Full Text
Introduction
This communication is intended to give an overview of management of supra ventricular tachycardia (SVT). This is the commonest arrhythmia seen in the causality or Emergency room. Patients perceive this problem as palpitations or unpleasant awareness of one’s own heart beat. Generally this is seen in the age group of 20 -40 years more often in females. The occurrence of symptoms is episodic (hence referred as PSVT, p- paroxysmal) and frequency can vary from 1- 2 times year to 2-3 times a week. It can occur any time of the day or night. Palpitations can be sometimes so rapid that they can result in dizziness or loss of consciousness. Some of the patients I have seen have been suffering from this problem for over 20 years.
The diagnosis is made by ECG. Typically the ECG shows regular tachycardia of rates 160-180/minute with narrow QRS complexes. P waves may or may not be seen. Patient is conscious though anxious and worried. Blood pressure is usually normal sometimes transiently may be lower but on lying down generally improves. Echocardiogram is usually normal as this condition affects people with normal hearts.
Mechanisms of SVT
There are typically 3 mechanisms of SVT- Atrioventricular Nodal Reentry Tachycardia (AVNRT), Atrioventricular Reciprocating Tachycardia (AVRT), and less commonly atrial tachycardia. By ECG alone many times these 3 may be indistinguishable from each other. The important thing is the initial treatment of SVT is same irrespective of the mechanism. In this letter I have dealt only with AVNRT and AVRT.
AVNRT: This is by far the most common mechanism underlying SVT. Basically patients with this arrhythmia have 2 pathways in the AV node- The fast and slow pathways. Normal individuals have only one pathway-the fast. When 2 pathways are present, under favorable electrophysiological conditions cardiac impulses travel down the slow pathway and up the fast pathway leading to a re-entry tachycardia which clinically manifests as SVT.
AVRT: Similar to AVNRT, patients have 2 pathways – a normal AV node and an accessory pathway. The difference is the extra or accessory pathway is outside the AV node and connects atria and ventricles. The tachycardia is set up when an impulse travels down the AV node and up the accessory pathway. Some of these patients have a sinus rhythm ECG which has a short PR interval and a delta wave. This is termed as manifest pre excitation. Patients with manifest pre excitation who have SVT are referred as Wolff–Parkinson–White (WPW) syndrome. Presentation of AVRT is similar to AVNRT but the tachycardia may be faster and involves younger individuals.
ECG Recognition: Both AVNRT and AVRT typically present with ECG showing a narrow QRS (qrs duration< 120 msec), sort RP tachycardia (The interval between R of qrs and retrograde P is less than the interval between the retrograde P and R of next QRS.)The retrograde P wave gives the impression of ST depression. Hence mistaken for unstable angina. Many patients with SVT thus unnecessarily undergo coronary angiogram. ECG taken during sinus rhythm is also important as it may show presence of pre excitation (short PR interval and a delta wave). If this is present indicates the diagnosis of AVRT and WPW syndrome.

Figure 1: Typical SVT-Narrow QRS short RP regular Tachycardia. Arrows point to retrograde p waves

Figure 2: Manifest pre-excitation in a patient with WPW syndrome. Arrows point to delta waves
Initial treatment
Stable SVT
The first step is to assess the hemodynamic stability of the patient. If the blood pressure is stable and patient is conscious the following initial treatment can be given.
A. Vagal maneuvers: Carotid massage is the first step that can be tried as IV access is being secured. One needs to massage internal carotid artery one side at a time after making sure there is no bruit in the carotid artery. This is another vagal maneuver that can also be taught to the patient to practice outside hospital settings. Ask the patient to breathe in deeply then close mouth and nose and then “ breathe out through the ears. This is known as the Valsalva maneuver. These maneuvers increase the vagal tone and cause decreased conduction through the AV node and cause tachycardia termination.
B. Medications: All patients who present with SVT should be connected to a monitor and intravenous (IV) access should be secured. The access should be preferably at the elbow. Any of the following medications can be tried. All the drugs act by interfering with the tachycardia circuit by causing decreased conduction at the AV node.
1. Adenosine: This is a very effective drug. It has a very short half life as its action starts the moment it touches the blood. Hence one should avoid aspirating blood into the syringe while this drug is being administered to prevent the blood from coming into contact with adenosine. The usual dosage in adults is 12 mg given as a IV push followed by flushing 10 -20 cc of saline rapidly. One should look out for transient flat line as it terminates the tachycardia by causing AV block, but as the half life is only a few seconds the rhythm returns. It can also cause transient atrial fibrillation and few ventricular etopics.
2. Beta blockers: IV Metaprolol 5- 10 mg can be administered in patients who do not have contra indications to beta blockers.
3. Calcium channel blockers: Verapamil or Diltiazem are the agents that can be used to terminate SVT. Diltiazem is usually given 5-15 mg; sometimes even 20 mg is required.
SVT with hypotension
Sometimes SVT could be associated with hypotension; generally this is transient and improves when patient is made to lie supine. Patient may continue to be hypotensive. This particularly happens in WPW syndrome when Atrial fibrillation develops. Normally AV node acts as a protective structure limiting the ventricular rates in atrial fibrillation, in WPW syndrome due to presence of an accessory pathway or a bypass tract this protection of AV node is lost, hence patient presents with wide QRS irregular tachycardia.( compare with VT which is wide QRS regular tachycardia). This situation is potentially dangerous as atrial fibrillation can lead to ventricular fibrillation and sudden death. Whatever the situation may be, if tachycardia is associated with hypotension, synchronized cardioversion is needed.
Long Term Treatment
Patients with SVT have periodic recurrent episodes, which need to be prevented.
- General conditions like anemia, diabetes, hypertension and importantly presence of hypothyroidism must be investigated and treated.
- Long term medications to prevent recurrences are indicated. The medications that are useful are Diltiazem, Verapamil and Metaprolol. All these medications act by suppressing conduction over AV node. These are useful in WPW syndrome who experience narrow QRS tachycardia though they may increase manifest pre excitation. Amiodarone is almost never indicated in AVNRT or AVRT. Propafenone or Amiodarone can be used in patients with WPW syndrome who have atrial fibrillation. However in these patients it is advisable to treat them by radiofrequency ablation.
- Radiofrequency ablation: Medications prescribed for SVT are only suppressive and never curative. Though the SVT episodes are episodic, patient needs to take medications daily throughout his/her life. Radiofrequency ablation in the last few years has evolved as a curative therapy for many of the arrhythmias. The treatment is non surgical. It is done in the cath lab under local anesthesia by an electrophysiologist. The first step is the Electrophysiological study to understand the source of the rapid heartbeat. It involves placing of special catheters which have electrodes in different areas in the heart by veins in the groin and neck. These catheters are connected to a computerized recording system by which the origin of the abnormal or accessory pathway can be found out. Once this is located, heat energy by radiofrequency current is delivered to the area with the catheter placed in the heart. This destroys the abnormal tissue immediately and the arrhythmia is permanently cured. The procedure time is typically about an hour and the success rates with this treatment for supraventricular tachycardia is about 98%- 99% with chances of occurring again of 1-2%. The most advantageous part is that the patient does not need to take any medications and live without the thought that he has any heart disease. The complication rates are < 1% and risk of AV block is 0.1%. Patient is generally ambulated 6-8 hours after the procedure and does not need long term follow up. Overall this is a very cost effective procedure.
When is Radiofrequency ablation Indicated?
1. Patients who experience recurrent SVT episodes despite using drugs like beta blockers/ calcium channel blockers.
2. Patients who find SVT episodes seriously interfering with their profession like teacher experiencing while teaching.
3. Those who have SVT associated with syncope or presyncope, which means that they are having hypotension during the episode.
4. WPW syndrome with atrial fibrillation as this can lead to ventricular fibrillation and sudden death
5. Patients intolerant to beta blockers/calcium channel blockers as they may develop bradycardia.
6. Some patients may choose to have ablation even when they have experienced and episode as they can avoid life -long medications and do not want the uncertainty of another episode.
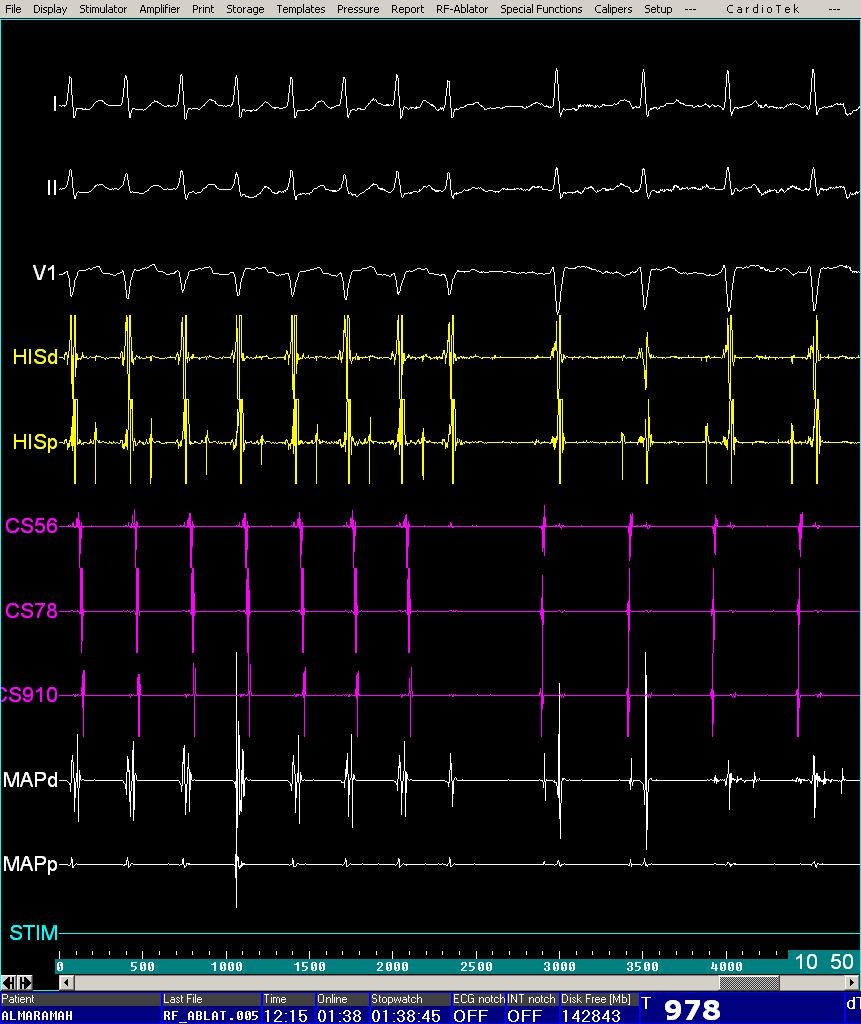
Figure 3: Termination of SVT during radiofrequency Ablation
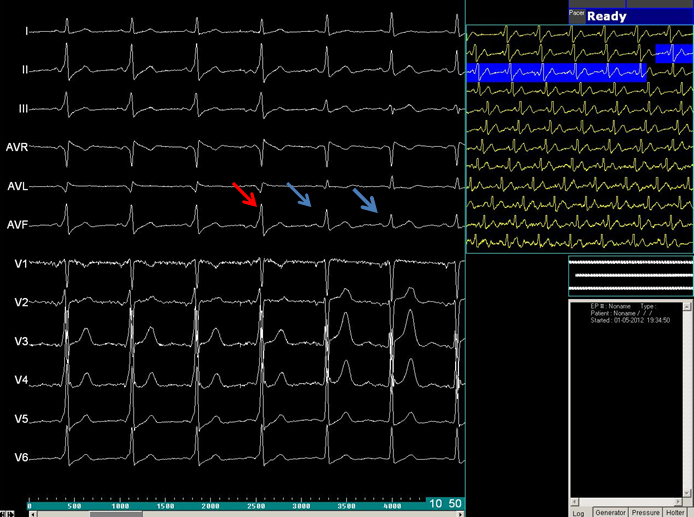
Figure 4: Radiofrequency Ablation in a patient with WPW syndrome. The first 4 beats show short PR interval with delta wave (Pre excitation). This is abolished from the 5th beat onwards as the energy is delivered.