [1].
But changes in BMD occur only slowly, making it difficult to judge the benefits, if any, of antithyroid medication. Early identification of the individuals at risk of long-term reduction in BMD caused by thyrotoxicosis, may enable early therapeutic intervention. A number of biochemical markers reflect the rapid bone turnover in thyrotoxicosis, early in the disease course, and their role in prediction of BMD are established recently [2].
There is a scarcity of data on bone markers in thyrotoxicosis from India. Western data suggest that these patients have hypercalcemia, hyperphosphatemia, raised alkaline phosphatase and suppressed parathyroid hormone (PTH). Available small data from northern India suggests that due to concomitant vitamin D deficiency in these patients have normal calcium levels and increased bone loss, but the authors have not performed bone markers in their study. Recently a study showed high prevalence of vitamin D deficiency in south Indian population [3]. So this topic is chosen to study vitamin D status, bone health markers & effect of vitamin D deficiency on bone health, in thyrotoxic patients.
Materials & methods
The study has been done on a group of hyperthyroidism patients and matched controls, attending to our centre, over a period of 6 months. Both inpatients and outpatients were included. A total of 100 cases of hyperthyroid patients were screened and 30 cases were selected for the study (5 male patients were screened but excluded because all of them were smokers). Control group consisting of 20 subjects were included who were matched by the hyperthyroid group as far as possible. Total calcium and vitamin D intake/day was calculated in all subjects by a dietary recall method with the help of a dietician.
Inclusion criteria
Subjects of 18-45 years, who is having fairly regular cycles with symptoms and signs of thyrotoxicosis for at least 3 months and who were not using antithyroid medication in the past.
Exclusion criteria
Parity > 3children, postmenopausal, amenorrhea > 6months (including pregnancy and lactation), smokers, drugs which interfere with bone turnover. History of malabsorption (pancreatitis, bowel surgery), and Beta blockers, diuretics, OC pills, calcium supplements, etc., because all these factors can interfere adversely with bone turnover.
Statistical analysis
Parameters are expressed as mean ± 1 SEM, statistical comparisons were performed with Student’s t test. Calculations were performed using SPSS software (version 10.0), a P value ≤ 0.05 was considered statistically significant.
Biochemical measurements
Serum samples were collected from all patients before 9 am after an overnight fast. The samples were immediately processed and kept frozen at -70°C until the assays were performed. Serum calcium and serum phosphatase were determined by spectrophotometric analysis, alkaline phosphatase measured by PNPP kinetic method. Serum 25-OHD was measured by radioimmunoassay, and intact PTH was determined by chemiluminescence assay (cold chain maintained from syringe to storage).
Osteocalcin measured by the highly specific immunoenzymometric assay (kits provided by biosource Europe S. A Rue de l’Industrie, 8, B-100 Nivelles, Belgium). β-crosslaps were measured by electro-chemiluminescensce.
Results and analysis
In this study all our patients had newly diagnosed hyperthyroidism, presumably of several months of duration and are associated with observable changes in bone mineral metabolism and bone markers. The baseline characters of the patients and controls and their data on bone minerals, markers are depicted in below tables (Tables 1 & 2).
Table 1: Baseline clinical & biochemical parameters.
|
Character
|
Patients(30) (mean±1SEM)
|
Controls(20) (mean±1SEM)
|
P value
|
|
Age (Yrs)
|
28.4±2.3
|
28.9±2.8
|
0.75
|
|
Symptoms before presentation (wks)
|
14±2
|
_
|
|
|
Etiology
|
|
Graves
|
29
|
_
|
|
|
Toxic adenoma
|
1
|
_
|
|
|
P.R
|
102±8
|
77.2±6
|
0
|
|
S.B.P (mm of Hg)
|
100±6
|
100±8
|
0.552
|
|
D.B.P(mm of Hg)
|
57.6±8
|
74±4
|
0.03
|
|
Blood biochemistry
|
|
RBS(mg/dl)
|
101±6.7
|
94.8±8.3
|
0.252
|
|
B.UREA(mg/dl)
|
27.6±1.7
|
29.8±2.1
|
0.114
|
|
S.creatinine(mg/dl)
|
0.863±0.56
|
0.820±0.7
|
0.384
|
|
T3(ng/dl)
|
488±68
|
121±80
|
0
|
|
T4(µg/ml)
|
21.8±1.5
|
8.04±1.9
|
0
|
|
TSH(µIU/ml)
|
0.05±0.02
|
2.3±0.3
|
0
|
Table 2: Bone minerals, markers in cases and controls.
|
Parameter
|
Cases(mean±1SEM)
|
Controls(mean±1SEM)
|
P value
|
|
Corrected calcium (mg/dl)
|
8.73±0.3
|
8.98±0.35
|
0.303
|
|
Phosphorus (mg/dl)
|
3.84±0.4
|
3.71±0.5
|
0.683
|
|
Alkalinephosphatase(u/l)
|
329±44.6
|
314±54
|
0.679
|
|
25(OH) vitD3 (ng/dl)
|
17.2±2.6
|
18.1±3.2
|
0.673
|
|
PTH (pg/ml)
|
23±4.45
|
18.3±5.5
|
0.191
|
|
Osteocalcin (ng/dl)
|
5.89±1.8
|
1.79±0.7
|
0.006
|
|
β – crosslaps(ng/dl)
|
0.453±0.8
|
0.215±0.1
|
0
|
Discussion
The majority of patients with hyperthyroidism in the west, has normal or increased serum total calcium levels, hyper phosphatemia and suppressed PTH levels than controls [4]. All of the above effects are due to increased bone resorption in thyrotoxicosis due to the direct effect of T3 on bone [5]. Our patients with thyrotoxicosis are different from the western patients from the bone mineral homeostasis point of view. These patients have normal calcium (in fact 20% had hypocalcemia), normal phosphate & PTH levels. This is due to the presence of associated subclinical vitamin D deficiency in our group, and recent data confirmed that there is widespread vitamin D deficiency in south Indian population [3]. This can further deteriorate bone quality in this population. These bone mineral parameters were well correlated with available Indian data [6].
Hyperthyroidism is characterized by increased bone turnover and bone resorptive activity [7]. It is observed in this study where both bone formation & resorption parameters were elevated (Figure 1 and 2). In the hyperthyroid status the initiation rate of new remodeling cycles is significantly increased. However, the total work performed by resorptive cells (i.e. the final resorption depth) is unchanged, whereas the total work performed by osteoblasts (i.e. mean thickness of completed walls) is reduced. The normal cycle duration of approximately 200 days is halved in thyrotoxicosis. Thus, during the thyrotoxic status resorption markers increase much more than formation markers (the same was observed in this study). This reflects unbalanced bone turnover in favour of bone resorption and is probably due to some degree of direct inhibition of osteoblasts by high thyroid hormone levels. Reversal above pattern seen with treatment of hyperthyroidism [8] (increase in formation markers than resorption markers).
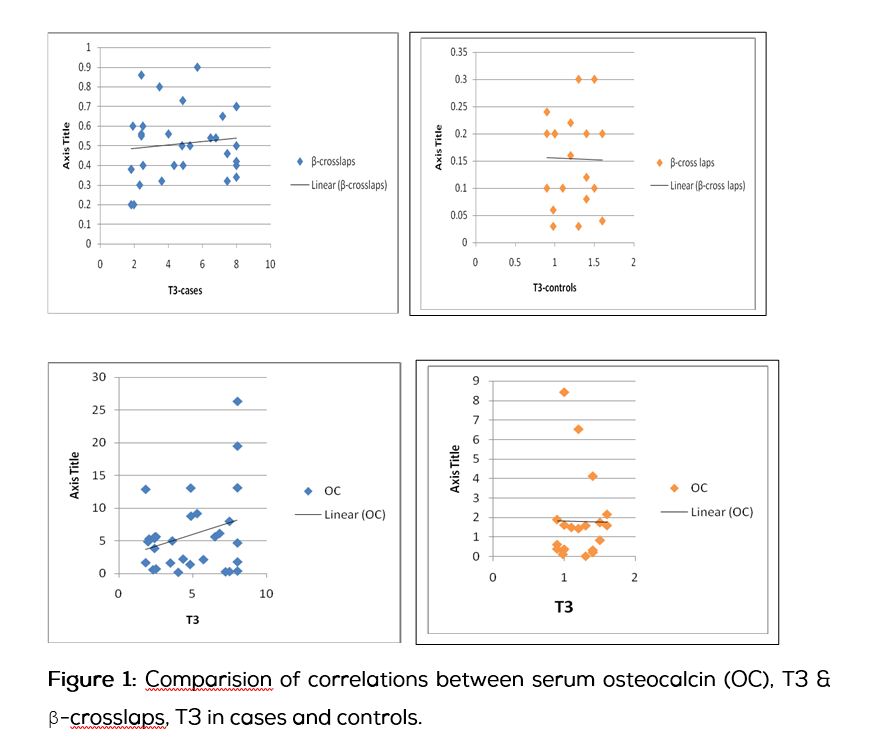
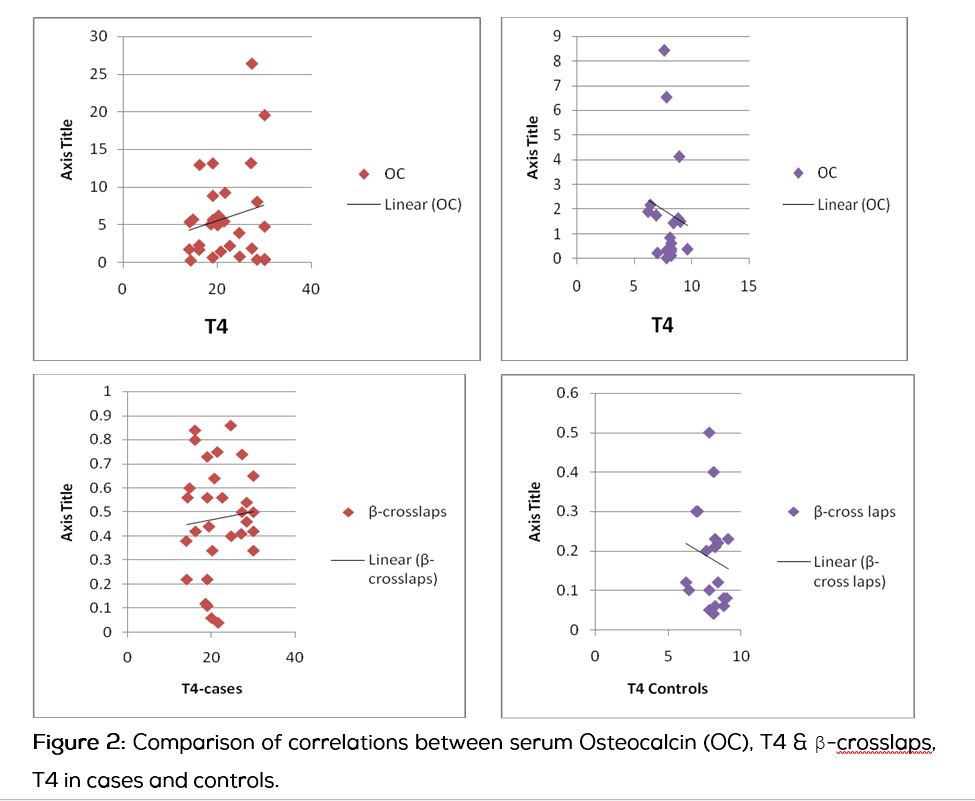
Conclusions
Hyperthyroidism is associated with increased rate of bone remodeling & changes in mineral homeostasis, thereby increase the risk of fracture. Associated vitamin D deficiency in hyperthyroid patient’’s further increase bone turnover, thereby adversely affecting bone quality. Therefore, therapeutic doses of vitamin D and calcium supplementation to correct vitamin D deficiency and continuous calcium supplementation in addition to antithyroid medication will improve bone quality in hyperthyroid patients and further larger studies are needed on this issue.
Limitations of the study
Sample size is small, so large scale studies are needed to confirm these findings. The status of bone mineral metabolism and bone markers were not studied after euthyroidism is achieved. As all of our patients (cases & controls) are vitamin D deficient, bone health markers in vitamin D sufficient group need to be done.
Conflict of Interest
The authors declare no conflict of interest.
References
1. Fraser SA, Smith DA, Anderson JB, Wilson GM. Osteoporosis and fractures following thyrotoxicosis. Lancet. 1975; 1(7707):981–983.
2. Hari Kumar KV, Muthukrishnan J, Verma A, Modi KD. Correlation between bonemarkers and BMD in post-menopausal women with osteoporosis. Endocr Pract. 2008; 14(9):1102–1107.
3. Harinarayan CV, Ramalakshmi T, Prasad UV, Sudhakar D, Srinivasarao PV, et al. High prevalence of low dietary calcium,high phytate consumption and vit D deficiency in healthy south Indians. Am J Clin Nutr. 2007; 85(4):1062–1067.
4. Mosekilde L, Eriksen EF, Charles P. Effects of thyroid hormones on bone and mineral metabolism. Endocrinol Metab Clin North Am. 1990; 19(1):35–63.
5. Manicourt D, Demeester-Mirkine N, Brauman H, Corvilain J. Disturbed mineral metabolism in hyperthyroidism good correlation with tri-iodothyronine. Clin Endocrinol (Oxf). 1979; 10(4):407–412.
6. Dinesh K. Dhanwal: Bone mineral metabolism in thyrotoxicosis. IJEM. 2007; 11(1&2):33–36.
7. Siddiqi A, Burrin JM, Noonan K, James I, Wood DF, et al. A longitudinal study of markers of bone turnover in Graves’ disease and their value in predicting bone mineral density. J Clin Endocrinol Metab. 1997; 82(3):753–759.
8. Garnero P, Vassy V, Bertholin A, Riou JP, Delmas PD. Markers of bone turnover in hyperthyroidism and the effects of treatment. J Clin Endocrinol Metab. 1994; 78(4):955–959.