Case Report
2016
December
Volume : 4
Issue : 4
Vanishing lung syndrome vs emphysematous bulla: 2 interesting cases
Vijay S, Sarma L, Deshpande P, Mohit C, Chaithanya I
Pdf Page Numbers :- 174-176
1Department of Pulmonology, Krishna Institute of Medical Sciences, Minister Road, Secunderabad-500003, Telangana, India
2Department of Radiology, Krishna Institute of Medical Sciences, Minister Road, Secunderabad-500003, Telangana, India
*Corresponding author: Dr. Vijay S, Department of Pulmonology, Krishna Institute of Medical Sciences, Minister Road, Secunderabad-500003, Telangana, India. Email: vijayusmle27@gmail.com
Received 05 August 2016; Revised 06 September 2016; Accepted 16 September 2016; Published 29 September 2016
Citation: Vijay S, Sarma L, Deshpande P, Mohit C, Chaithanya I. Vanishing lung syndrome vs emphysematous bulla: 2 interesting cases. J Med Sci Res. 2016; 4(4):174-176. DOI: http://dx.doi.org/10.17727/JMSR.2016/4-038
Copyright: © 2016 Vijay S, et al. Published by KIMS Foundation and Research Center. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Vanishing lung syndrome (VLS) is a rare radiological syndrome in which the lungs seem to disappear on chest radiograph. It is a chronic, progressive disorder usually affecting young male smokers and is characterised by giant emphysematous bullae, which commonly develop in the upper lobes. A rare case of a 28-year-old female patient who had no history of smoking, presented with chronic cough, expectoration and weight loss, is described. Radiograph and CT chest revealed findings suggestive of giant bullous disease/vanishing lung syndrome. Bronchoscopy showed copious purulent secretions. In view of recurrent infections and weight loss, the patient referred to surgeon for possible bullectomy, after controlling the infection. Another patient was a middle aged lady who presented with breathlessness was found to have severe pulmonary arterial hypertension (PAH). CT evaluation revealed large emphysematous bulla in right lower lobe along with chronic pulmonary thromboembolism (PTE).
Keywords: Vanishing lung syndrome; giant emphysematous bullae; bullectomy; young female
Full Text
Introduction
Vanishing lung syndrome (VLS) also known as idiopathic giant bullous emphysema is a disorder where the alveolar spaces gradually disintegrate, create large air spaces to form large bullae with eventual compression and atrophy of lung and progression to respiratory failure. It is an uncommon syndrome that differs from common forms of bullous emphysema by affecting younger population, most commonly young male smokers [1, 2]. The basic pathogenesis is not exactly known. However, it has been attributed to possible respiratory myositis. There is evidence of diaphragmatic weakness, and the disorder is associated with systemic lupus erythematosus in one-third of cases. Lung function tests show a restrictive pattern. High resolution computed tomography (HRCT) reveals bullae occupying more than one-third of the affected hemithorax (vary in size 1 - 20 cm) with upper lobe preponderance; there can be bilateral and asymmetric lung involvement and the presence of varying degrees of centrilobular and paraseptal emphysema. There may be compression effect on adjacent structures (lung atelectasis, inversion of the ipsilateral diaphragm or contralateral displacement of the mediastinum and displacement of junction lines [3]. HRCT also allows assessment of coexisting conditions such as infected cysts, bronchiectasis, pulmonary artery enlargement and pneumothorax. The disorder tends to be progressive. Criteria for bullectomy include large bullae with significant symptoms (reduced lung function or infection) [3] .
VLS is different from bullous emphysema in that it has bullae with structurally normal intervening lung, whereas emphysema has bullae associated with more diffusely abnormal lung parenchyma because of chronic obstructive pulmonary disease (COPD). VLS is said to be present if the bullae occupy at least one-third of the hemithorax and compress the surrounding lung parenchyma [4]. Bullectomy, either via video thoracoscopy or conventional thoracotomy, is the treatment of choice for giant bullous lung disease. Bullectomy is indicated for symptomatic patients who have incapacitating dyspnea or chest pain, and who have complications related to a bullous disease such as infection or pneumothorax [4]. Bullectomy needs to be differentiated from lung-volume reduction surgery (LVRS), which is surgical removal of 20-30% of nonbullous emphysematous lung from each side. Rarely,auto bullectomy may occur. Inflammation, tumour, mucous plug or blood clot may obstruct an already compromised bronchial communication with the bulla resulting in a closed space. Gradually, air reabsorbs leading to shrinkage and spontaneous regression of the giant bulla. Bullous emphysema is the presence of bullae in a patient with the chronic obstructive pulmonary disease and is characterised by the presence of centrilobular emphysema in the non-bullous lung.
Case summary
A 28-year-old female came with complaints of cough, purulent sputum, exertional shortness of breath since one year, with increasing severity since three months. There was history of fever since two days. She had used antibiotics on three occasions in last one year. The patient had a history of weight loss of about 2-3 kg. There was no history of hypertension, diabetes or any other co-morbidity. She is married and has two children.
On examination she is thin built with a heart rate of 110/min, blood pressure was 110/70 mm/Hg. Oxygen saturation was 98% on air.On auscultation,there was reduced air entry in inframammary,infraclavicular and axillary areas.
Chest plain radiograph revealed hyperlucency in left hemithorax with evidence of collapsed lung. CT chest showed large emphysematous area occupying the entire left upper lobe with very minimal lung towards the periphery. The presence of clinical and radiological features and restrictive pattern on pulmonary function testing favours the diagnosis of ‘vanishing lung syndrome' in our patient. Bronchoscopy showed copious purulent secretions in the trachea, left main and segmental bronchi. Acid fast bacilli were negative; culture showed no growth of pathogens (patient received two courses of antibiotics before sample collection). In view of recurrent infections, weight loss, the patient was referred to surgeon for possible bullectomy, after controlling infection.
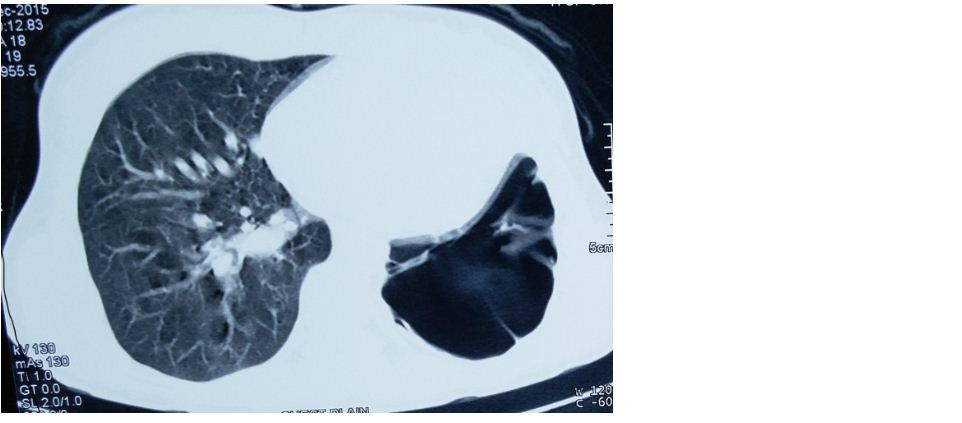
Figure 1: CT chest showed large emphysematous area occupying the entire left upper lobe area with very minimal lung shadow towards the periphery. Note: The enlareged right lobar plumonary artery.
Case 2
A 50-years-old female presented with shortness of breath of 20 years duration. She was extensively evaluated and CT pulmonary angio revealed severe pulmonary arterial hypertension (PAH) and chronic pulmonary thromboembolism (PTE) .There is a eccentric chronic partial thrombus in the right main pulmonary artery extending into upper lobar, middle lobar and lower lobar arteries. The thrombus is causing complete occlusion of middle lobe arteries. There was a large emphysematous bulla in right lower lobe. She was advised oral anticoagulants, bronchodilators.
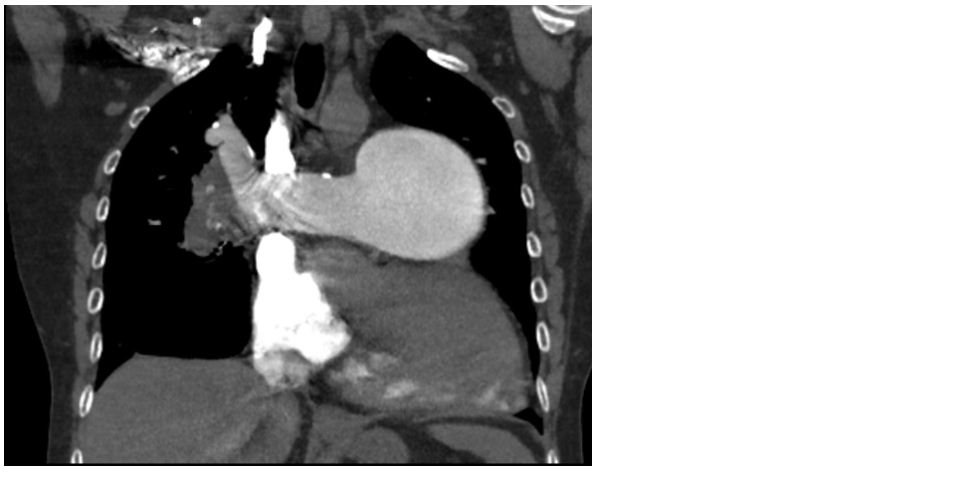
Figure 2: CT showed large emphysematous bulla in the lower lobe of right lung.
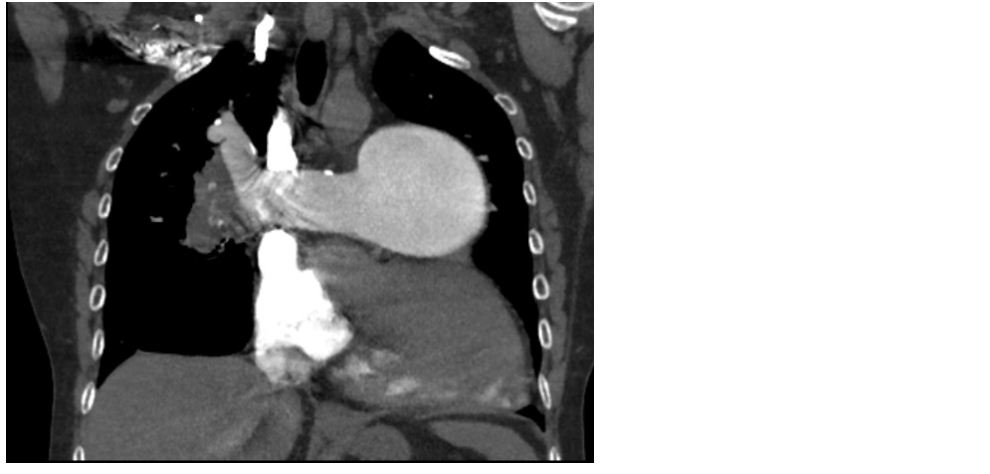
Figure 3: CT pulmonary angio revealed severe pulmonary arterial hypertension (PAH) and chronic pulmonary thromboembolism (PTE).
Discussion
HRCT is considered the best imaging modality to identify centrilobular emphysema. The formation of these intrathoracic spaces, under the influence of lung elastic recoil, causes healthy parenchyma to collapse rearranging itself to a lower expansion state. This structural change is speculated to play a role in determining the size and progression of bullae. The large size of bullae and its predominantly apical location makes it hard to differentiate from a pneumothorax on chest radiograph. The inability to see the entire lung pleural line separated from the chest wall on a chest radiograph makes pneumothorax less likely and warrants further imaging [5].
Very few case reports of female non-smokers diagnosed with vanishing lung syndrome include 31-years-old non-smoker female diagnosed with VLS [6] and another 56-year-old chinese female diagnosed with VLS published in IJCEM 2015.
Conclusion
Advanced bilateral upper lobe bullous emphysema affecting young male smokers should raise the suspicion of VLS. Both VLS and emphysematous bulla are more commonly seen in males and smokers and unusually both our patients were females and non-smokers. In most patients, the predominant findings on HRCT scans are extensive para septal emphysema coalescing into giant bullae. HRCT is helpful in confirming the diagnosis of VLS, assessing the degree of the disease, and providing information to guide in patient management.
Acknowledgements
The Department of Radiology & Imageology, Krishna Institute of Medical Sciences (KIMS), Secunderabad.
Conflicts of interest
The authors declare no conflicts of interest.
References
[1] Vij AS, James R, Singh A, Dhaliwal AS, Chhabra A, et al. A rare case of vanishing lung syndrome. J Assoc Physicians India. 2014; 62(12):51–53.
[2] Hashimoto M, Nakamura A, Kondo N, Hasegawa S. Successful surgical treatment for infectious giant bullae with mediastinal shift: A case report. J Case Reports Images Surg. 2016; 2:80–83.
[3] Sharma N, Justaniah AM, Kanne JP, Gurney JW, Mohammed TL. Vanishing lung syndrome (giant bullous emphysema): CT findings in 7 patients and a literature review. J Thorac Imaging. 2009; 4(3):227–230.
[4] Agarwal R, Agarwal AN. Bullous lung diseases or bullous emphysema? Respir Care. 2006; 5(5):532–534.
[5] Khasawneh FA, Nakhla EN, Karim A, Halloush RA. Vanishing lung syndrome is mistaken for bilateral spontaneous pneumothorax. BMJ Case Rep. 2013.
[6] Ahmad N, Pinelis EV, Patel P. The Case of Vanishing Lung. Chest. 2010; 138(4):133A.