Abstract
Background: Non-small cell lung carcinoma (NSCLC) is the most common form of lung cancer and a leading cause of cancer-related mortality worldwide. Immunotherapy targeting the PD-1/PD-L1 pathway has transformed the management of advanced NSCLC. PD-L1 expression, assessed through immunohistochemistry (IHC), is an important predictive biomarker for selecting patients for immune checkpoint inhibitor therapy. This study aimed to determine the prevalence of PD-L1 expression and evaluate its association with clinicopathological characteristics in NSCLC patients at a tertiary care institute in India.
Methods: This descriptive, observational, cross-sectional study included 100 histologically and IHC-confirmed NSCLC cases. PD-L1 expression was assessed on formalin-fixed paraffin-embedded tissue sections using IHC. The Tumor Proportion Score (TPS) and Combined Positive Score (CPS) were calculated. Associations between PD-L1 expression and variables such as age, sex, smoking status, histologic type, and tumor grade were analyzed using appropriate statistical methods.
Results: PD-L1 expression (TPS ≥1%) was identified in 42% of cases, of which 11% showed high expression (TPS ≥50%) and 31% showed low expression (TPS 1–49%). PD-L1 positivity was more frequent in males (42.5%), patients aged 61–70 years (45.4%), adenocarcinomas (42.5%), and non-smokers (47.6%). A statistically significant association was observed between PD-L1 expression and higher tumor grade (p = 0.029), with 57.1% of poorly differentiated tumors being PD-L1 positive compared to 31.03% of moderately differentiated tumors. No significant associations were found with age, sex, smoking status, or histologic subtype. CPS analysis identified five patients with TPS <1% but CPS ≥1, suggesting additional eligibility for immunotherapy.
Conclusion: PD-L1 expression was observed in a substantial proportion of NSCLC patients and showed a significant association with poor tumor differentiation. Incorporating PD-L1 testing using both TPS and CPS into routine diagnostic workflows is essential for optimizing immunotherapy selection and personalizing treatment strategies in advanced NSCLC.
Keywords: non-small cell lung carcinoma; PD-L1; immunohistochemistry; immunotherapy; tumor proportion score
Full Text
Introduction
Lung cancer remains the leading cause of cancer-related mortality worldwide, with an estimated 1.76 million deaths annually [1]. Non-small cell lung carcinoma (NSCLC) accounts for approximately 80–85% of all lung cancer cases [2]. The prognosis for NSCLC is often poor due to late-stage diagnosis and limited therapeutic options for advanced disease [3].
Traditional treatment modalities such as surgery, chemotherapy, and radiotherapy provide limited survival benefits in metastatic settings and are frequently associated with significant toxicity [3]. Over the past decade, the treatment landscape of NSCLC has evolved significantly with the introduction of targeted therapies and immunotherapy. Immune checkpoint inhibitors (ICIs), particularly those directed against the programmed death-1 (PD-1) receptor and its ligand, programmed death ligand-1 (PD-L1), have become central to the management of advanced NSCLC [4, 5]. The PD-1/PD-L1 pathway plays a key role in immune evasion; tumor cells expressing PD-L1 can suppress T-cell–mediated cytotoxicity, enabling unchecked tumor progression [6]. Blocking this interaction with monoclonal antibodies restores anti-tumor immunity and can produce durable clinical responses [7].
PD-L1 expression on tumor cells, assessed by immunohistochemistry (IHC), is the most widely validated predictive biomarker for response to anti-PD-1/PD-L1 therapy [8]. Expression is commonly quantified using the Tumor Proportion Score (TPS), defined as the percentage of viable tumor cells exhibiting partial or complete membranous staining [9]. Patients with high PD-L1 expression (TPS ≥50%) show significant benefit from first-line pembrolizumab monotherapy, as demonstrated in pivotal trials such as KEYNOTE-024 and KEYNOTE-042 [10, 11]. The Combined Positive Score (CPS), which includes PD-L1 staining on tumor cells and immune cells, is also gaining relevance, particularly for select immunotherapy agents and specific cancer types [12]. Despite its established clinical utility, the prevalence of PD-L1 expression and its association with clinicopathological features vary across different populations and geographic regions [13–15].
This study aims to determine the prevalence of PD-L1 expression in NSCLC patients diagnosed at our tertiary care institute in India and to assess its correlation with key clinicopathological parameters, thereby contributing real-world data to the global understanding of this important biomarker.
Materials and methods
This descriptive, observational, cross-sectional study was conducted from March 2023 to February 2024 in the Department of Pathology, SMS Medical College and Hospital, Jaipur, after obtaining approval from the Institutional Ethics Committee along with written informed consent from all participants. The study included tumor samples or lung biopsies from clinically and radiologically suspected or confirmed cases of lung carcinoma received during the study period. The sample size was estimated using a single proportion formula. Based on a previously reported PD-L1 prevalence of 45% [16], with a 95% confidence level and an absolute allowable error of 10%, the minimum required sample size was calculated to be 99, which was rounded to 100 cases.
Patients with histologically confirmed NSCLC and tissue sections showing preserved tumor morphology with at least 100 viable tumor cells were included. Participants who had provided informed consent were eligible for the study. Specimens exhibiting extensive necrosis were excluded from the analysis.
Relevant clinical information, including age, sex, smoking history, and radiological findings, was obtained from requisition forms. All tissue specimens were fixed in 10% neutral buffered formalin, routinely processed, and embedded in paraffin. Sections measuring 3–4 μm were stained with hematoxylin and eosin (H&E) for histopathological evaluation and subtyping. Immunohistochemistry (IHC) for TTF-1, p40, Napsin A, and Synaptophysin was performed when required to confirm the diagnosis and subtype of NSCLC.
PD-L1 IHC was performed on 4 μm sections using the Leica Bond Max Autostainer with the Bond Polymer DAB Detection System, employing the CAL10 clone (Master Diagnostica). PD-L1 positivity was defined as complete circumferential or partial linear membranous staining of tumor cells at any intensity. Diagnoses were established via a two-stage process: initial independent review by two pathologists, followed by a consensus meeting to resolve any discrepancies, thereby mitigating interobserver variability. Two scoring systems were applied for assessment. The Tumor Proportion Score (TPS) was calculated as the percentage of PD-L1–positive tumor cells among all viable tumor cells and categorized as follows: TPS <1% (negative), TPS 1–49% (low expression), and TPS ≥50% (high expression). The Combined Positive Score (CPS) was determined by dividing the number of PD-L1–positive tumor cells, lymphocytes, and macrophages by the total number of viable tumor cells and multiplying by 100. A CPS ≥1 was considered positive.
Statistical analysis
Statistical analysis was performed using SPSS software. Qualitative variables were expressed as proportions and percentages and analyzed using the Chi-square test. Quantitative variables were presented as mean ± standard deviation. A p-value of <0.05 was regarded as statistically significant.
Results
Baseline clinicopathological characteristics
A total of 100 patients diagnosed with NSCLC were included in the study. The baseline clinicopathological characteristics are summarized in Table 1. The cohort consisted predominantly of males (87%), with a male-to-female ratio of 6.6:1. Most patients belonged to the 61–70 years age group (44%), followed by those aged above 70 years (26%). Squamous cell carcinoma (SCC) was the most frequently observed histologic subtype, accounting for 60% of cases, while adenocarcinoma constituted 40%. A significant proportion of the patients (79%) had a history of smoking.
Table 1: Baseline clinicopathological characteristics of the study population (n = 100).
|
Characteristic
|
Category
|
Frequency (n)
|
Percentage (%)
|
|
Gender
|
Male
|
87
|
87.0
|
|
|
Female
|
13
|
13.0
|
|
Age group
|
<40 years
|
4
|
4.0
|
|
|
40-50 years
|
8
|
8.0
|
|
|
51-60 years
|
18
|
18.0
|
|
|
61-70 years
|
44
|
44.0
|
|
|
70 years
|
26
|
26.0
|
|
Histologic type
|
Adenocarcinoma
|
40
|
40.0
|
|
|
Squamous cell Carcinoma
|
60
|
60.0
|
|
Smoking status
|
Smoker
|
79
|
79.0
|
|
|
Non- Smoker
|
21
|
21.0
|
|
Histologic Grade
|
Moderately Differentiated
|
58
|
58.0
|
|
|
Poorly differentiated
|
42
|
42.0
|
Prevalence of PD-L1 expression
The distribution of PD-L1 expression based on the Tumor Proportion Score (TPS) is presented in Table 2 and Figure 1. The majority of cases (58%) were negative for PD-L1 (TPS <1%). PD-L1 positivity (TPS ≥1%) was observed in 42% of patients, of whom 31% exhibited low expression (TPS 1–49%) and 11% demonstrated high expression (TPS ≥50%).
Table 2: Distribution of PD-L1 Expression by Tumor Proportion Score (TPS).
|
PDL-1 Expression (TPS)
|
Frequency (n)
|
Percentage (%)
|
|
Negative (<1%)
|
58
|
58
|
|
Low (1-49%)
|
31
|
31
|
|
High (>=50%)
|
11
|
11
|
|
Total
|
100
|
100
|
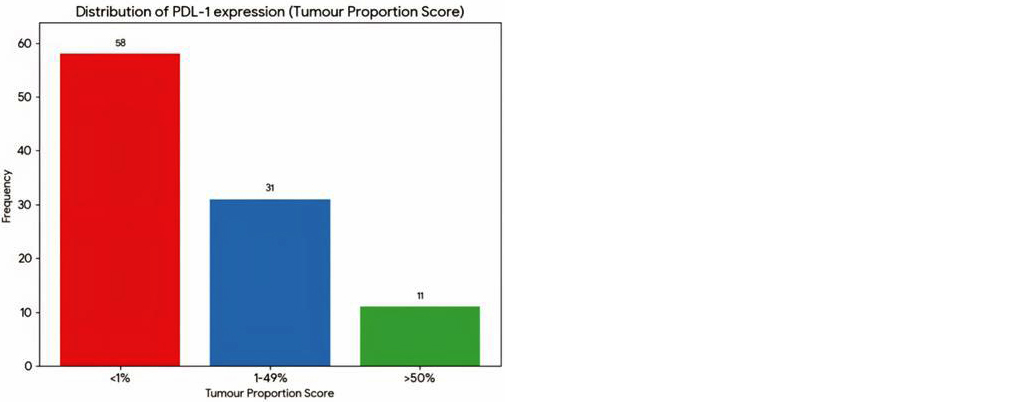
Figure 1: Bar diagram showing the distribution of PDL-1 expression by TPS.
Association of PDL-1 expression with clinicopathological parameters
The associations between PDL-1 expression (TPS) and various clinicopathological parameters are detailed in Table 3.
Table 3: Association of PDL-1 expression with clinicopathological parameters.
|
Parameter
|
Category
|
PDL-1
Negative (TPS<1%) n= 58
|
PDL-1 Low (TPS 1-49%)
n= 31
|
PDL-1 High (TPS>=50%) n= 11
|
P- value
|
|
Gender
|
Male(n= 87)
|
50(86.2%)
|
28(90.3%)
|
9(81.8%)
|
0.782
|
|
|
Female(n=13)
|
8(13.8%)
|
3(9.7%)
|
2(18.2%)
|
|
|
Age Group
|
61-70 years(n=44)
|
24(41.4%)
|
13(41.9%)
|
7(63.6%)
|
0.450
|
|
Smoking Status
|
Smoker(n=79)
|
47(81.0%)
|
24(77.4%)
|
8(72.7%)
|
0.776
|
|
|
Non smoker(n=21)
|
11(19.0%)
|
7(22.6%)
|
3(27.3%)
|
|
|
Histologic Type
|
Adenocarcinoma(n=40)
|
23(39.7%)
|
11(35.5%)
|
6(54.5%)
|
0.539
|
|
|
SCC(n= 60)
|
35(60.3%)
|
20(64.5%)
|
5(45.5%)
|
|
|
Histologic Grade
|
Moderate(n=58)
|
40(69.0%)
|
14(45.2%)
|
4(36.4%)
|
0.029
|
|
|
Poor(n=42)
|
18(31.0%)
|
17(54.8%)
|
7(63.6%)
|
|
Correlation of PD-L1 expression with clinicopathological parameters
PD-L1 expression was analyzed in relation to gender, age, smoking status, histologic type, and tumor grade. Although a higher proportion of PD-L1–positive cases was observed among males (37/87; 42.5%) and patients aged 61–70 years (20/44; 45.4%), these associations were not statistically significant (p > 0.05). Similarly, PD-L1 positivity was numerically higher in non-smokers (10/21; 47.6%) and in adenocarcinoma cases (17/40; 42.5%) when compared with smokers (32/79; 40.5%) and squamous cell carcinoma (25/60; 41.6%), but these differences did not reach statistical significance.
In contrast, a significant association was identified between PD-L1 expression and histologic grade (p = 0.029). Poorly differentiated tumors exhibited a markedly higher frequency of PD-L1 positivity (24/42; 57.1%) compared with moderately differentiated tumors (18/58; 31.03%), indicating that PD-L1 expression increases with loss of differentiation.
PD-L1 expression by combined positive score (CPS)
Assessment using the Combined Positive Score (CPS) demonstrated that 46% (46/100) of cases were PD-L1 positive (CPS ≥1). A strong correlation was observed between TPS and CPS (p = 0.000). As shown in Table 4, five patients (5%) who were negative by TPS (TPS <1%) were reclassified as PD-L1 positive based on CPS (CPS ≥1). This finding highlights an important subgroup of patients who may still be eligible for immunotherapy when CPS scoring is applied.
Table 4: Concordance between TPS and CPS Scoring (n=100).
|
TPS category
|
Total patients(n)
|
CPS positive (>=1)
|
CPS negative (<1)
|
|
<1%(Negative)
|
58
|
5(8.6%)
|
53(91.4%)
|
|
1-49%(Low)
|
31
|
30(96.8%)
|
1(3.2%)
|
|
>=50%(High)
|
11
|
11(100%)
|
0(0%)
|
The association between histologic grade and PDL-1 expression remained significant when assessed by CPS (p=0.007), with poorly differentiated tumors showing a higher proportion of CPS positivity (26/42, 61.9%) compared to moderately differentiated tumors (20/58, 34.5%).
Discussion
This cross-sectional study provides important insights into the prevalence of PD-L1 expression and its clinicopathological associations in a cohort of 100 NSCLC patients from a tertiary care center in North India.
The overall prevalence of PD-L1 expression (TPS ≥1%) observed in this study was 42%, with 11% of patients demonstrating high expression (TPS ≥50%). These findings fall within the range of previously reported global and regional prevalence rates, which show notable variability across different populations. As shown in Table 5, our prevalence is comparable to studies by Pawelczyk et al., who reported a positivity rate of 32.6% [17], Yan Jin et al., who documented 30.8% positivity [18], and recent Indian studies by Kumar et al. (57.4%) [19] and Kilaru et al. (44.7%) [21]. However, the prevalence in our cohort is lower than that reported by Dietel et al. in a large multinational cohort (52%) [22] and by Jain et al. in an Indian study (53.2%) [20].
Such differences can be attributed to multiple factors, including variations in demographic characteristics, sample size, proportions of histological subtypes, and differences in IHC platforms, antibody clones (such as 22C3, SP263, or SP142), and scoring methodologies. Inter-observer variability and the prior treatment status of patients may also contribute to the heterogeneity observed across studies.
Table 5: Comparison of PD-L1 expression prevalence with other studies.
|
Study
|
Year
|
Total Cases(n)
|
TPS1-49%
|
TPS>=50%
|
Overall >=1%
|
|
Pawelczyk et al. [17]
|
2019
|
866
|
22.3%
|
10.3%
|
32.6%
|
|
Yan Jin et al. [18]
|
2019
|
1156
|
21.1%
|
9.7%
|
30.8%
|
|
Dietel et al. [22]
|
2019
|
2368
|
30%
|
22%
|
52%
|
|
Kumar et al. [13]
|
2021
|
101
|
67.65%
|
32.35%
|
100%
|
|
Jain et al. [20]
|
2021
|
252
|
36%
|
27.6%
|
53.2%
|
|
Kumar et al. [19]
|
2021
|
327
|
37.6%
|
19.8%
|
57.4%
|
|
Kilaru et al.
|
2024
|
94
|
30.8%
|
13.8%
|
44.7%
|
|
Present study
|
2024
|
100
|
31%
|
11%
|
42%
|
*Note: Kumar et al. reported TPS<50% and ≥50%; the TPS 1-49% is derived. Dietel et al. TPS 1-49% is approximated from reported data.
In our study, PD-L1 expression demonstrated a statistically significant association with higher histologic grade (p = 0.029). Poorly differentiated tumors showed a markedly higher frequency of PD-L1 positivity (57.1%) compared with moderately differentiated tumors (31.03%). This finding is consistent with previous reports. Pawelczyk et al. [17] and Jacob et al. [16] similarly observed significantly higher PD-L1 expression in tumors of higher grade, suggesting that aggressive, poorly differentiated tumors may more frequently exploit the PD-1/PD-L1 pathway to evade immune surveillance. This correlation underscores the biological significance of PD-L1 in tumor progression and supports its potential role as a marker of aggressive disease.
In contrast to some reports [18, 19], we did not find statistically significant associations between PD-L1 expression and gender, age, smoking status, or histologic subtype (adenocarcinoma vs. squamous cell carcinoma). Although PD-L1 positivity was numerically higher in males, non-smokers, and adenocarcinoma cases, these differences did not reach statistical significance. The absence of a significant association with smoking status in our cohort, despite the predominance of smokers, aligns with findings from certain studies [20] but differs from others that report higher PD-L1 expression in smokers [18, 21]. The predominance of squamous cell carcinoma—a subtype strongly associated with smoking—and the relatively small number of non-smokers (n = 21) in our study may have influenced these observations.
A key strength of our study was the parallel assessment of PD-L1 using both TPS and CPS. We observed a strong concordance between the two scoring systems (p = 0.000). Notably, CPS identified an additional 5% of patients (5/100) as PD-L1 positive who would have been classified as negative using TPS alone (TPS <1% but CPS ≥1). This subgroup of patients, who demonstrate PD-L1 expression on infiltrating immune cells within the tumor microenvironment, may still derive benefit from immunotherapy. CPS is an established biomarker for selecting patients for certain immune checkpoint inhibitors in cancers such as gastric and urothelial carcinoma [12], and our findings highlight its potential utility in NSCLC to expand treatment eligibility. Further prospective studies are warranted to validate the clinical significance of CPS in NSCLC.
Limitations: This study has several limitations. The single-center design and relatively small sample size may limit the generalizability of the findings. As a cross-sectional study, it provides only a snapshot of PD-L1 expression without longitudinal follow-up to assess treatment response or survival outcomes. Additionally, molecular profiling for key driver mutations such as EGFR and ALK was not included, which may have provided a more comprehensive understanding of the biomarker landscape in this cohort.
Conclusion
In conclusion, this study demonstrates that PD-L1 expression is present in a substantial proportion (42%) of NSCLC patients in our region, with 11% exhibiting high expression (TPS ≥50%), making them potential candidates for first-line immunotherapy monotherapy. The significant association between PD-L1 expression and poor tumor differentiation underscores its role in tumor aggressiveness and highlights its importance as a clinically relevant biomarker. The application of CPS further identified an additional subset of patients who may benefit from immunotherapy, despite being TPS negative. These findings emphasize the need to incorporate routine PD-L1 testing—using both TPS and CPS scoring into the diagnostic evaluation of NSCLC. Such an approach is essential for optimizing treatment selection, supporting personalized therapeutic strategies, and ultimately improving clinical outcomes for patients with this challenging and often fatal disease.
Acknowledgements
We wish to sincerely acknowledge the financial support provided by DHR Multidisciplinary Research Unit of SMS Medical College Jaipur for their financial support in this study.
Conflicts of Interest
Authors declare no conflict of interests.
References
[1] Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, et al. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021; 71:209–249.
[2] Nicholson AG, Tsao MS, Beasley MB, Borczuk AC, Rossi G, et al. The 2021 WHO Classification of Lung Tumours: Impact of advances since 2015. J Thorac Oncol. 2022; 17:362–387.
[3] Lahini A, Maji A, Potdar PD, Londhe V, Chattopadhyay S. Lung cancer immunotherapy: Progress, pitfalls and promises. Mol Cancer. 2023; 22:40.
[4] Dantoing E, Piton N, Salatin M, Beltraminelli H, Schaeffer C, et al. Anti–PD1/PD–L1 immunotherapy for non–small cell lung cancer with actionable oncogenic driver mutations. Int J Mol Sci. 2021; 22:6288.
[5] Huang Z, Su W, Lu T, Zhu Y, Tian L, et al. First–line immune checkpoint inhibitors in non–small cell lung cancer: Current landscape and future progress. Front Pharmacol. 2020; 11:578091.
[6] Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer. 2012; 12:252–264.
[7] Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, et al. Safety, activity, and immune correlates of anti–PD–1 antibody in cancer. N Engl J Med. 2012; 366:2443–2454.
[8] Shukuya T, Carbone DP. Predictive markers for the efficacy of anti–PD–1/PD–L1 antibodies in lung cancer. J Thorac Oncol. 2016; 11:976–988.
[9] Incorvaia L, Fanale D, Badalamenti G, Brando C, Bono M, et al. Programmed death ligand 1 (PD–L1) as a predictive biomarker for pembrolizumab therapy in patients with advanced non–small cell lung cancer (NSCLC). Adv Ther. 2019; 36:2600–2617.
[10] Reck M, Rodríguez–Abreu D, Robinson AG, Hui R, Csoszi T, et al. Pembrolizumab versus chemotherapy for PD–L1–positive non–small–cell lung cancer. N Engl J Med. 2016; 375:1823–1833.
[11] Mok TSK, Wu YL, Kudaba I, Kowalski DM, Cho BC, et al. Pembrolizumab versus chemotherapy for previously untreated, PD–L1–expressing, locally advanced or metastatic non–small–cell lung cancer (KEYNOTE–042): A randomised, open–label, controlled, phase 3 trial. Lancet. 2019; 393:1819–1830.
[12] Kulangara K, Zhang N, Corigliano E, Morrissey C, Sheng J, et al. Clinical utility of the Combined Positive Score for programmed death ligand–1 expression and the approval of pembrolizumab for treatment of gastric cancer. Arch Pathol Lab Med. 2019; 143:330–337.
[13] Kumar M, Guleria B, Swamy S, Soni S. Correlation of programmed death ligand 1 expression with gene expression and clinicopathological parameters in Indian patients with non–small cell lung cancer. Lung India. 2020; 37:145–150.
[14] Fu F, Deng C, Sun W, Zheng H, Wei S, et al. Distribution and concordance of PD–L1 expression by routine 22C3 assays in East Asian patients with non–small cell lung cancer. Respir Res. 2022; 23:302.
[15] Ganie F, Mehfooz N, Siraj F, Rather M, Qayoom S, et al. Clinicopathological features and status of programmed death ligand 1 (PD–L1) expression in lung cancer: A single–centre study from North India. Cureus. 2023; 15:35056.
[16] Jacob S, Rajendran V, Anila KR, Thomas V, Abraham VK. Distribution and expression of programmed death ligand–1 (PD–L1) in non–small cell carcinoma of lung in a tertiary care centre in South India. Turk Patoloji Derg. 2021; 37:139–144.
[17] Pawelczyk K, Piotrowska A, Ciesielska U, Chorzalska A, Gorka J, et al. Role of PD–L1 expression in non–small cell lung cancer and its prognostic significance according to clinicopathological factors and diagnostic markers. Int J Mol Sci. 2019; 20:824.
[18] Skov BG, Rørvig SB, Jensen TH, Sørensen JB. The prevalence of programmed death ligand–1 (PD–L1) expression in non–small cell lung cancer in an unselected, consecutive population. Mod Pathol. 2020; 33:109–117.
[19] Kumar R, Narayanan S, Pai T, Lahoti C, Gulia S, et al. P33.18: The prevalence of PD–L1 expression in lung cancer—Real–world experience from a tertiary care oncology centre. J Thorac Oncol. 2021; 16:412–413.
[20] Jain E, Sharma S, Aggarwal A, Kaur R, Singh N, et al. PD–L1 expression and its clinicopathologic and genomic correlation in non–small cell lung carcinoma patients: An Indian perspective. Pathol Res Pract. 2021; 228:153497.
[21] Kilaru S, Panda SS, Moharana L, Mohanty S, Mishra S, et al. PD–L1 expression and its significance in advanced NSCLC: Real–world experience from a tertiary care centre. J Egypt Natl Canc Inst. 2024; 36:3.
[22] Dietel M, Savelov N, Salanova R, Micke P, Hofling L, et al. Real–world prevalence of programmed death ligand 1 expression in locally advanced or metastatic non–small–cell lung cancer: The global, multicenter EXPRESS study. Lung Cancer. 2019; 134:174–179.
|
Author Designations:
Aastha Sharma (Senior Resident); Ranjana Solanki (Senior Professor); Arpita Jindal (Senior Professor); Ashmeet Kaur (Senior Demonstrator).
|